Preoperative phosphorus levels may serve as a predictor of recurrent/persistent lesions after surgery for primary hyperparathyroidism: a cross-sectional study
- PMID: 40546836
- PMCID: PMC12177539
- DOI: 10.21037/gs-2025-156
Preoperative phosphorus levels may serve as a predictor of recurrent/persistent lesions after surgery for primary hyperparathyroidism: a cross-sectional study
Abstract
Background: Surgery is the definitive treatment for primary hyperparathyroidism (PHPT). However, surgical outcomes can be affected by numerous factors, some of which are still a matter of debate. We examined cases at the First Affiliated Hospital of Zhejiang University, and assessed the risk factors affecting surgical success and postoperative recurrence.
Methods: We conducted a retrospective analysis of the clinical data of patients who underwent surgery for PHPT without intraoperative parathyroid hormone (IOPTH) monitoring at the First Affiliated Hospital of Zhejiang University between August 2017 and June 2022. We analyzed the surgical success rates, recurrence rates, and persistent disease rates, and performed univariate and multivariate analyses to identify the risk factors associated with surgical success and postoperative recurrence/persistent lesions.
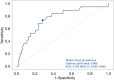
Results: The overall surgical success rate was 97.8%, and the postoperative recurrence rate was 8.2%. Univariate analysis confirmed that a higher level of preoperative parathyroid hormone (PTH) and blood calcium is associated with a lower success rate of surgery (P<0.05). However, the multivariate analysis did not reveal any significance in them. The univariate analysis identified preoperative target organ damage, urolithiasis, and preoperative alkaline phosphatase (ALP), PTH, and phosphorus levels as risk factors for postoperative recurrence/persistent lesions (P<0.05). The multivariate analysis revealed that only the phosphorus level was a significant risk factor for postoperative recurrence/persistent lesions (P<0.05). The receiver operating characteristic (ROC) curve analysis indicated that phosphorus levels below 0.865 mmol/L were associated with a higher incidence of recurrence/persistent lesions, and had a sensitivity of 0.718 and a specificity of 0.67.
Conclusions: In PHPT, satisfactory surgical success rates can be achieved without IOPTH monitoring. The blood phosphorus level is a significant predictor of postoperative recurrence or persistent lesions, and thus could guide clinical decision making.
Keywords: Primary hyperparathyroidism (PHPT); blood phosphorus; intraoperative parathyroid hormone monitoring (IOPTH monitoring); parathyroid adenoma.
Copyright © 2025 AME Publishing Company. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://gs.amegroups.com/article/view/10.21037/gs-2025-156/coif). The authors have no conflicts of interest to declare.
Figures


Similar articles
-
Signs and symptoms to determine if a patient presenting in primary care or hospital outpatient settings has COVID-19.Cochrane Database Syst Rev. 2022 May 20;5(5):CD013665. doi: 10.1002/14651858.CD013665.pub3. Cochrane Database Syst Rev. 2022. PMID: 35593186 Free PMC article.
-
Maternal and neonatal outcomes of elective induction of labor.Evid Rep Technol Assess (Full Rep). 2009 Mar;(176):1-257. Evid Rep Technol Assess (Full Rep). 2009. PMID: 19408970 Free PMC article.
-
Drugs for preventing postoperative nausea and vomiting in adults after general anaesthesia: a network meta-analysis.Cochrane Database Syst Rev. 2020 Oct 19;10(10):CD012859. doi: 10.1002/14651858.CD012859.pub2. Cochrane Database Syst Rev. 2020. PMID: 33075160 Free PMC article.
-
Taxane monotherapy regimens for the treatment of recurrent epithelial ovarian cancer.Cochrane Database Syst Rev. 2022 Jul 12;7(7):CD008766. doi: 10.1002/14651858.CD008766.pub3. Cochrane Database Syst Rev. 2022. PMID: 35866378 Free PMC article.
-
Probing for congenital nasolacrimal duct obstruction.Cochrane Database Syst Rev. 2017 Jul 12;7(7):CD011109. doi: 10.1002/14651858.CD011109.pub2. Cochrane Database Syst Rev. 2017. PMID: 28700811 Free PMC article.
References
-
- Wells SA, Jr, Leight GS, Ross AJ, 3rd. Primary hyperparathyroidism. Curr Probl Surg 1980;17:398-463. - PubMed
LinkOut - more resources
Full Text Sources
