Association between antibiotic exposure and childhood atopic dermatitis: a systematic review and meta-analysis
- PMID: 40547440
- PMCID: PMC12182308
- DOI: 10.1016/j.eclinm.2025.103296
Association between antibiotic exposure and childhood atopic dermatitis: a systematic review and meta-analysis
Abstract
Background: Antibiotics constitute a prevalent class of medications prescribed for pediatric patients. Concerns have arisen regarding the impact of early-life antibiotic use on the risk of atopic illnesses, including childhood atopic dermatitis (AD). AD affects approximately 2% of adults but is twice as prevalent in children, with rates ranging up to 4%. Therefore, the potential correlation between antibiotic exposure and childhood AD is of significant concern.
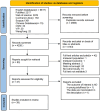
Methods: Relevant literature was searched from English databases (PubMed, Web of science, Scopus, and The Cochrane Library) and Chinese databases (CNKI database, VIP Database, Wanfang Database) to May 1, 2025. Random-effects meta-analyses were conducted to assess the association between antibiotic exposure and the risk of childhood AD. This study is registered with PROSPERO (CRD42024535141).
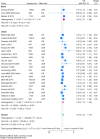
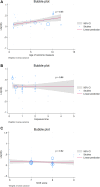
Findings: A total of 39 literature sources were included, encompassing 7,487,925 children. Meta-analysis showed that antibiotic exposure during pregnancy and childhood is associated with an increased risk of childhood AD (OR = 1.22, 95% CI: 1.17-1.28; heterogeneity: I2 = 98.06%). The subgroup analyses showed that: (1) Children exposed to antibiotics during childhood had a higher risk of developing AD compared to those exposed to antibiotics during pregnancy; (2) the increased risk of AD following antibiotic exposure was significantly affected by the diagnostic criteria and race, but not living areas; (3) antibiotic exposure frequency and type of antibiotics may contribute to the increased risk of AD following antibiotic exposure; (4) the increased risk of AD following antibiotic exposure seems to be positive related with age of outcome measure but not the age of exposure.
Interpretation: Antibiotic exposure during pregnancy or early childhood enhances AD risk, with childhood exposure posing a higher risk than prenatal exposure. Exposure time (during pregnancy and childhood) and the age at outcome measurement are important influencing factors for this association. Diagnostic criteria, race, frequency of antibiotic exposure, and type of antibiotics may also affect this relationship. While the observed statistical significance may be associated with the increased statistical power afforded by the large sample size, the clinical implications of these findings warrant cautious interpretation. Further comprehensive and high-quality studies are warranted to clarify these findings.
Funding: This work was supported by the Natural Science Foundation of Zhejiang (LYY22H310002), the Medical Science and Technology Project of Zhejiang Province (2024KY1170), Special Fund for the Incubation of Young Clinical Scientist, The Children's Hospital of Zhejiang University School of Medicine (CHZJU2023YS006).
Keywords: Antibiotic; Atopic dermatitis; Children; Eczema; Meta-analysis.
© 2025 The Author(s).
Conflict of interest statement
None.
Figures






Similar articles
-
Analgesia use during pregnancy and risk of cryptorchidism: a systematic review and meta-analysis.Hum Reprod. 2017 May 1;32(5):1118-1129. doi: 10.1093/humrep/dex047. Hum Reprod. 2017. PMID: 28333256 Free PMC article.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2017 Dec 22;12(12):CD011535. doi: 10.1002/14651858.CD011535.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2020 Jan 9;1:CD011535. doi: 10.1002/14651858.CD011535.pub3. PMID: 29271481 Free PMC article. Updated.
-
Intravenous magnesium sulphate and sotalol for prevention of atrial fibrillation after coronary artery bypass surgery: a systematic review and economic evaluation.Health Technol Assess. 2008 Jun;12(28):iii-iv, ix-95. doi: 10.3310/hta12280. Health Technol Assess. 2008. PMID: 18547499
-
Skin care interventions in infants for preventing eczema and food allergy.Cochrane Database Syst Rev. 2022 Nov 14;11(11):CD013534. doi: 10.1002/14651858.CD013534.pub3. Cochrane Database Syst Rev. 2022. PMID: 36373988 Free PMC article.
References
-
- Labib A., Ju T., Yosipovitch G. Emerging treatments for itch in atopic dermatitis: a review. J Am Acad Dermatol. 2023;89(2):338–344. - PubMed
-
- Tian J., Zhang D., Yang Y., et al. Global epidemiology of atopic dermatitis: a comprehensive systematic analysis and modelling study. Br J Dermatol. 2023;190(1):55–61. - PubMed
-
- Weidinger S., Novak N. Atopic dermatitis. Lancet. 2016;387(10023):1109–1122. - PubMed
-
- Langan S.M., Irvine A.D., Weidinger S. Atopic dermatitis. Lancet. 2020;396(10247):345–360. - PubMed
-
- Zhao H., Zhou J., Lu H., et al. Azithromycin pretreatment exacerbates atopic dermatitis in trimellitic anhydride-induced model mice accompanied by correlated changes in the gut microbiota and serum cytokines. Int Immunopharmacol. 2022;102 - PubMed
LinkOut - more resources
Full Text Sources

