Sodium-Glucose Cotransporter 2 Inhibitors, Erythrocytosis, and Thrombosis in Adults With Type 2 Diabetes
- PMID: 40549381
- PMCID: PMC12186121
- DOI: 10.1001/jamanetworkopen.2025.17086
Sodium-Glucose Cotransporter 2 Inhibitors, Erythrocytosis, and Thrombosis in Adults With Type 2 Diabetes
Abstract
Importance: Sodium-glucose cotransporter 2 inhibitors (SGLT2is) are widely used and have been shown to induce erythrocytosis. However, the clinical implications of this phenomenon, particularly its association with venous and arterial thrombotic events, remain uncertain.
Objective: To assess the extent, temporal course, and thrombotic complications of SGLT2i-induced erythrocytosis.
Design, setting, and participants: This retrospective cohort study used patient data from Israel's largest health care organization from January 1, 2015, through June 30, 2024. Adult patients aged 18 years or older with type 2 diabetes who initiated SGLT2is were identified and compared with those who initiated dipeptidyl peptidase 4 inhibitors (DPP-4is) or glucagon-like peptide 1 receptor agonists (GLP-1RAs) using a propensity score-matched, active-comparator, new-user cohort design.
Exposure: New initiation of an SGLT2i, a GLP-1RA, or a DPP-4i.
Main outcomes and measures: Outcomes included erythrocytosis within 1 year of initiating SGLT2is, as well as arterial and venous thrombotic events until the end of follow-up. Prevalence rates, rate differences, and odds ratios (ORs) for new-onset erythrocytosis and hemoglobin increase greater than 0.5 g/dL with 95% CIs were calculated. Hazard ratios (HRs) and 95% CIs for thrombotic outcomes were estimated using time-varying Cox proportional hazards regression models.
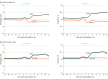
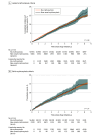
Results: After 1:1 propensity score matching, a total of 137 552 adults were included in the SGLT2i vs DPP-4i cohort (68 776 pairs; SGLT2i initiators: mean [SD] age, 64.55 [12.03] years; 55.3% male; DPP-4i initiators: mean [SD] age, 64.73 [13.08] years; 53.5% male) and 131 512 adults in the SGLT2i vs GLP-1RA cohort (65 756 pairs; SGLT2i initiators: mean [SD] age, 63.73 [11.87] years; 52.0% male; GLP-1RA initiators: mean [SD] age, 62.77 [11.56] years; 51.4% female). Among SGLT2i initiators, erythrocytosis prevalence in the SGLT2i vs DPP-4i cohort increased by 5.5% (95% CI, 5.1%-5.8%) and in the SGLT2i vs GLP-1RA cohort by 5.8% (95% CI, 5.4%-6.2%). In the SGLT2i vs GLP-1RA cohort, hemoglobin increased by 0.37 g/dL (95% CI, 0.36-0.38 g/dL) and hematocrit by 1.50% (95% CI, 1.48%-1.53%). Male sex (adjusted OR [AOR], 4.12; 95% CI, 3.80-4.48), smoking (AOR, 2.00; 95% CI, 1.85-2.16), and the use of empagliflozin vs dapagliflozin (AOR, 1.16; 95% CI, 1.09-1.25) were associated with an increased risk of developing erythrocytosis. New-onset erythrocytosis was not associated with an increased risk of myocardial infarction (HR, 0.92; 95% CI, 0.58-1.44), venous thromboembolism (HR, 1.56; 95% CI, 0.68-3.60), or stroke (HR, 1.26; 95% CI, 0.84-1.90).
Conclusions and relevance: In this cohort study of patients with type 2 diabetes, SGLT2i use was associated with a higher risk of erythrocytosis compared with DPP-4is and GLP-1RAs; however, erythrocytosis was not associated with thrombotic events. These findings provide important reassurance regarding the safety of SGLT2i-induced erythrocytosis.
Conflict of interest statement
Figures
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

