Lung parenchymal and cardiac appearances on computed tomography pulmonary angiography impact survival in chronic thromboembolic pulmonary hypertension: results from the ASPIRE Registry
- PMID: 40551799
- PMCID: PMC12183745
- DOI: 10.1183/23120541.00732-2024
Lung parenchymal and cardiac appearances on computed tomography pulmonary angiography impact survival in chronic thromboembolic pulmonary hypertension: results from the ASPIRE Registry
Abstract
Background: Chronic thromboembolic pulmonary hypertension (CTEPH) is commonly evaluated using computed tomography pulmonary angiography (CTPA). We evaluated the frequency and impact of parenchymal and cardiac abnormalities on survival in CTEPH.
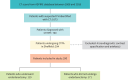
Methods: Patients were identified from the ASPIRE (Assessing the Spectrum of Pulmonary Hypertension Identified at a Referral Centre) Registry. Kaplan-Meier analysis was used to assess survival.
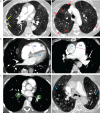
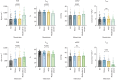
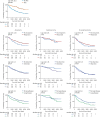
Results: 290 patients (55% female, mean±sd age 65±14 years) with CTEPH were included. Mosaic perfusion was noted in 83%, lung infarction in 73% and parenchymal lung disease in 28%. The severity of mosaic perfusion and lung infarction correlated with markers of disease severity (p<0.001). Whereas the presence of mosaic perfusion was associated with improved survival in all patients (p=0.03), it did not predict outcome in those undergoing pulmonary endarterectomy (PEA) (p=0.6) and those not undergoing PEA (p=0.22). The presence of lung infarction had no impact on mortality. The presence of co-existing lung disease was associated with a worse survival (p<0.008) in patients not undergoing PEA. Mosaic perfusion was less common in patients with parenchymal lung disease (65%) compared to those without parenchymal lung disease (90%), p<0.001. An increased right/left ventricular ratio and aortic diameter predicted a worse outcome (p<0.002).
Conclusion: Lung parenchymal and cardiac changes on CTPA predict outcome in CTEPH. Co-existing parenchymal lung disease is not uncommon and when present may mask the presence of mosaic perfusion. This study highlights the importance of systematically evaluating the lung parenchyma and cardiac changes in patients with CTEPH.
Copyright ©The authors 2025.
Conflict of interest statement
Conflict of interest: D.G. Kiely, S. Alabed and A.J. Swift are investigators within the National Institute for Health Research (NIHR) Sheffield Cardiovascular Biomedical Research Unit. A.J. Swift reports research grants and speaker fees from Janssen, the Wellcome Trust and the BHF. M. Sharkey is funded by the Wellcome Trust (223521/Z/21/Z) and NIHR Sheffield Biomedical Research Centre (NIHR203321). The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
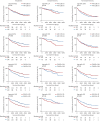
References
-
- Durrington C, Hurdman JA, Elliot CA, et al. Systematic pulmonary embolism follow-up increases diagnostic rates of chronic thromboembolic pulmonary hypertension and identifies less severe disease: results from the ASPIRE Registry. Eur Respir J 2024; 63: 2300846. doi: 10.1183/13993003.00846-2023 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
