Mucinous Cystic Neoplasms in Male Patients: Histopathological and Molecular Diagnoses
- PMID: 40558295
- PMCID: PMC12192160
- DOI: 10.3390/curroncol32060352
Mucinous Cystic Neoplasms in Male Patients: Histopathological and Molecular Diagnoses
Abstract
Cystic mucinous neoplasms (MCNs) of the pancreas are rare cystic tumors, accounting for approximately 2-5% of all pancreatic neoplasms. They predominantly occur in premenopausal women and are typically located in the body or tail of the pancreas. Due to their potential for malignant transformation, especially in cases associated with invasive carcinoma such as pancreatic ductal adenocarcinoma, early detection, complete surgical resection, and rigorous postoperative surveillance are essential. The occurrence of MCNs in male patients is exceedingly rare, comprising only about 2% of reported cases, and often resulting in preoperative diagnostic challenges. Molecular analyses have identified a strong association between KRAS mutations and disease progression in MCNs, underscoring their potential role as prognostic markers despite limited diagnostic utility. In this report, we present two additional cases of MCNs in male patients, highlighting their histopathological features and the ancillary investigations undertaken to support diagnosis.
Keywords: KRAS; case report; cystic mucinous neoplasms; cystic tumors; male; pancreas.
Conflict of interest statement
The authors declare no conflicts of interest.
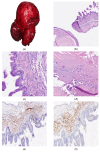
Figures




Similar articles
-
Nature and management of pancreatic mucinous cystic neoplasm (MCN): A systematic review of the literature.Pancreatology. 2016 Nov-Dec;16(6):1028-1036. doi: 10.1016/j.pan.2016.09.011. Epub 2016 Sep 20. Pancreatology. 2016. PMID: 27681503
-
Unveiling the intriguing relationship: oncogenic KRAS, morphological shifts, and mutational complexity in pancreatic mucinous cystic neoplasms.J Pathol. 2025 Apr;265(4):401-407. doi: 10.1002/path.6397. Epub 2025 Feb 5. J Pathol. 2025. PMID: 39906959 Free PMC article.
-
Management of mucinous cystic neoplasms of the pancreas.World J Gastroenterol. 2010 Dec 7;16(45):5682-92. doi: 10.3748/wjg.v16.i45.5682. World J Gastroenterol. 2010. PMID: 21128317 Free PMC article.
-
Mucinous cystic neoplasms of the pancreas and liver share a similar DNA methylation profile with mucinous ovarian tumors.J Pathol. 2025 Sep;267(1):10-24. doi: 10.1002/path.6439. Epub 2025 Jun 25. J Pathol. 2025. PMID: 40557758 Free PMC article.
-
Multiregion Genomic Analysis of Human Pancreatic Mucinous Cystic Neoplasms.Mod Pathol. 2025 Jul;38(7):100759. doi: 10.1016/j.modpat.2025.100759. Epub 2025 Mar 22. Mod Pathol. 2025. PMID: 40122523
References
-
- Nagtegaal I.D., Odze R.D., Klimstra D., Paradis V., Rugge M., Schirmacher P., Washington K.M., Carneiro F., Cree I.A., the WHO Classification of Tumours Editorial Board The 2019 WHO classification of tumours of the digestive system. Histopathology. 2020;76:182–188. doi: 10.1111/his.13975. - DOI - PMC - PubMed
-
- Kim H., Kim J.H., An J., Choi J.S. Comparison with surgically resected mucinous cystic neoplasm of pancreas and branch-duct type intraductal papillary mucinous neoplasm considering clinico-radiological high-risk features: A reassessment of current guidelines. Abdom. Imaging. 2024;49:2746–2755. doi: 10.1007/s00261-024-04364-y. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

