The Effect of Three-Dimensional Stabilization Thread Design on Biomechanical Fixation and Osseointegration in Type IV Bone
- PMID: 40558364
- PMCID: PMC12190597
- DOI: 10.3390/biomimetics10060395
The Effect of Three-Dimensional Stabilization Thread Design on Biomechanical Fixation and Osseointegration in Type IV Bone
Abstract
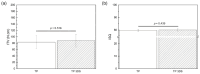
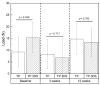
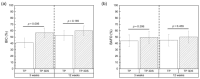
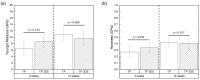
Achieving the appropriate primary stability for immediate or early loading in areas with low-density bone, such as the posterior maxilla, is challenging. A three-dimensional (3D) stabilization implant design featuring a tapered body with continuous cutting flutes along the length of the external thread form, with a combination of curved and linear geometric surfaces on the thread's crest, has the capacity to enhance early biomechanical and osseointegration outcomes compared to implants with traditional buttressed thread profiles. Commercially available implants with a buttress thread design (TP), and an experimental implant that incorporated the 3D stabilization trimmed-thread design (TP 3DS) were used in this study. Six osteotomies were surgically created in the ilium of adult sheep (N = 14). Osteotomy sites were randomized to receive either the TP or TP 3DS implant to reduce site bias. Subjects were allowed to heal for either 3 or 12 weeks (N = 7 sheep/time point), after which samples were collected en bloc (including the implants and surrounding bone) and implants were either subjected to bench-top biomechanical testing (e.g., lateral loading), histological/histomorphometric analysis, or nanoindentation testing. Both implant designs yielded high insertion torque (ITV ≥ 30 N⋅cm) and implant stability quotient (ISQ ≥ 70) values, indicative of high primary stability. Qualitative histomorphological analysis revealed that the TP 3DS group exhibited a continuous bone-implant interface along the threaded region, in contrast to the TP group at the early, 3-week, healing time point. Furthermore, TP 3DS's cutting flutes along the entire length of the implant permitted the distribution of autologous bone chips within the healing chambers. Histological evaluation at 12 weeks revealed an increase in woven bone containing a greater presence of lacunae within the healing chambers in both groups, consistent with an intramembranous-like healing pattern and absence of bone dieback. The TP 3DS macrogeometry yielded a ~66% increase in average lateral load during pushout testing at baseline (T = 0 weeks, p = 0.036) and significantly higher bone-to-implant contact (BIC) values at 3 weeks post-implantation (p = 0.006), relative to the traditional TP implant. In a low-density (Type IV) bone model, the TP 3DS implant demonstrated improved performance compared to the conventional TP, as evidenced by an increase in baseline lateral loading capacity and increased BIC during the early stages of osseointegration. These findings indicate that the modified implant configuration of the TP 3DS facilitates more favorable biomechanical integration and may promote more rapid and stable bone anchorage under compromised bone quality conditions. Therefore, such improvements could have important clinical implications for the success and longevity of dental implants placed in regions with low bone density.
Keywords: implant stability quotient; insertion torque value; lateral loading; nanoindentation; osseointegration; primary stability.
Conflict of interest statement
No conflicts of interests to declare.
Figures




Similar articles
-
Impact of three-dimensional stabilization thread design on biomechanical fixation and osseointegration of endosteal implants.J Mech Behav Biomed Mater. 2025 Aug;168:107004. doi: 10.1016/j.jmbbm.2025.107004. Epub 2025 Apr 8. J Mech Behav Biomed Mater. 2025. PMID: 40245678 Free PMC article.
-
Investigation of the expression of the C-terminal cross-linking telopeptide of type I collagen (CTXI) in saliva during early and delayed loading of dental implants.BMC Oral Health. 2025 Jul 2;25(1):1013. doi: 10.1186/s12903-025-05529-x. BMC Oral Health. 2025. PMID: 40604796 Free PMC article. Clinical Trial.
-
The impact of immediately placed and restored single-tooth implants on hard and soft tissues in the anterior maxilla.Eur J Oral Implantol. 2016;9 Suppl 1:S89-106. Eur J Oral Implantol. 2016. PMID: 27314114
-
Maximizing screw length in expandable lateral lumbar interbody spacers with integrated fixation may obviate the need for supplemental pedicle screws.Spine J. 2025 Jul;25(7):1564-1573. doi: 10.1016/j.spinee.2025.01.035. Epub 2025 Jan 30. Spine J. 2025. PMID: 39890027
-
Interventions for replacing missing teeth: different times for loading dental implants.Cochrane Database Syst Rev. 2009 Jan 21;(1):CD003878. doi: 10.1002/14651858.CD003878.pub4. Cochrane Database Syst Rev. 2009. Update in: Cochrane Database Syst Rev. 2013 Mar 28;(3):CD003878. doi: 10.1002/14651858.CD003878.pub5. PMID: 19160225 Updated.
References
-
- Lu X., Zhao Y., Peng X., Lu C., Wu Z., Xu H., Qin Y., Xu Y., Wang Q., Hao Y., et al. Comprehensive Overview of Interface Strategies in Implant Osseointegration. Adv. Funct. Mater. 2025;35:2418849. doi: 10.1002/adfm.202418849. - DOI
-
- Marão H.F., Jimbo R., Neiva R., Gil L.F., Bowers M., Bonfante E.A., Tovar N., Janal M.N., Coelho P.G. Cortical and Trabecular Bone Healing Patterns and Quantification for Three Different Dental Implant Systems. Int. J. Oral Maxillofac. Implant. 2017;32:585–592. doi: 10.11607/jomi.4856. - DOI - PubMed
-
- Stacchi C., Vercellotti T., Torelli L., Furlan F., Di Lenarda R. Changes in Implant Stability Using Different Site Preparation Techniques: Twist Drills versus Piezosurgery. A Single-Blinded, Randomized, Controlled Clinical Trial. Clin. Implant. Dent. Relat. Res. 2013;15:188–197. doi: 10.1111/j.1708-8208.2011.00341.x. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

