The Importance of Neuroimaging Follow-Up in Bilirubin-Induced Encephalopathy: A Clinical Case Review
- PMID: 40563712
- PMCID: PMC12191066
- DOI: 10.3390/brainsci15060539
The Importance of Neuroimaging Follow-Up in Bilirubin-Induced Encephalopathy: A Clinical Case Review
Abstract
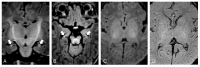
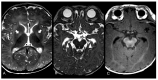
Introduction: Hyperbilirubinemia in newborns can lead to kernicterus, a severe form of neonatal encephalopathy caused by bilirubin toxicity. Despite timely interventions such as exchange transfusion, kernicterus can still develop, especially in high-risk infants. MRI is crucial for detecting early and evolving signs of bilirubin-induced brain damage. Case Report: We report a term newborn who developed severe hyperbilirubinemia and kernicterus despite receiving exchange transfusion. The infant presented on day 3 of life with jaundice, hypotonia, and feeding difficulties and had a bilirubin level of 51 mg/dL. After exchange transfusion, bilirubin levels normalized, but neurotoxicity persisted. Initial MRI at one month showed mild T1 hyperintensity in the hippocampi with no changes in the basal ganglia. At two months, T1 hyperintensities in the hippocampi partially resolved. By six months, MRI revealed T2 hyperintensities in the globus pallidus and hippocampal atrophy, consistent with kernicterus. Magnetic resonance spectroscopy (MRS) showed reduced N-acetylaspartate (NAA) levels, indicating neuronal loss. Discussion: MRI is essential in monitoring bilirubin-induced brain injury. In this case, early MRI findings showed mild hippocampal T1 hyperintensity, which resolved partially. At six months, T2 hyperintensities in the globus pallidus confirmed chronic bilirubin encephalopathy. MRS demonstrated a reduction in N-acetylaspartate, indicative of neuronal loss. Susceptibility-Weighted Imaging (SWI) showed no abnormalities, likely due to the myelination process in neonates. Conclusions: This case highlights the importance of repeated MRI in detecting bilirubin-induced brain damage. Early neuroimaging enables timely interventions and improves long-term neurodevelopmental outcomes in infants with severe hyperbilirubinemia.
Keywords: MRI; hyperbilirubinemia; kernicterus; neuroimaging; newborn.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Fluid supplementation for neonatal unconjugated hyperbilirubinaemia.Cochrane Database Syst Rev. 2017 Aug 1;8(8):CD011891. doi: 10.1002/14651858.CD011891.pub2. Cochrane Database Syst Rev. 2017. PMID: 28762235 Free PMC article.
-
Metalloporphyrins for treatment of unconjugated hyperbilirubinemia in neonates.Cochrane Database Syst Rev. 2003;(2):CD004207. doi: 10.1002/14651858.CD004207. Cochrane Database Syst Rev. 2003. PMID: 12804504
-
Periodic change of body position under phototherapy in term and preterm neonates with hyperbilirubinaemia.Cochrane Database Syst Rev. 2022 Mar 2;3(3):CD011997. doi: 10.1002/14651858.CD011997.pub2. Cochrane Database Syst Rev. 2022. PMID: 35235686 Free PMC article.
-
Sickle Cell Hepatopathy With Acute Hepatic Sequestration and Extreme Hyperbilirubinemia.Cureus. 2025 May 27;17(5):e84888. doi: 10.7759/cureus.84888. eCollection 2025 May. Cureus. 2025. PMID: 40575228 Free PMC article.
-
Controversies in our understanding of extreme hyperbilirubinemia in glucose-6-phosphate dehydrogenase-deficient neonates.Pediatr Res. 2025 Apr;97(5):1507-1515. doi: 10.1038/s41390-024-03611-8. Epub 2024 Oct 6. Pediatr Res. 2025. PMID: 39370450 Review.
References
-
- Huang M.J., Kua K.E., Teng H.C., Tang K.S., Weng H.W., Huang C.S. Risk factors for severe hyperbilirubinemia in neonates. Pediatr. Res. 2004;56:682–689. doi: 10.1203/01.PDR.0000141846.37253.AF. - DOI - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources

