Red Cell Distribution Width as a Predictive Biomarker for Early Lung Injury in Pediatric Patients Following Cardiopulmonary Bypass
- PMID: 40564743
- PMCID: PMC12191811
- DOI: 10.3390/children12060785
Red Cell Distribution Width as a Predictive Biomarker for Early Lung Injury in Pediatric Patients Following Cardiopulmonary Bypass
Abstract
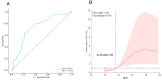
Background: Red cell distribution width (RDW) has emerged as a prognostic biomarker in various clinical contexts. This retrospective study evaluated the predictive utility of RDW for cardiopulmonary bypass-associated acute lung injury (CPB-ALI) in pediatric patients undergoing cardiac surgery. Methods: A total of 166 children were enrolled and classified into CPB-ALI and non-ALI groups. Preoperative and postoperative RDW values were analyzed. Results: Postoperative RDW was significantly higher in the CPB-ALI group (15.40% vs. 13.78%, p < 0.001). Multivariate logistic regression identified postoperative RDW as an independent predictor of CPB-ALI (OR: 1.35, 95% CI: 1.10-1.64, p = 0.003). Receiver operating characteristic analyses yielded an AUC of 0.732, and restricted cubic spline analyses revealed a nonlinear association between RDW and CPB-ALI risks (p < 0.001). Higher postoperative RDW levels were positively correlated with prolonged mechanical ventilation duration, ICU stay, and total hospital stay (p < 0.001 for all). Conclusions: These findings suggest that postoperative RDW is a cost-effective and accessible biomarker for the early identification of CPB-ALI and may inform individualized perioperative management in pediatric cardiac surgery.
Keywords: acute lung injury (ALI); biomarker; cardiopulmonary bypass (CPB); pediatric cardiac surgery; red cell distribution width (RDW).
Conflict of interest statement
The authors declare no conflicts of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
Figures

Similar articles
-
Unveiling the role of risk factors and predictive models in acute type-a aortic dissection surgery: OI downregulation and its association with immune disorders.Int J Med Sci. 2025 Jan 13;22(3):745-753. doi: 10.7150/ijms.104622. eCollection 2025. Int J Med Sci. 2025. PMID: 39898254 Free PMC article.
-
Intravenous magnesium sulphate and sotalol for prevention of atrial fibrillation after coronary artery bypass surgery: a systematic review and economic evaluation.Health Technol Assess. 2008 Jun;12(28):iii-iv, ix-95. doi: 10.3310/hta12280. Health Technol Assess. 2008. PMID: 18547499
-
Predictive ability of red blood cell distribution width for negative remodeling of type B aortic dissection.J Vasc Surg. 2025 Jul;82(1):72-79. doi: 10.1016/j.jvs.2025.03.167. Epub 2025 Mar 15. J Vasc Surg. 2025. PMID: 40096898
-
Assessing the Predictive Power of the Hemoglobin/Red Cell Distribution Width Ratio in Cancer: A Systematic Review and Future Directions.Medicina (Kaunas). 2023 Dec 5;59(12):2124. doi: 10.3390/medicina59122124. Medicina (Kaunas). 2023. PMID: 38138227 Free PMC article.
-
Platelet Indices and RDW to Assess Inflammatory Milieu in Subclinical Hashimoto's Thyroiditis.Clin Med Insights Endocrinol Diabetes. 2025 Jun 13;18:11795514251349337. doi: 10.1177/11795514251349337. eCollection 2025. Clin Med Insights Endocrinol Diabetes. 2025. PMID: 40528863 Free PMC article.
References
LinkOut - more resources
Full Text Sources

