Bispecific Antibodies in Solid Tumors: Advances and Challenges
- PMID: 40565299
- PMCID: PMC12192982
- DOI: 10.3390/ijms26125838
Bispecific Antibodies in Solid Tumors: Advances and Challenges
Abstract
Bispecific antibodies (BsAbs) have shown potential in cancer treatment and have become a rapidly growing field in cancer immunotherapy. Unlike monoclonal antibodies with two identical binding sites, BsAbs simultaneously bind two distinct epitopes on the same or different antigens, allowing for a range of mechanisms of action, including engaging immune cells to kill cancer cells and blocking signaling pathways. Despite regulatory approvals for hematological malignancies in the last decade, their clinical success in solid malignancies has been lacking until recently. There are currently five BsAbs approved by the FDA in the United States for solid tumors-amivantamab, tarlatamab, tebentafusp, zanidatamab and zenocutuzumab-and two BsAbs approved in China-cadonilimab and ivonescimab. Currently, several BsAbs are under clinical development for solid tumors, but are mostly in early phase I and II trials. This review provides an overview of the basic mechanism of action of BsAbs, current FDA-approved BsAbs, and current BsAbs under clinical development, their challenges in clinical use, the management of toxicities, and future directions.
Keywords: bispecific T cell engager; bispecific antibodies; cytokine release syndrome; personalized cancer therapy; precision medicine; targeted therapy.
Conflict of interest statement
Author Atif Hussein is a guest editor for the
Figures

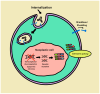
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

