Catheter-Based Therapies in Acute Pulmonary Embolism-Mortality and Safety Outcomes: A Systematic Review and Meta-Analysis
- PMID: 40565913
- PMCID: PMC12194266
- DOI: 10.3390/jcm14124167
Catheter-Based Therapies in Acute Pulmonary Embolism-Mortality and Safety Outcomes: A Systematic Review and Meta-Analysis
Abstract
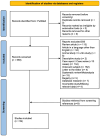
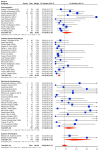
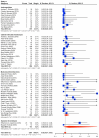
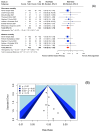
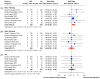
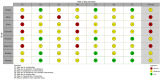
Background/Objectives: Right ventricular (RV) dysfunction and circulatory collapse are considered to play a major role in mortality in patients suffering from pulmonary embolism (PE). Catheter-based therapies (CBTs) have been shown to improve RV hemodynamics. The aim of this study was to present available data for CBTs in acute PE and investigate whether CBTs offer mortality benefit and better safety outcomes over anticoagulation (AC) in patients with intermediate-risk PE. Methods: PubMed was searched from inception until February 2024 for studies that investigated treatment strategies in patients with confirmed PE. We initially investigated the crude incidence of mortality and major bleeding for individual interventions in patients with either intermediate or high-risk PE. We then directly compared CBT to AC for intermediate-risk PE, for which the effectiveness endpoint was comparative short-term (30-day or in-hospital) and midterm (90-day or 1-year) all-cause mortality and the safety outcomes included minor bleeding, major bleeding, and intracranial hemorrhage (ICH). Results: In all, 59 studies (4457 patients) were eventually included in our study. For the prevalence study, we described the crude incidence for mortality and major bleeding for interventions like catheter-directed thrombolysis (CDT), mechanical thrombectomy (MT), AC, and systemic thrombolysis (ST) in patients with either intermediate or high-risk PE. Our data synthesis comparing CBT to AC included 1657 patients (11 studies) with intermediate-risk PE. Our results indicate that CBT is associated with a lower risk of both short-term (RR 0.43; 95% CI [0.24-0.79], I2 = 0%) and midterm all-cause mortality (RR 0.38; 95% CI [0.23-0.62], I2 = 0%) compared to AC. Major bleeding and ICH did not differ between the two groups. Conclusions: In patients with intermediate-risk PE, our meta-analysis of the current literature suggests that CBT offers better outcomes in terms of short-term and midterm mortality compared to AC alone, with no difference in safety outcomes. Further RCTs are needed to explore and validate these findings.
Keywords: acute pulmonary embolism; catheter-based therapy; catheter-directed thrombolysis; intermediate-risk pulmonary embolism; mechanical thrombectomy.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

Similar articles
-
Catheter-directed therapies for the treatment of high risk (massive) and intermediate risk (submassive) acute pulmonary embolism.Cochrane Database Syst Rev. 2022 Aug 8;8(8):CD013083. doi: 10.1002/14651858.CD013083.pub2. Cochrane Database Syst Rev. 2022. PMID: 35938605 Free PMC article.
-
Catheter-Based Interventions Have Little to No Benefit in Intermediate-Low Risk Pulmonary Embolism.J Vasc Surg. 2025 Aug 11:S0741-5214(25)01574-5. doi: 10.1016/j.jvs.2025.08.003. Online ahead of print. J Vasc Surg. 2025. PMID: 40803596
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2017 Dec 22;12(12):CD011535. doi: 10.1002/14651858.CD011535.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2020 Jan 9;1:CD011535. doi: 10.1002/14651858.CD011535.pub3. PMID: 29271481 Free PMC article. Updated.
-
Antithrombotic therapy for ambulatory patients with multiple myeloma receiving immunomodulatory agents.Cochrane Database Syst Rev. 2021 Sep 28;9(9):CD014739. doi: 10.1002/14651858.CD014739. Cochrane Database Syst Rev. 2021. PMID: 34582035 Free PMC article.
References
-
- Jaff M.R., McMurtry M.S., Archer S.L., Cushman M., Goldenberg N., Goldhaber S.Z., Jenkins J.S., Kline J.A., Michaels A.D., Thistlethwaite P., et al. Management of Massive and Submassive Pulmonary Embolism, Iliofemoral Deep Vein Thrombosis, and Chronic Thromboembolic Pulmonary Hypertension. Circulation. 2011;123:1788–1830. doi: 10.1161/CIR.0b013e318214914f. - DOI - PubMed
-
- Konstantinides S.V., Meyer G., Becattini C., Bueno H., Geersing G.-J., Harjola V.-P., Huisman M.V., Humbert M., Jennings C.S., Jiménez D., et al. 2019 ESC Guidelines for the Diagnosis and Management of Acute Pulmonary Embolism Developed in Collaboration with the European Respiratory Society (ERS) Eur. Heart J. 2020;41:543–603. doi: 10.1093/eurheartj/ehz405. - DOI - PubMed
-
- Kuo W.T., Sista A.K., Faintuch S., Dariushnia S.R., Baerlocher M.O., Lookstein R.A., Haskal Z.J., Nikolic B., Gemmete J.J. Society of Interventional Radiology Position Statement on Catheter-Directed Therapy for Acute Pulmonary Embolism. J. Vasc. Interv. Radiol. 2018;29:293–297. doi: 10.1016/j.jvir.2017.10.024. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

