A Structured Narrative Review of the OSA-T2DM Axis
- PMID: 40565914
- PMCID: PMC12194640
- DOI: 10.3390/jcm14124168
A Structured Narrative Review of the OSA-T2DM Axis
Abstract
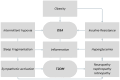
Background/Objectives: Obstructive sleep apnea (OSA) and type 2 diabetes mellitus (T2DM) are two highly prevalent and interconnected conditions with significant implications for morbidity and mortality. Emerging evidence suggests a bidirectional relationship between the two disorders, mediated by shared pathophysiological mechanisms such as intermittent hypoxia, systemic inflammation, and autonomic dysfunction. Methods: A structured narrative review of the literature was conducted using a comprehensive PubMed search of clinical and observational studies published between 2020 and 2024. Studies evaluating the association between OSA and diabetes, including its effects on glycemic control, diabetic complications, and treatment outcomes, were included. Results: Thirty-three studies met our inclusion criteria. OSA is independently associated with impaired glucose metabolism, increased insulin resistance, and a higher risk of diabetic complications, including nephropathy, retinopathy, and neuropathy. Continuous positive airway pressure (CPAP) therapy has shown variable effects on metabolic outcomes, largely dependent on adherence. Traditional OSA severity metrics, such as the apnea-hypopnea index (AHI), did not consistently predict metabolic burden. Factors such as sleep quality, nocturnal hypoxemia, and comorbid insomnia have emerged as the most relevant predictors. Sex-specific differences and the roles of pharmacological and behavioral interventions were also noted. Conclusions: OSA is a modifiable and under-recognized risk factor for poor glycemic control and diabetes complications. Routine screening and individualized treatment strategies are warranted, particularly for patients with T2DM and suboptimal metabolic control. Future research should focus on defining the phenotypes at the greatest risk and developing integrated treatment pathways.
Keywords: OSAS; T2DM; diabetes mellitus; obstructive sleep apnea; sleep disorders.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures


Similar articles
-
Drug therapy for obstructive sleep apnoea in adults.Cochrane Database Syst Rev. 2006 Apr 19;(2):CD003002. doi: 10.1002/14651858.CD003002.pub2. Cochrane Database Syst Rev. 2006. Update in: Cochrane Database Syst Rev. 2013 May 31;(5):CD003002. doi: 10.1002/14651858.CD003002.pub3. PMID: 16625567 Updated.
-
Practice parameters for the surgical modifications of the upper airway for obstructive sleep apnea in adults.Sleep. 2010 Oct;33(10):1408-13. doi: 10.1093/sleep/33.10.1408. Sleep. 2010. PMID: 21061864 Free PMC article.
-
Adherence to continuous positive airway pressure for the treatment of obstructive sleep apnea in neurodegenerative diseases: A systematic review.Sleep Med Rev. 2023 Oct;71:101836. doi: 10.1016/j.smrv.2023.101836. Epub 2023 Aug 9. Sleep Med Rev. 2023. PMID: 37586145
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
-
Twelve-Month CPAP Therapy Modulates BDNF Levels in Patients with Severe Obstructive Sleep Apnea: Implications for Metabolic and Treatment Compliance.Int J Mol Sci. 2025 Jun 18;26(12):5855. doi: 10.3390/ijms26125855. Int J Mol Sci. 2025. PMID: 40565316 Free PMC article.
References
-
- Zhang J., Zhan Q., Deng Z., Lin L., Feng Z., He H., Zhang D., Zhao H., Gu X., Yin X., et al. Does diabetes modify the triglyceride-glucose index associated with cardiovascular events and mortality? A meta-analysis of 50 cohorts involving 7,239,790 participants. Cardiovasc. Diabetol. 2025;24:42. doi: 10.1186/s12933-025-02585-z. - DOI - PMC - PubMed
-
- Rottenkolber M., Gar C., Then C., Wanger L., Sacco V., Banning F., Potzel A.L., Kern-Matschilles S., Nevinny-Stickel-Hinzpeter C., Grallert H., et al. A Pathophysiology of Type 2 Diabetes Unrelated to Metabolic Syndrome. J. Clin. Endocrinol. Metab. 2021;106:1460–1471. doi: 10.1210/clinem/dgab057. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

