Stand-Alone Lateral Lumbar Interbody Fusion at L3-L4 with 3D-Printed Porous Titanium Cages: A Safe and Effective Alternative in the Treatment of Degenerative Disc Disease (DDD)
- PMID: 40565978
- PMCID: PMC12193929
- DOI: 10.3390/jcm14124233
Stand-Alone Lateral Lumbar Interbody Fusion at L3-L4 with 3D-Printed Porous Titanium Cages: A Safe and Effective Alternative in the Treatment of Degenerative Disc Disease (DDD)
Abstract
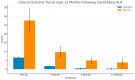
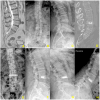
Background/Objectives: Stand-alone lateral lumbar interbody fusion (LLIF) remains a debated approach in spinal surgery, with limited published evidence supporting its efficacy without supplemental fixation. This prospective study presents the institutional case series on single-level L3-L4 stand-alone LLIF, using next-generation 3D-printed titanium cages, as treatment for degenerative disc disease (DDD). Methods: A cohort of 49 patients with symptomatic DDD, unresponsive to conservative therapy, underwent stand-alone LLIF at L3-L4 (neither posterior pedicle screws nor lateral plating). Clinical outcomes (VAS and ODI) and radiological parameters (disc height, segmental/lumbar lordosis) were collected preoperatively and at 1, 6, and 12 months. Repeated-measures ANOVA with Bonferroni correction was adopted for statistical analysis. Results: Significant improvements were observed in pain and disability scores at all time points, with the mean VAS score decreasing from 6.53 to 0.29, and ODI from 27.6% to 3.84% at one year (p < 0.001). Radiographic analysis confirmed durable increases in disc height and segmental lordosis. Solid fusion was achieved in 97.9% of cases. No patient required posterior revision; transient neurological symptoms were mild and self-limiting. Conclusions: This study demonstrates that stand-alone LLIF at L3-L4 is safe and effective in achieving stable fusion and clinical-radiological improvement. These results challenge the necessity of supplemental fixation and support the broader adoption of a less invasive fusion paradigm.
Keywords: LLIF; degenerative disc disease; fusion; intervertebral disc; low back pain; minimally invasive spine surgery; spine.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
References
-
- Zheng J., Song Y., Yu B. GPNMB Suppresses Inflammation and Extracellular Matrix Degradation in Nucleus Pulposus Cells by Inhibiting Pro-Inflammatory Cytokine Production and Activation of the NF-κB Signaling Pathway. J Interferon Cytokine Res. 2025;45:238–246. doi: 10.1089/jir.2025.0022. - DOI - PubMed
-
- Schmidt H., Reitmaier S., Yang D., Duda G., Pumberger M. Degenerative relationships in lumbar intervertebral discs and facet joints: An MRI-based comparative study of asymptomatic individuals and patients with chronic and intermittent low back pain. Front. Bioeng. Biotechnol. 2025;13:1502082. doi: 10.3389/fbioe.2025.1502082. - DOI - PMC - PubMed
-
- Genitiempo M., Perna A., Santagada D.A., Meluzio M.C., Proietti L., Bocchi M.B., Logroscino C.A., Tamburrelli F.C. Single-level Bryan cervical disc arthroplasty: Evaluation of radiological and clinical outcomes after 18 years of follow-up. Eur. Spine J. 2020;29:2823–2830. doi: 10.1007/s00586-020-06486-5. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

