The Pathophysiology of Cardiac Troponin Release and the Various Circulating Cardiac Troponin Forms-Potential Clinical Implications
- PMID: 40565986
- PMCID: PMC12194301
- DOI: 10.3390/jcm14124241
The Pathophysiology of Cardiac Troponin Release and the Various Circulating Cardiac Troponin Forms-Potential Clinical Implications
Abstract
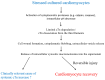
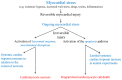
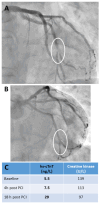
Current routine high-sensitivity cardiac troponin assays are the criterion standard for the laboratory diagnosis of myocardial injury due to their high analytical sensitivity and specificity. However, in daily clinical practice, unexpectedly elevated cardiac troponin test results without an obvious clinical correlate are becoming more frequent compared with previous cardiac troponin assay generations. In these patients, myocardial injury may sometimes be undetected by imaging techniques, including cardiac magnetic resonance imaging. This has led to an increased interest in the pathophysiology of cardiac troponin release, particularly with regard to whether troponin can be released in the absence of myocardial necrosis and thereby resulting in an increase in cardiac troponin in the systemic circulation. Although there is in vitro evidence that cardiac biomarkers are released from reversibly injured cultured cardiomyocytes, there is still a lack of evidence for cardiac troponin release apart from different forms of cell death (i.e., apoptosis or necrosis) in animal experiments. Conversely, various circulating cardiac troponin forms have been identified in human blood samples using different analytical methods, raising the question of whether the cause of myocardial injury can be reliably determined by measuring specific circulating cardiac troponin forms. Preliminary clinical data suggests that testing for specific circulating troponin forms could increase the specificity of cardiac troponin for diagnosing acute myocardial infarctions caused by an acute coronary syndrome. This review aims to provide an up-to-date overview of these current cardiac troponin research topics with their potential clinical implications. Typical clinical cases illustrate how to interpret cTn in the individual patient and how to derive a correct diagnosis.
Keywords: acute myocardial infarction; cardiac troponin; circulating troponin forms; myocardial injury; pathophysiology; release.
Conflict of interest statement
The author reports research collaboration on cardiac biomarker point-of-care diagnostics with Siemens Healthineers, The Netherlands.
Figures
Similar articles
-
Assessing the comparative effects of interventions in COPD: a tutorial on network meta-analysis for clinicians.Respir Res. 2024 Dec 21;25(1):438. doi: 10.1186/s12931-024-03056-x. Respir Res. 2024. PMID: 39709425 Free PMC article. Review.
-
A rapid and systematic review of the clinical effectiveness and cost-effectiveness of paclitaxel, docetaxel, gemcitabine and vinorelbine in non-small-cell lung cancer.Health Technol Assess. 2001;5(32):1-195. doi: 10.3310/hta5320. Health Technol Assess. 2001. PMID: 12065068
-
Surveillance of Barrett's oesophagus: exploring the uncertainty through systematic review, expert workshop and economic modelling.Health Technol Assess. 2006 Mar;10(8):1-142, iii-iv. doi: 10.3310/hta10080. Health Technol Assess. 2006. PMID: 16545207
-
Effectiveness and safety of vitamin D in relation to bone health.Evid Rep Technol Assess (Full Rep). 2007 Aug;(158):1-235. Evid Rep Technol Assess (Full Rep). 2007. PMID: 18088161 Free PMC article.
-
Cost-effectiveness of using prognostic information to select women with breast cancer for adjuvant systemic therapy.Health Technol Assess. 2006 Sep;10(34):iii-iv, ix-xi, 1-204. doi: 10.3310/hta10340. Health Technol Assess. 2006. PMID: 16959170
References
-
- Thygesen K., Mair J., Katus H., Plebani M., Venge P., Collinson P., Lindahl B., Giannitsis E., Hasin Y., Galvani M., et al. Study Group on Biomarkers in Cardiology of the ESC Working Group on Acute Cardiac Care; Recommendations for the use of cardiac troponin measurement in acute cardiac care. Eur. Heart J. 2010;31:2197–2204. doi: 10.1093/eurheartj/ehq251. - DOI - PubMed
-
- Thygesen K., Mair J., Giannitsis E., Mueller C., Lindahl B., Blankenberg S., Huber K., Plebani M., Biasucci L.M., Tubaro M., et al. The Study Group on Biomarkers in Cardiology of the ESC Working group on Acute Cardiac Care; How to use high-sensitivity cardiac troponins in acute cardiac care. Eur. Heart J. 2012;33:2252–2257. doi: 10.1093/eurheartj/ehs154. - DOI - PubMed
-
- Thygesen K., Alpert J.S., Jaffe A.S., Chaitman B.R., Bax J.B., Morrow D.A., White H.D. Executive Group on behalf of the Joint European Society of Cardiology (ESC)/American College of Cardiology (ACC)/American Heart Association (AHA)/World Heart Federation (WHF) Task Force for the Universal Definition of Myocardial Infarction. Fourth universal definition of myocardial infarction (2018) Eur. Heart J. 2019;40:237–269.
Publication types
LinkOut - more resources
Full Text Sources

