The Prevalence and Risk Factors of Residual Back Pain After Vertebroplasty for Osteoporotic Vertebral Compression Fractures: A Systematic Review and Meta-Analysis
- PMID: 40571423
- PMCID: PMC12318695
- DOI: 10.1111/os.70095
The Prevalence and Risk Factors of Residual Back Pain After Vertebroplasty for Osteoporotic Vertebral Compression Fractures: A Systematic Review and Meta-Analysis
Abstract
Background: Osteoporotic vertebral compression fractures (OVCFs) are prevalent among the elderly. Percutaneous vertebroplasty (PVA) is a commonly adopted minimally invasive treatment, yet many patients endure residual back pain (RBP) posttreatment, affecting their recovery and quality of life. Given the inconsistent prevalence of RBP across studies and the multitude of influencing factors, a systematic review and meta-analysis is necessary to determine its prevalence and identify risk factors.
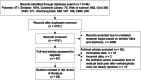
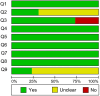
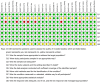
Methods: English (PubMed, Embase, Web of Science, Ovid, Cochrane Library) and Chinese (CNKI, WanFang Data, VIP, CBM) literature databases were systematically searched until December 31, 2023. A random-effects meta-analysis was used to pool prevalence rates from individual studies. The associations between the identified risk factors and RBP were also analyzed. Sensitivity and subgroup analyzes were performed to identify the source of heterogeneity and to compare the prevalence estimates across the groups. The Joanna Briggs Institute's (JBIs) quality assessment checklist was used to evaluate the quality of the included studies. The I2 tests were used to assess heterogeneity among the studies.
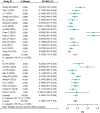
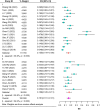
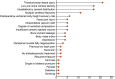
Results: A total of 5146 articles were collected. Finally, 26 articles involving 9703 participants were included. Among them, 1245 experienced RBP. The prevalence of RBP in individual studies ranged from 4.56% to 50.00%, with a median of 14.90%. The pooled prevalence was 16.3% (95% CI: 13.5%-19.1%). The prevalence was higher among females [16.1% (95% CI: 13.1%-19.1%)] than males [15.9% (95% CI: 12.5%-19.2%)]. Subgroup analysis based on evaluation time showed that the prevalence was higher at 3 months or more after surgery [total: 17.3% (95% CI: 13.2%-21.4%) vs. 15.7% (95% CI: 12.1%-19.2%), males: 16.5% (95% CI: 12.3%-20.6%) vs. 15.3% (95% CI: 11.0%-19.6%), females: 16.9% (95% CI: 12.6%-21.1%) vs. 15.5% (95% CI: 11.6%-19.5%)]. Regarding the risk factors, several factors demonstrated significant associations with RBP. Patients with low pre-bone mineral density were more likely to experience RBP compared to those with higher density. Moreover, thoracolumbar fascia injury, unsatisfactory cement distribution, multiple vertebral fractures, and postoperative vertebral body height recovery rate were also identified as risk factors increasing the likelihood of RBP.
Conclusion: RBP is common after PVA, indicating the imperative of intervention strategies to alleviate the suffering and reduce negative ramifications. Moreover, various risk factors should be comprehensively considered to accurately assess patients' conditions and formulate targeted treatment and rehabilitation plans to alleviate patients' RBP symptoms.
Keywords: meta‐analysis; osteoporotic vertebral compression fractures; percutaneous vertebroplasty; residual back pain; systematic review.
© 2025 The Author(s). Orthopaedic Surgery published by Tianjin Hospital and John Wiley & Sons Australia, Ltd.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures


Similar articles
-
Prevalence and risk factors for residual back pain after percutaneous vertebral augmentation in osteoporotic vertebral compression fracture patients: a systematic review and meta-analysis.BMC Musculoskelet Disord. 2025 Jun 2;26(1):541. doi: 10.1186/s12891-025-08731-8. BMC Musculoskelet Disord. 2025. PMID: 40457319 Free PMC article.
-
What Risk Factors Are Associated With Recurrent Osteoporotic Vertebral Compression Fractures After Percutaneous Vertebral Augmentation? A Meta-analysis.Clin Orthop Relat Res. 2025 Feb 26;483(8):1528-1539. doi: 10.1097/CORR.0000000000003430. Clin Orthop Relat Res. 2025. PMID: 40036060
-
Percutaneous vertebroplasty and percutaneous balloon kyphoplasty for the treatment of osteoporotic vertebral fractures: a systematic review and cost-effectiveness analysis.Health Technol Assess. 2014 Mar;18(17):1-290. doi: 10.3310/hta18170. Health Technol Assess. 2014. PMID: 24650687 Free PMC article.
-
Incidence and prognostic factors of residual back pain in patients treated for osteoporotic vertebral compression fractures: a systematic review and meta-analysis.Eur Spine J. 2024 Dec;33(12):4521-4537. doi: 10.1007/s00586-024-08426-z. Epub 2024 Aug 6. Eur Spine J. 2024. PMID: 39103616
-
Percutaneous vertebroplasty for osteoporotic vertebral compression fracture.Cochrane Database Syst Rev. 2015 Apr 30;(4):CD006349. doi: 10.1002/14651858.CD006349.pub2. Cochrane Database Syst Rev. 2015. Update in: Cochrane Database Syst Rev. 2018 Apr 04;4:CD006349. doi: 10.1002/14651858.CD006349.pub3. PMID: 25923524 Updated.
References
-
- Das L., Laway B. A., Sahoo J., et al., “Bone Mineral Density, Turnover, and Microarchitecture Assessed by Second‐Generation High‐Resolution Peripheral Quantitative Computed Tomography in Patients With Sheehan's Syndrome,” Osteoporosis International 35, no. 5 (2024): 919–927. - PubMed
-
- Livingstone S. J., Guthrie B., Mcminn M., et al., “Derivation and Validation of the CFracture Competing Risk Fracture Prediction Tool Compared With QFracture in Older People and People With Comorbidity: A Population Cohort Study,” Lancet Healthy Longevity 4, no. 1 (2023): e43–e53. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

