Risk Factors and Prognosis of Polymyxin- and Carbapenem-Resistant Enterobacteriaceae Infections: A Propensity-Matched Real-World Study
- PMID: 40572145
- PMCID: PMC12194920
- DOI: 10.3390/microorganisms13061256
Risk Factors and Prognosis of Polymyxin- and Carbapenem-Resistant Enterobacteriaceae Infections: A Propensity-Matched Real-World Study
Abstract
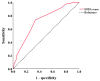
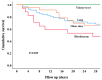
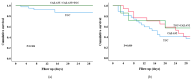
The risk factors and prognosis of polymyxin- and carbapenem-resistant Enterobacteriaceae (PR-CRE) infections were analyzed to reduce their incidence and concurrently improve patient prognosis. This retrospective study analyzed patients with CRE infections admitted to West China Hospital of Sichuan University between 1 September 2019 and 30 September 2023. Based on polymyxin susceptibility, the cases were categorized into PR-CRE and PS-CRE (polymyxin-susceptible CRE) groups, with 1:1 propensity score matching performed between the two cohorts. Comprehensive data, including demographic characteristics, laboratory findings, antibiotic regimens, and clinical outcomes, were collected and analyzed to identify risk factors for PR-CRE infections and evaluate treatment efficacy. This study aims to provide evidence-based references for infection control strategies and antimicrobial stewardship in managing PR-CRE infections. A total of 254 patients were included in this study, with 127 patients in the PR-CRE group. The sensitivity rates of isolates in the PR-CRE group to tigecycline and ceftazidime-avibactam were 94.4% and 88.9%, respectively. Multivariate analysis identified chronic organic disease (OR 2.747, 95% CI 1.303-5.789; p = 0.008) and the use of polymyxin ≥ 3 days (OR 19.203, 95% CI 7.126-51.752; p < 0.001) as independent risk factors for PR-CRE infection. Moreover, ceftazidime-avibactam-based regimens were superior to tigecycline-based regimens for the treatment of PR-CRE infections (71.43% vs. 58.46%), especially in critically ill patients (33.33% vs. 58.82%). Finally, a SOFA score ≥ 5.5 (HR 6.718, 95% CI 2.526-17.866; p < 0.001) was identified as an independent risk factor for 28-day mortality in patients with PR-CRE infection. The presence of chronic organic diseases and the use of polymyxin for ≥3 days were identified as independent risk factors associated with PR-CRE infections in hospitalized patients, highlighting the need to optimize polymyxin use. Furthermore, the efficacy of ceftazidime-avibactam-based regimens may be superior to tigecycline-based regimens for the treatment of PR-CRE infections.
Keywords: carbapenem-resistant Enterobacteriaceae; polymyxin; prognosis; risk factors.
Conflict of interest statement
The authors declare no conflicts of interest. Consent for publication: All authors read and approved the final manuscript.
Figures
Similar articles
-
Ceftazidime-avibactam versus polymyxins in treating patients with carbapenem-resistant Enterobacteriaceae infections: a systematic review and meta-analysis.Infection. 2024 Feb;52(1):19-28. doi: 10.1007/s15010-023-02108-6. Epub 2023 Oct 25. Infection. 2024. PMID: 37878197 Free PMC article.
-
Improved diagnostic stewardship in carbapenem-resistant Enterobacterales gene detection helps in early initiation of targeted therapy.J Med Microbiol. 2025 Jun;74(6):002029. doi: 10.1099/jmm.0.002029. J Med Microbiol. 2025. PMID: 40540319 Free PMC article.
-
Antibiotics for ventilator-associated pneumonia.Cochrane Database Syst Rev. 2016 Oct 20;10(10):CD004267. doi: 10.1002/14651858.CD004267.pub4. Cochrane Database Syst Rev. 2016. PMID: 27763732 Free PMC article.
-
Clinical outcomes and the impact of treatment modalities in children with carbapenem-resistant Enterobacteriaceae bloodstream infections: a retrospective cohort study from a tertiary university hospital.J Antimicrob Chemother. 2025 Jan 3;80(1):147-153. doi: 10.1093/jac/dkae387. J Antimicrob Chemother. 2025. PMID: 39475360 Free PMC article.
-
Tigecycline Treatment for Carbapenem-Resistant Enterobacteriaceae Infections: A Systematic Review and Meta-Analysis.Medicine (Baltimore). 2016 Mar;95(11):e3126. doi: 10.1097/MD.0000000000003126. Medicine (Baltimore). 2016. PMID: 26986165 Free PMC article.
References
-
- Anyanwu M.U., Jaja I.F., Okpala C.O.R., Njoga E.O., Okafor N.A., Oguttu J.W. Mobile Colistin Resistance (mcr) Gene-Containing Organisms in Poultry Sector in Low- and Middle-Income Countries: Epidemiology, Characteristics, and One Health Control Strategies. Antibiotics. 2023;12:1117. doi: 10.3390/antibiotics12071117. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

