HPV Vaccination Knowledge and Decision-Making Among Adults 27 to 45 Years: A Large Online Survey
- PMID: 40575452
- PMCID: PMC12198051
- DOI: 10.1002/lio2.70182
HPV Vaccination Knowledge and Decision-Making Among Adults 27 to 45 Years: A Large Online Survey
Abstract
Objective: Understand knowledge and barriers to human papillomavirus (HPV) vaccination among United States (US) adults, comparing adults in the original age cohort of 18-26 years to those in the expanded 27-45-yearyear-old cohort.
Methods: A cross-sectional survey was administered to US adults recruited through social media. Descriptive statistics characterized the data. Multivariate logistic regression identified factors associated with vaccination.
Results: Among 1735 respondents, the majority were in the 27-45 age group (936, 53.94%). The 27-45-year group exhibited more knowledge of HPV's link to head and neck cancer and vaccine protection but expressed less concern about HPV infection (all p < 0.05). Key motivators for the history of vaccination in the 27-45 year cohort included vaccine effectiveness (48.65%) and prior knowledge (42.44%). Self-vaccination rates were comparable across age groups (18-26: 70.62% vs. 27-45: 68.07%, p = 0.256). Older adults were less likely to vaccinate dependents (68.57% vs. 75.00%, p < 0.001) despite higher interest (p < 0.001). Main barriers for unvaccinated 27-45 year old adults included scheduling issues, insurance coverage, and lack of concern for HPV infection (all p < 0.05). Among individuals aged 27 to 45, multivariate logistic regression analysis revealed significantly higher odds of vaccination in those from the Western US (compared to Northeast/Midwest) (OR 3.15, 95% CI: [1.84, 5.39]) and personal history of head and neck cancer (3.01, [1.78-5.09]).
Conclusion: Most respondents understand HPV risks and are vaccinated. Interventions directed towards education about vaccine safety, the hazards of HPV, and improving access may increase vaccination.
Level of evidence: IV.
Keywords: Gardasil; HPV; HPV vaccination; patient knowledge; treatment decision making.
© 2025 The Author(s). Laryngoscope Investigative Otolaryngology published by Wiley Periodicals LLC on behalf of The Triological Society.
Conflict of interest statement
The authors declare no conflicts of interest.
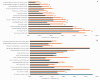
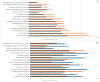
Figures

Similar articles
-
Prophylactic vaccination against human papillomaviruses to prevent cervical cancer and its precursors.Cochrane Database Syst Rev. 2018 May 9;5(5):CD009069. doi: 10.1002/14651858.CD009069.pub3. Cochrane Database Syst Rev. 2018. PMID: 29740819 Free PMC article.
-
Face-to-face interventions for informing or educating parents about early childhood vaccination.Cochrane Database Syst Rev. 2018 May 8;5(5):CD010038. doi: 10.1002/14651858.CD010038.pub3. Cochrane Database Syst Rev. 2018. PMID: 29736980 Free PMC article.
-
Factors affecting caregivers' HPV vaccination decisions for adolescent girls: A secondary analysis of a Chinese RCT.PLoS One. 2025 Jun 17;20(6):e0324260. doi: 10.1371/journal.pone.0324260. eCollection 2025. PLoS One. 2025. PMID: 40526724 Free PMC article. Clinical Trial.
-
Coverage of HPV Vaccination and Influencing Factors Among Female College Students in Northern China.Vaccines (Basel). 2025 May 31;13(6):598. doi: 10.3390/vaccines13060598. Vaccines (Basel). 2025. PMID: 40573929 Free PMC article.
-
Interventions targeted at women to encourage the uptake of cervical screening.Cochrane Database Syst Rev. 2021 Sep 6;9(9):CD002834. doi: 10.1002/14651858.CD002834.pub3. Cochrane Database Syst Rev. 2021. PMID: 34694000 Free PMC article.
References
LinkOut - more resources
Full Text Sources
Research Materials
