Epidemiological trends of influenza A and B in one hospital in Chengdu and national surveillance data (2019-2024)
- PMID: 40575488
- PMCID: PMC12198144
- DOI: 10.3389/fcimb.2025.1603369
Epidemiological trends of influenza A and B in one hospital in Chengdu and national surveillance data (2019-2024)
Abstract
Background: Influenza A (Flu A) and Influenza B (Flu B) are major contributors to seasonal epidemics, causing significant morbidity and mortality worldwide. Understanding their epidemiological trends is essential for optimizing prevention and control strategies.
Objective: This study aims to analyze the epidemiological trends of Flu A and Flu B, compare hospital-based and national surveillance data, and evaluate the impact of COVID-19 on influenza transmission to provide scientific evidence for influenza control measures.
Methods: We analyzed influenza positivity rates from Sichuan Jinxin Xinan Women and Children Hospital data (HD) and Chinese National Influenza Center (CNIC) between 2019 and 2024. Temporal trends, subtype distributions, and the effects of non-pharmaceutical interventions (NPIs) were assessed.
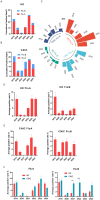
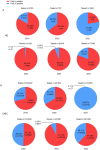
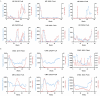
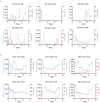
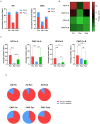
Results: Influenza activity exhibited significant temporal variations. In HD, the highest cumulative positivity rate of Flu A + Flu B was observed in 2023 (31.9%), whereas the lowest rate occurred during the COVID-19 pandemic (2020-2022), with a nadir in 2021 (2.0%). Flu A remained the predominant subtype in HD except in 2021, whereas CNIC data showed a relatively higher proportion of Flu B. Weekly positivity rates displayed distinct seasonal trends in CNIC data but not in HD. A comparative analysis of pre-pandemic (2019), pandemic (2020-2022), and post-pandemic (2023-2024) phases indicated that NPIs had a stronger suppressive effect on Flu A than on Flu B.
Conclusion: Hospital-based and national influenza surveillance data showed heterogeneity in subtype proportions, seasonal trends, and pandemic-related impacts. These findings underscore the importance of integrating multiple surveillance sources for a comprehensive understanding of influenza dynamics. Enhancing vaccine coverage, implementing targeted public health interventions, and optimizing resource allocation are crucial for mitigating the influenza burden in the post-pandemic era.
Keywords: COVID-19; epidemiology; influenza A; influenza B; non-pharmaceutical interventions.
Copyright © 2025 Li, Yang, Chen, Ma and Hu.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- Alexander M. E., Bowman C., Moghadas S. M., Summers R., Gumel A. B., Sahai B. M.. (2004). A vaccination model for transmission dynamics of influenza. SIAM J. Appl. Dynamical Syst. 3, 503–524. doi: 10.1137/030600370 - DOI
-
- Caini S., Kroneman M., Wiegers T., El Guerche-Séblain C., Paget J. (2018). Clinical characteristics and severity of influenza infections by virus type, subtype, and lineage: a systematic literature review. Influenza Other Respir. Viruses 12, 780–792. doi: 10.1111/irv.2018.12.issue-6 - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

