Rates of Depression in Children and Adolescents With ADHD: A Systematic Review and Meta-Analysis
- PMID: 40577247
- PMCID: PMC12318167
- DOI: 10.1177/10870547251341597
Rates of Depression in Children and Adolescents With ADHD: A Systematic Review and Meta-Analysis
Abstract
Objective: Accumulating evidence indicates high rates of major depressive disorder (MDD) in children and adolescents with ADHD. This systematic review and meta-analysis aimed to examine the rate of depression in children and adolescents with ADHD who are without intellectual disability (ID).
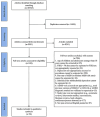
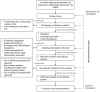
Method: A comprehensive search of six databases identified 20,745 studies. After screening based on inclusion and exclusion criteria, 24 studies were retained. A meta-analysis estimated the pooled depression rate in this population, and subgroup analyses examined differences based on sex, pubertal status, ADHD medication use, recruitment settings, depression assessment tools, informants, and risk of bias rating. Depression rates in children and adolescents with ADHD were compared with neurotypical peers in the retained case-control studies.
Results: Depression rates in children and adolescents with ADHD across the included studies ranged from 1.7% to 60%, with the meta-analysis estimating a pooled depression rate of 11.31% (95% CI [0.07, 0.16]). Subgroup analyses indicated significant differences by sex, with females showing higher rates than males. Differences were also noted by assessment methods, with the highest rates observed when both questionnaires and interviews were used. While other factors did not significantly affect rates, notable trends were identified and reported in the current article.
Conclusion: Depression is a common co-occurrent psychiatric condition in children and adolescents with ADHD, with rates observed in this review and meta-analysis being higher than those reported for neurotypical children and adolescents. This review underscores the importance of combining multiple assessment methods to capture a comprehensive picture of depression in this population, as well as ensuring balanced demographic representation. This review also suggests that further research should explore the depression developmental patterns in children and adolescents with ADHD and identify whether patterns are similar to the neurotypical population.
Keywords: ADHD; adolescents; children; co-occurrence; depression; rate.
Conflict of interest statement
Declaration of Conflicting InterestsThe author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures


Similar articles
-
Methylphenidate for children and adolescents with attention deficit hyperactivity disorder (ADHD).Cochrane Database Syst Rev. 2015 Nov 25;2015(11):CD009885. doi: 10.1002/14651858.CD009885.pub2. Cochrane Database Syst Rev. 2015. Update in: Cochrane Database Syst Rev. 2023 Mar 27;3:CD009885. doi: 10.1002/14651858.CD009885.pub3. PMID: 26599576 Free PMC article. Updated.
-
Methylphenidate for children and adolescents with autism spectrum disorder.Cochrane Database Syst Rev. 2017 Nov 21;11(11):CD011144. doi: 10.1002/14651858.CD011144.pub2. Cochrane Database Syst Rev. 2017. PMID: 29159857 Free PMC article.
-
Parent training interventions for Attention Deficit Hyperactivity Disorder (ADHD) in children aged 5 to 18 years.Cochrane Database Syst Rev. 2011 Dec 7;2011(12):CD003018. doi: 10.1002/14651858.CD003018.pub3. Cochrane Database Syst Rev. 2011. PMID: 22161373 Free PMC article.
-
Amphetamines for attention deficit hyperactivity disorder (ADHD) in children and adolescents.Cochrane Database Syst Rev. 2016 Feb 4;2(2):CD009996. doi: 10.1002/14651858.CD009996.pub2. Cochrane Database Syst Rev. 2016. PMID: 26844979 Free PMC article.
-
Methylphenidate for attention deficit hyperactivity disorder (ADHD) in children and adolescents - assessment of adverse events in non-randomised studies.Cochrane Database Syst Rev. 2018 May 9;5(5):CD012069. doi: 10.1002/14651858.CD012069.pub2. Cochrane Database Syst Rev. 2018. PMID: 29744873 Free PMC article.
References
-
- Achenbach T. M., Rescorla L. A. (2001). Manual for ASEBA school-age forms & profiles. University of Vermont, Research Center for Children, Youth & Families.
-
- American Psychiatric Association. (1994). Diagnostic and statistical manual of mental disorders (4th ed.). American Psychiatric Publishing, Inc.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

