Risk of gastric cancer after bariatric surgery: a meta-analysis of retrospective studies
- PMID: 40585478
- PMCID: PMC12202535
- DOI: 10.3389/fsurg.2025.1573430
Risk of gastric cancer after bariatric surgery: a meta-analysis of retrospective studies
Abstract
Objectives: As obesity rates rise and Bariatric & Metabolic surgery (MBS) becomes more common, many patients with obesity opt for these procedures. Despite this, there are still concerns regarding the risk of postoperative gastric cancer. This study reviews comparative studies on the risk of gastric gancer among MBS vs. non MBS patients, reported in the last 15 years.
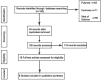
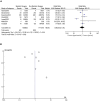
Methods and study design: We conducted literature searches on PubMed, Web of Science, and Cochrane Library using specifically formulated terms and limited the publication period to 2000 to 2024. The number of people in the literature who underwent MBS and those who developed gastric cancer after MBS were extracted and statistically analyzed using RevMan 5.3. A random-effects model was employed to determine the merged odds ratio (OR) values, with the Mantel-Haenszel estimation method. Publication bias was assessed using a funnel plot. Heterogeneity between studies was analyzed with the Cochran Q (Chi-square) test and I² statistics.
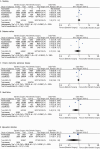
Results: A total of nine studies reported the incidence of gastric cancer, with a total of 1,025,852 patients with obesity in the MBS group and 7,171,376 patients with obesity in the matched control group. After excluding the confounding factors commonly associated with gastric cancer in the included studies, we found that the incidence rate of gastric cancer was comparable for parents after MBS and patients with obesity (OR = 0.98, 95% CI 0.50-1.94, P = 0.96) in meta-analysis.
Conclusions: It appears that there is no significant difference in the risk of gastric cancer between patients with obesity who have undergone MBS and those who have not, further investigation is needed to define the long term risk. Consequently, concerns can be reduced in patients with obesity who are in urgent need of MBS but are worried about developing gastric cancer. It provides evidence-based medicine evidence for clinical treatment.
Keywords: bariatric and metabolic surgery MBS; gastric cancer; meta-analysis; review; systermatic review.
© 2025 Li, Li, Peng and Zhang.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures



Similar articles
-
Maternal and neonatal outcomes of elective induction of labor.Evid Rep Technol Assess (Full Rep). 2009 Mar;(176):1-257. Evid Rep Technol Assess (Full Rep). 2009. PMID: 19408970 Free PMC article.
-
Electronic cigarettes for smoking cessation.Cochrane Database Syst Rev. 2022 Nov 17;11(11):CD010216. doi: 10.1002/14651858.CD010216.pub7. Cochrane Database Syst Rev. 2022. Update in: Cochrane Database Syst Rev. 2024 Jan 8;1:CD010216. doi: 10.1002/14651858.CD010216.pub8. PMID: 36384212 Free PMC article. Updated.
-
Sertindole for schizophrenia.Cochrane Database Syst Rev. 2005 Jul 20;2005(3):CD001715. doi: 10.1002/14651858.CD001715.pub2. Cochrane Database Syst Rev. 2005. PMID: 16034864 Free PMC article.
-
Electronic cigarettes for smoking cessation.Cochrane Database Syst Rev. 2021 Sep 14;9(9):CD010216. doi: 10.1002/14651858.CD010216.pub6. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 Nov 17;11:CD010216. doi: 10.1002/14651858.CD010216.pub7. PMID: 34519354 Free PMC article. Updated.
-
Prophylactic non-steroidal anti-inflammatory drugs for the prevention of macular oedema after cataract surgery.Cochrane Database Syst Rev. 2016 Nov 1;11(11):CD006683. doi: 10.1002/14651858.CD006683.pub3. Cochrane Database Syst Rev. 2016. PMID: 27801522 Free PMC article.
References
Publication types
LinkOut - more resources
Full Text Sources
Research Materials

