Beyond surgical radicality in intramedullary spinal cord metastases: neurological function and systemic disease burden drive patient outcomes
- PMID: 40587076
- PMCID: PMC12367927
- DOI: 10.1007/s11060-025-05119-5
Beyond surgical radicality in intramedullary spinal cord metastases: neurological function and systemic disease burden drive patient outcomes
Abstract
Purpose: Intramedullary spinal cord metastases (ISCM) are rare, clinically challenging lesions with limited evidence-based guidance. Optimal surgical management remains controversial, particularly regarding the ideal extent of resection (EOR) and associated prognostic factors. This study systematically evaluates perioperative outcomes, neurological function, and short-term survival according to biopsy-only, subtotal, or gross total resection (GTR) approaches.
Methods: This retrospective single-center study included 16 patients treated surgically for histologically confirmed ISCM between 2015 and 2024. Patients were stratified by surgical extent (biopsy, subtotal, or total resection). Outcomes included perioperative complications, neurological function, and 90-day survival. A literature review of surgical ISCM series (≥ 5 cases) was also performed.
Results: Sixteen patients with a median age of 59 years (56% male) were included. Thoracic lesions predominated (56%). Surgical complications were seen in 19% of the cases, however no irreversible neurological injury and no intraoperative mortality or transfusion occured. Early mortality was lowest following GTR (13%) compared to subtotal (60%) or biopsy-only (33%) approaches (p = 0.015). However, multivariable regression showed that EOR alone was not independently predictive of short-term survival (p = 0.834), indicating patient selection bias. Neurological function remained stable or improved in all of cases, irrespective of resection extent.
Conclusion: Surgical management of ISCM can be performed safely with minimal neurological morbidity, achieving symptom stabilization or improvement. Although GTR was associated with favorable short-term survival, systemic disease burden and postoperative neurological function are stronger prognostic factors. Therefore, surgical decisions should prioritize functional preservation and patient selection based on disease extent and overall health.
Keywords: Extent of resection; ISCM; Intramedullary metastases; Neurosurgical oncology; Spinal metastases.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate/publish: This retrospective analysis of ISCM patients was approved by the local Ethics Committee in accordance with the Declaration of Helsinki. Explicit consent to participate from each patient was not available due to the retrospective study design and many patients of the cohort had already deceased. Competing interests: The authors declare no competing interests.
Figures

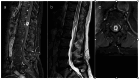
References
-
- Isla A, Paz JM, Sansivirini F, Zamora P, Garcia Grande A, Fernandez A (2000) Intramedullary spinal cord metastasis. A case report. J Neurosurg Sci 44:99–101 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

