Progressive coronary stenosis detected by intraoperative TEE after acute type-A aortic dissection repair: a case report
- PMID: 40593248
- PMCID: PMC12214222
- DOI: 10.1186/s40981-025-00802-y
Progressive coronary stenosis detected by intraoperative TEE after acute type-A aortic dissection repair: a case report
Abstract
Background: Acute type-A aortic dissection is a life-threatening condition requiring urgent intervention. Among its complications, coronary malperfusion is particularly fatal. Although rare, coronary artery stenosis after surgical repair is critical yet underrecognized.
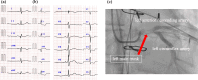
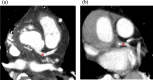
Case presentation: A 77-year-old man underwent emergency aortic arch replacement for acute type-A aortic dissection. Intraoperative transesophageal echocardiography (TEE) initially showed no coronary involvement. However, ST-segment elevation and new hypokinesia appeared post-repair. TEE identified progressive left main coronary artery stenosis. Coronary angiography confirmed severe stenosis, leading to urgent coronary artery bypass grafting. The patient recovered well and was discharged on postoperative day 33.
Conclusions: This case highlights the importance of intraoperative TEE for early detection of coronary complications following acute type-A aortic dissection repair. Dissection can progress even after aortic replacement surgery and requires vigilance. Careful monitoring and prompt intervention are crucial to optimize the outcome of these rare but life-threatening events.
Keywords: Acute type-A aortic dissection; Coronary artery stenosis; Transesophageal echocardiography.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: Not applicable. Consent for publication: Written informed consent was obtained from the patient for publication of this case report. Competing interests: The authors declare that they have no competing interests.
Figures

References
LinkOut - more resources
Full Text Sources
