A prospective study on incidence of desaturations in ERCP with non-anesthesiologist sedation and adverse event awareness of endoscopists
- PMID: 40594061
- PMCID: PMC12217398
- DOI: 10.1038/s41598-025-04922-4
A prospective study on incidence of desaturations in ERCP with non-anesthesiologist sedation and adverse event awareness of endoscopists
Abstract
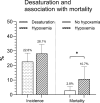
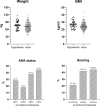
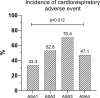
Little is known of the desaturation rate among NAPS (non-anesthesiological/nurse-administered propofol-sedation) ERCPs (endoscopic retrograde cholangiopancreatography) and endoscopists` awareness of overall incidence of adverse events (AEs). The primary aims were to assess desaturation rates and endoscopists` AE-awareness. In this prospective observation study, all ERCPs performed in a certain period were included. Nurses documented hypoxemia and measures taken to correct it. Charts were reviewed for clinical data. Definitions of AEs were based on the 2020 ESGE guidelines. Of 232 included ERCPs, 218 (94%) were conducted using NAPS. Mean age was 67.9 (SD 15.8) years, 53.2% were female, median ASA status was 2 (IQR 2;3). Most (86.8%) procedures were started on 2 L O2 flow/min (via nasal cannula), propofol mono-sedation was used in 98.2%. A desaturation occurred in 22.6% (n = 45) of procedures, and 28.1% (n = 56), when including interventions performed for hypoxemia. Risk factors for desaturations were higher BMI, and higher ASA status (p < 0.05). Documentation of AEs by endoscopists was exceptionally low. Only 22.2% of post-ERCP pancreatitis, 19% of intraprocedural bleeding, 20% of desaturations were officially recorded/documented. All-cause 30-day mortality was significantly higher in the desaturation group (10.7% vs. 2.8%, p = 0.03). Sedation-AEs are common and desaturation is statistically significantly associated with 30-day-mortality. Incidence of complications is underappreciated by endoscopists.
Keywords: Adverse events; ERCP; Endoscopic retrograde cholangiopancreatography; Hypoxemia; Nurse-administered propofol sedation (NAPS); Sedation-related complications.
© 2025. The Author(s).
Conflict of interest statement
Competing interests: The authors declare no competing interests.
Figures
References
-
- Wehrmann, T. et al. S3-Leitlinie „Sedierung in der gastrointestinalen Endoskopie“ der Deutschen Gesellschaft für Gastroenterologie, Verdauungs- und Stoffwechselkrankheiten (DGVS). Z Gastroenterol61(9), 1246–1301 (2023). - PubMed
-
- Dumonceau, J. M. et al. Non-anesthesiologist administration of propofol for gastrointestinal endoscopy: European society of gastrointestinal endoscopy, European society of gastroenterology and endoscopy nurses and associates guideline-updated June 2015. Endoscopy47(12), 1175–1189 (2015). - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

