Associations between serum uric acid related ratios and the onset of metabolic dysfunction associated steatotic liver disease
- PMID: 40594823
- PMCID: PMC12215300
- DOI: 10.1038/s41598-025-07986-4
Associations between serum uric acid related ratios and the onset of metabolic dysfunction associated steatotic liver disease
Abstract
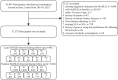
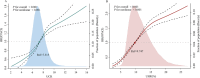
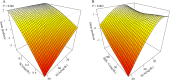
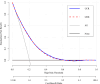
To investigate the relationship between SUA-related ratios [the SUA-to-creatinine ratio (UCR) and the SUA-to-high-density lipoprotein cholesterol ratio (UHR)] and the risk of new-onset metabolic dysfunction-associated steatotic liver disease (MASLD) prospectively. In this study, data from 37,575 patients from the Dalian Health Management Cohort (DHMC) were analysed. A restricted cubic spline was used to analyse the nonlinear relationship between the SUA-related ratios and MASLD. Generalized additive mixed models were used to evaluate the interaction of SUA with SCr and HDL-C levels. Cox proportional risk modelling was used to explore the relationships between SUA-related ratios and MASLD scores. Results were validated through subgroup and sensitivity analyses. Receiver operating characteristic curves and decision curve analysis evaluated predictive utility. During follow-up (mean 3.20 years), 891 (2.37%) developed lean MASLD and 7,043 (18.74%) nonlean MASLD. Higher UCR and UHR were associated with greater cumulative risk (log-rank test P = 0.001). Each 1.0-SD increase in UCR and UHR conferred 23% (HR: 1.23, 95%CI: 1.21-1.26) and 28% (HR: 1.28, 95%CI: 1.24-1.33) greater MASLD risk, respectively. Nonlinear relationships were observed (Pnonlinearity<0.001). The results of the ROC curves indicate C statistics of 0.773 and 0.769, respectively, with the incorporation of UCR and UHR into the base model. Elevated UCR and UHR independently predict MASLD incidence, demonstrating utility for risk stratification in both lean and nonlean populations.
Keywords: Generalized additive model; Metabolic dysfunction-associated steatotic liver disease; The serum uric acid to creatinine ratio; The serum uric acid to high-density lipoprotein cholesterol ratio.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study was conducted in accordance with both the Declaration of Helsinki and Istanbul and was approved by the Ethics Committee of the Second Affiliated Hospital of Dalian Medical University (approval number: 2022064). A waiver of signed informed consent was granted on the basis of the approval of the ethics committee for this study. Competing interests: The authors declare no competing interests.
Figures

References
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

