Comparison of efficacy and safety between surgical and conservative treatments for hemorrhoids: a meta-analysis
- PMID: 40596934
- PMCID: PMC12211330
- DOI: 10.1186/s12876-025-04089-2
Comparison of efficacy and safety between surgical and conservative treatments for hemorrhoids: a meta-analysis
Abstract
Objectives: Hemorrhoids, a common anorectal condition, can be managed through surgical or conservative treatments. The aim of this meta-analysis is to compare the efficacy and safety of surgical and conservative treatments for hemorrhoids.
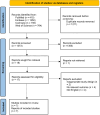
Methods: A systematic search was conducted from of PubMed, Embase, the Cochrane Library, and Web of Science from their inception to September 25, 2024. Eligible studies compared surgical treatments with non-invasive conservative treatments in hemorrhoids. Statistical analyses included pooled odds ratios (ORs) and mean differences (MDs)/standard mean differences (SMDs) with 95% confidence intervals (CIs).
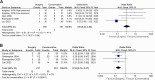
Results: Seven studies, including 760 patients, were analyzed. Surgery achieved higher rates of complete symptom resolution than conservative therapy (OR = 2.96, 95% CI: 1.66-5.28, p < 0.001). Overall pain scores favored surgery (SMD = -0.93, 95% CI: 1.73 to -0.13, p = 0.02). Subgroup analysis showed clear superiority within four days (SMD = -1.26, 95% CI -1.84 to -0.68) but parity beyond ten days (SMD = 0.00, 95% CI -0.44 to 0.44; p = 0.99). Comparable patterns were observed in pregnant women with thrombosed external hemorrhoids. Rates of postoperative bleeding (OR: 1.09; 95% CI: 0.42 to 2.82, p = 0.86; I2 = 41%, p = 0.15) and urinary retention (OR: 1.75; 95% CI: 0.30 to 10.31, p = 0.54; I2 = 45%, p = 0.18) did not differ significantly between groups. Surgical-specific adverse events were infrequent (incontinence 3%, persistent pain 5%, watery discharge 6%). Surgery shortened recovery in pregnant thrombosed cases by approximately seven days (MD: -6.80; 95% CI: -7.64 to -5.96, p < 0.001; I2 = 55%, p = 0.14) and reduced overall recurrence (95% CI: 0.10 to 0.37, p < 0.001; I2 = 0%, p = 0.97).
Conclusion: Surgical treatments provide superior symptom relief, faster recovery, and lower recurrence but with some specific post-treatment complications, while conservative treatments are safer and less invasive but with provides slower symptom relief and higher recurrence rates. Individualized treatment should consider symptom severity, patient preferences, and risk tolerance.
Keywords: Conservative treatment; Hemorrhoids; Meta-Analysis; Surgical treatment.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: Not applicable. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures

Similar articles
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
-
Selective progesterone receptor modulators (SPRMs) for uterine fibroids.Cochrane Database Syst Rev. 2017 Apr 26;4(4):CD010770. doi: 10.1002/14651858.CD010770.pub2. Cochrane Database Syst Rev. 2017. PMID: 28444736 Free PMC article.
-
Conservative, physical and surgical interventions for managing faecal incontinence and constipation in adults with central neurological diseases.Cochrane Database Syst Rev. 2024 Oct 29;10(10):CD002115. doi: 10.1002/14651858.CD002115.pub6. Cochrane Database Syst Rev. 2024. PMID: 39470206
-
Single-incision sling operations for urinary incontinence in women.Cochrane Database Syst Rev. 2017 Jul 26;7(7):CD008709. doi: 10.1002/14651858.CD008709.pub3. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2023 Oct 27;10:CD008709. doi: 10.1002/14651858.CD008709.pub4. PMID: 28746980 Free PMC article. Updated.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2017 Dec 22;12(12):CD011535. doi: 10.1002/14651858.CD011535.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2020 Jan 9;1:CD011535. doi: 10.1002/14651858.CD011535.pub3. PMID: 29271481 Free PMC article. Updated.
References
-
- Hawkins AT, et al. The American society of Colon and rectal surgeons clinical practice guidelines for the management of hemorrhoids. Dis Colon Rectum. 2024;67(5):614–23. - PubMed
-
- Pata F, et al. Anatomy, physiology and pathophysiology of haemorrhoids. Rev Recent Clin Trials. 2021;16(1):75–80. - PubMed
-
- Devi V, et al. Hemorrhoid disease: A review on treatment, clinical research and patent data. Infect Disord Drug Targets. 2023;23(6):e270423216271. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

