Comparison of tidal volume and airway pressure during neonatal resuscitation in mask leaks
- PMID: 40599049
- PMCID: PMC12215236
- DOI: 10.1111/ped.70139
Comparison of tidal volume and airway pressure during neonatal resuscitation in mask leaks
Abstract
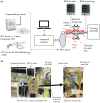
Background: Providing positive-pressure ventilation (PPV) to the lungs is essential for neonatal resuscitation. Accurate PPV requires a precise measurement of tidal volume and airway pressure, with airway obstruction and mask leakage being the primary concerns for ineffective ventilation. This study aimed to investigate the differences between tidal volume and airway pressure measured by a respiratory function monitor (RFM) and the actual values delivered to the lungs in scenarios involving mask leaks, using a system comprising a PPV device, a face mask, and an artificial lung model.
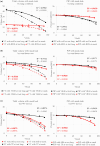
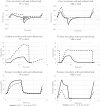
Methods: Three experiments were conducted to assess mask leakage (1) under varying lung conditions, (2) under different ventilation rates, and (3) using different PPV devices. Two RFMs were used, one in the test lung and the other in the mask. Trends in those data were assessed by means of a correlation graph.
Results: Mask leakage resulted in an underestimation of the actual tidal volume, with the effect intensifying as the leak percentage increased. PPV devices using a compressed gas source demonstrated less reduction in lung tidal volume (from 15 to 12 mL) owing to mask leaks compared with those without such a source (from 16 to 5 mL).
Conclusions: Significant discrepancies were observed between RFM readings and test lung values for tidal volume. These findings highlight the importance of accurate monitoring to prevent lung injury caused by excessive tidal volume, particularly in the presence of mask leaks. Accurately measuring tidal volume in the presence of mask leaks presents a significant challenge for the future.
Keywords: infant newborn; positive‐pressure respiration; resuscitation.
© 2025 The Author(s). Pediatrics International published by John Wiley & Sons Australia, Ltd on behalf of Japan Pediatric Society.
Conflict of interest statement
Fumihiko Takatori (First author) is an employee of Nihon Kohden. No financial support for this study was received from Nihon Kohden.
Figures
Similar articles
-
Nasal interfaces for neonatal resuscitation.Cochrane Database Syst Rev. 2023 Oct 3;10(10):CD009102. doi: 10.1002/14651858.CD009102.pub2. Cochrane Database Syst Rev. 2023. PMID: 37787113 Free PMC article.
-
Laryngeal mask airway versus bag-mask ventilation or endotracheal intubation for neonatal resuscitation.Cochrane Database Syst Rev. 2018 Mar 15;3(3):CD003314. doi: 10.1002/14651858.CD003314.pub3. Cochrane Database Syst Rev. 2018. PMID: 29542112 Free PMC article.
-
Tidal volume delivery during chest compression with either an endotracheal tube or supraglottic airway in a porcine animal model.Eur J Pediatr. 2025 Jul 8;184(8):470. doi: 10.1007/s00431-025-06312-4. Eur J Pediatr. 2025. PMID: 40624444
-
Non-invasive ventilation for cystic fibrosis.Cochrane Database Syst Rev. 2017 Feb 20;2(2):CD002769. doi: 10.1002/14651858.CD002769.pub5. Cochrane Database Syst Rev. 2017. PMID: 28218802 Free PMC article.
-
Impact of neonatal noninvasive resuscitation strategies on lung mechanics, tracheal pressure, and tidal volume in preterm lambs.Am J Physiol Lung Cell Mol Physiol. 2024 Aug 1;327(2):L203-L217. doi: 10.1152/ajplung.00236.2022. Epub 2024 May 21. Am J Physiol Lung Cell Mol Physiol. 2024. PMID: 38771135 Free PMC article.
References
-
- Ersdal HL, Mduma E, Svensen E, Perlman JM. Early initiation of basic resuscitation interventions including face mask ventilation may reduce birth asphyxia related mortality in low‐income countries. A prospective descriptive observational study. Resuscitation. 2012;83(7):869–873. 10.1016/j.resuscitation.2011.12.011 - DOI - PubMed
-
- Wyckoff MH, Wyllie J, Aziz K, de Almeida MF, Fabres J, Fawke J, et al. Neonatal life support: 2020 international consensus on cardiopulmonary resuscitation and emergency cardiovascular care science with treatment recommendations. Circulation. 2020;142:185–221. - PubMed
-
- Schmölzer GM, Dawson JA, Kamlin COF, O'Donnell CPF, Morley CJ, Davis PG. Airway obstruction and gas leak during mask ventilation of preterm infants in the delivery room. Arch Dis Child Fetal Neonatal Ed. 2011;96(4):1–4. - PubMed
-
- Schmölzer GM, Kamlin OCOF, O'Donnell CPF, Dawson JA, Morley CJ, Davis PG. Assessment of tidal volume and gas leak during mask ventilation of preterm infants in the delivery room. Arch Dis Child Fetal Neonatal Ed. 2010. Nov;95(6):F43–F46. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

