Mapping the colorectal cancer patient journey in Egypt: A qualitative study of diagnosis, treatment, and lifestyle perspectives
- PMID: 40601685
- PMCID: PMC12220998
- DOI: 10.1371/journal.pone.0326144
Mapping the colorectal cancer patient journey in Egypt: A qualitative study of diagnosis, treatment, and lifestyle perspectives
Abstract
Background: Colorectal cancer (CRC) in Egypt presents a significant public health challenge, ranking as the 7th most common cancer and the 8th leading cause of cancer deaths. Understanding patients' experiences is crucial to inform tailored screening and supportive care. This study aims to explore Egyptian CRC patients' experiences of diagnoses, treatment, and perceptions of a healthy diet and physical activity.
Methods: Utilizing the Social Ecological Model (SEM) as a theoretical framework, we conducted one-hour, face-to-face, semi-structured interviews with 19 CRC patients in Alexandria, Egypt, between August and September 2023. Audio recorded interviews were transcribed and analyzed thematically to identify patterns across individual, interpersonal, organizational, social context (culture/community), and policy levels of the SEM.
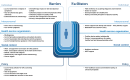
Results: The participants, 12 males and 7 females with a mean age of 54.8 (±10.2) years, predominantly came from low-income backgrounds, with the majority being either unemployed (47.4%) or disabled (31.6%). We identified facilitators and barriers to optimal care at several levels of the SEM. The main barriers were as follows: lack of awareness, symptom neglect, fear and embarrassment of colonoscopy, limited diet and activity from chemotherapy and colostomy, job loss, and poverty (individual); peers fear of colonoscopy and judgment (interpersonal); misdiagnosis, inadequate patient education, and lack of structured diet and activity programs (health organization); unsupportive work environments, cultural and religious beliefs, health literacy, and cancer stigma (social context); and unclear screening policies, lack of equipment, lack of insurance, high costs, and limited rural healthcare (policy). The main facilitators were faith resilience and positive perceptions of diet and activity (individual); family and friend support (interpersonal); positive doctor-patient relationships (health organization); NGO support (social context); and free healthcare at university hospitals (policy).
Conclusion: The study highlights the complex interplay of barriers and facilitators CRC patients encounter throughout their experience with cancer. The findings emphasize the need for improved awareness, education, support systems; enhanced healthcare access; and targeted policy changes, especially in rural areas, to improve early diagnosis, treatment outcomes, and patient quality of life.
Copyright: This is an open access article, free of all copyright, and may be freely reproduced, distributed, transmitted, modified, built upon, or otherwise used by anyone for any lawful purpose. The work is made available under the Creative Commons CC0 public domain dedication.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
References
-
- Siegel RL, et al. Colorectal cancer statistics, 2020. CA Cancer J Clin. 2020;70(3):145–64. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical