Is the use of standardized patients more effective than role-playing in medical education? A meta-analysis
- PMID: 40606465
- PMCID: PMC12214434
- DOI: 10.3389/fmed.2025.1601116
Is the use of standardized patients more effective than role-playing in medical education? A meta-analysis
Abstract
Aim: This study aimed to compare the effectiveness of using Standardized patients (SPs) and Role-playing (RP) in medical education. It is crucial to understand the differences in the effects of SPs and RP. However, the existing measurement results are varied, and the findings lack robustness.
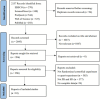
Methods: We collected the results of various experiments and conducted a meta-analysis. In total, 10 articles and 27 effect sizes were included in the analysis, involving 721 students.
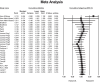
Results: The meta-analysis results showed that compared to the RP method, using SPs significantly improved students' self-confidence (effect size = 0.415). However, in other aspects, the two methods showed similar outcomes. We observed that the effectiveness of SPs teaching methods increased over time.
Conclusion: SPs effectively enhance students' self-confidence by simulating diverse roles, situations, and real-world work scenarios. This study provides a comprehensive comparative perspective on RP and SPs.
Keywords: clinical simulation; medical education; meta-analysis; role-playing; standardized patients.
Copyright © 2025 Xiao and Fu.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
-
Interventions to improve hearing aid use in adult auditory rehabilitation.Cochrane Database Syst Rev. 2016 Aug 18;2016(8):CD010342. doi: 10.1002/14651858.CD010342.pub3. Cochrane Database Syst Rev. 2016. PMID: 27537242 Free PMC article.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2017 Dec 22;12(12):CD011535. doi: 10.1002/14651858.CD011535.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2020 Jan 9;1:CD011535. doi: 10.1002/14651858.CD011535.pub3. PMID: 29271481 Free PMC article. Updated.
-
Systematic review and economic analysis of the comparative effectiveness of different inhaled corticosteroids and their usage with long-acting beta2 agonists for the treatment of chronic asthma in adults and children aged 12 years and over.Health Technol Assess. 2008 May;12(19):iii-iv, 1-360. doi: 10.3310/hta12190. Health Technol Assess. 2008. PMID: 18485271
-
The educational effects of portfolios on undergraduate student learning: a Best Evidence Medical Education (BEME) systematic review. BEME Guide No. 11.Med Teach. 2009 Apr;31(4):282-98. doi: 10.1080/01421590902889897. Med Teach. 2009. PMID: 19404891
References
-
- Bastiaens I, Beesley C. Economic hardship and welfare policy preferences: What can the COVID-19 pandemic tell us? Polit Stud Rev. (2024) 23:313–32. 10.1177/14789299241252386 - DOI
Publication types
LinkOut - more resources
Full Text Sources

