Giant Cell Myocarditis Presenting With Cardiogenic Shock: Diagnostic and Therapeutic Challenges
- PMID: 40615209
- PMCID: PMC12441243
- DOI: 10.1016/j.jaccas.2025.103859
Giant Cell Myocarditis Presenting With Cardiogenic Shock: Diagnostic and Therapeutic Challenges
Abstract
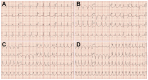
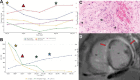
Giant cell myocarditis (GCM) is a rare but often fatal inflammatory cardiomyopathy characterized by aggressive myocardial inflammation and necrosis. Prompt recognition and immunosuppressive therapy are critical for improving outcomes. A 48-year-old woman with no prior cardiac history presented with dyspnea, orthopnea, and hypotension. Electrocardiography showed wide complex tachycardia with retrograde V-to-A conduction. Laboratory findings revealed rising high-sensitivity troponin, hepatic injury, and leukocytosis. Echocardiography showed biventricular failure, and cardiac magnetic resonance imaging showed myocardial edema and subepicardial enhancement. Endomyocardial biopsy confirmed GCM. Immunosuppressive therapy with corticosteroids, tacrolimus, and mycophenolate mofetil led to clinical improvement, avoiding transplantation. GCM remains a diagnostic and therapeutic challenge due to its rapid progression and arrhythmic burden. This case highlights the importance of early biopsy, tailored immunosuppression, and vigilant monitoring in managing fulminant myocarditis.
Keywords: endomyocardial biopsy; giant cell myocarditis; immunosuppression.
Copyright © 2025 The Authors. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Funding Support and Author Disclosures The authors have reported that they have no relationships relevant to the contents of this paper to disclose.
Figures

References
-
- Caforio A.L.P., Pankuweit S., Arbustini E., et al. Current state of knowledge on aetiology, diagnosis, management, and therapy of myocarditis: a position statement of the European Society of Cardiology Working Group on Myocardial and Pericardial Diseases. Eur Heart J. 2013;34(33):2636–2648. doi: 10.1093/eurheartj/eht210. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

