Budesonide-Formoterol Metered-Dose Inhaler vs Fluticasone-Salmeterol Dry-Powder Inhaler
- PMID: 40622686
- PMCID: PMC12235531
- DOI: 10.1001/jamainternmed.2025.2299
Budesonide-Formoterol Metered-Dose Inhaler vs Fluticasone-Salmeterol Dry-Powder Inhaler
Abstract
Importance: Transitioning from metered-dose inhalers to propellant-free dry-powder inhalers could reduce health care-related greenhouse gas emissions, but the clinical difference in outcomes that may be associated with this switch is uncertain.
Objective: To evaluate the clinical difference in outcomes associated with a July 2021 Veterans Health Administration (VHA) formulary change that replaced budesonide-formoterol metered-dose inhaler with fluticasone-salmeterol dry-powder inhaler for the treatment of chronic obstructive pulmonary disease and asthma.
Design, setting, and participants: This within-person, self-controlled case series (SCCS) and matched observational cohort study (cohort study) used data from the US Veterans Affairs health care system from January 2018 through December 2022. Veterans who were prescribed a combination inhaler before and after the formulary change were included in both the SCCS and cohort study. Data were analyzed between April 19, 2024, and April 4, 2025.
Exposures: Treatment with budesonide-formoterol metered-dose inhaler vs fluticasone-salmeterol dry-powder inhaler.
Main outcomes and measures: Rescue medication use (albuterol and prednisone fills), emergency department visits, and hospitalizations (all-cause, respiratory-related, and pneumonia-specific) were assessed.
Results: Following the VHA formulary change, 260 268 patients switched from budesonide-formoterol metered-dose therapy to fluticasone-salmeterol dry-powder therapy. In the SCCS (median [IQR] age, 71 [62-75] years; 91% male), among patients who switched inhalers and experienced the adverse outcomes of interest, treatment with fluticasone-salmeterol dry-powder inhaler therapy was associated with a 10% decrease in albuterol fills (incidence rate ratio [IRR], 0.90 [95% CI, 0.90-0.91]), a 2% increase in prednisone fills (IRR, 1.02 [95% CI, 1.01-1.03]), a 5% increase in all-cause emergency department visits (IRR, 1.05 [95% CI, 1.04-1.06]), an 8% increase in all-cause hospitalizations (IRR, 1.08 [95% CI, 1.06-1.09]), a 10% increase in respiratory-related hospitalizations (IRR, 1.10 [95% CI, 1.07-1.14]), and a 24% increase in pneumonia-specific hospitalizations (IRR, 1.24 [95% CI, 1.17-1.31]). In the cohort study of 258 557 patients (mean [SD] age, 68.9 [11.3] years; 94% male), those who switched to a fluticasone-salmeterol dry-powder inhaler had no difference in mortality (1.89% vs 1.90%; adjusted absolute difference, -0.01 percentage points [95% CI, -0.12 to 0.10 percentage points]) but had increases in all-cause hospitalizations (16.14% vs 15.64%; adjusted absolute difference, 0.49 percentage points [95% CI, 0.21-0.78 percentage points]), respiratory-related hospitalizations (3.15% vs 2.74%; adjusted absolute difference, 0.41 percentage points [95% CI, 0.27-0.55 percentage points]), and pneumonia-related hospitalizations (1.15% vs 1.03%; adjusted absolute difference, 0.12 percentage points [95% CI, 0.04-0.21 percentage points]) at 180 days after the switch compared with matched patients who did not switch.
Conclusions and relevance: The study found that the VHA formulary transition from budesonide-formoterol metered-dose inhaler to fluticasone-salmeterol dry-powder inhaler was associated with increased health care utilization, suggesting potential harm and the need to reevaluate this policy change.
Conflict of interest statement
Figures

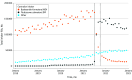

References
-
- Delivering a ‘net zero’ National Health Service. NHS England. Accessed November 5, 2024. https://www.england.nhs.uk/greenernhs/publication/delivering-a-net-zero-...
-
- Gupta S, Couillard S, Digby G, et al. Canadian Thoracic Society position statement on climate change and choice of inhalers for patients with respiratory disease. Can J Respir Crit Care Sleep Med. 2023;7(5):232-239. doi: 10.1080/24745332.2023.2254283 - DOI
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

