Comparison of different tracheal intubation methods for unstable upper cervical spine injuries in a human cadaver model
- PMID: 40624230
- PMCID: PMC12234655
- DOI: 10.1038/s41598-025-09724-2
Comparison of different tracheal intubation methods for unstable upper cervical spine injuries in a human cadaver model
Abstract
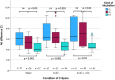
In severe trauma, it is estimated that approximately 2% of patients will sustain a spinal cord injury. The optimal method for advanced airway management that will minimize any associated cervical spine movement remains a topic of debate. Therefore, the aim of this study is to compare the effects of different tracheal intubation techniques in unstable injuries of the cervical spine. Tracheal intubation using conventional laryngoscopy (CL), video laryngoscopy (VL) or flexible bronchoscopic intubation (FO) was performed in six fresh human cadavers. Compression of the dural sac as well as angulation, distraction and intubation time were assessed by myelography in the presence of isolated atlanto-occipital dislocation (AOD) and of combined atlanto-occipital dislocation with atlanto-axial instability (AAI). In case of an isolated AOD, FO intubation resulted in significantly less compression of the dural sac at both levels compared to CL (- 0.46 mm vs. - 1.31 mm; p < 0.001, r = .66) for C0/C1 and (- 0.09 mm vs. - 0.19 mm; p = < 0.05, r = .36) for C1/C2 and VL (- 0.46 mm vs. - 0.64 mm; p = < 0.05, r = .42 for C0/C1 and (- 0.09 mm vs. - 0.22 mm; p = < 0.01, r = .52) for C1/C2. Atlanto-axial Angulation in simultaneous AOD and AAI, the differences between CL and VL were significantly in favor of VL (4.1° vs. 3.2°; p = < 0.05, r = .39), and using FO resulted in less angulation than CL (2.5° vs. 4.1°; p = < 0.001, r = .60) and VL (2.5° vs. 3.2°; p = < 0.05). FO required longer in the case of combined AOD and AAI (FO 16.6 s vs. CL 9.8 s; p = < 0.001, r = .56), (FO 16.6 s vs. VL 9.7 s; p = < 0.001, r = .56). The study demonstrated that tracheal intubation using VL caused significant less compression of the dural sac than the CL. FO showed the lowest compression at all measuring points, but took almost twice as long. For elective or stable patients, where time to airway management is not a relevant factor, FO appears to be the safest method. However, FO is not available everywhere, and in urgent emergency situations, the longer duration may not be acceptable. In such cases, video laryngoscopy can represent a compromise between duration and patient safety, and most physicians have more clinical experience with VL than with FO.
Keywords: Cervical spine; Direct laryngoscopy; Flexible bronchoscopic intubation; Tracheal intubation; Video laryngoscopy.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Competing interests: The authors declare no competing interests. Ethical approval and consent to participate: The protocol for this study was approved and had provided permission by the ethics committee of the Rhineland-Palatinate Medical Association (Registration No. 837.156.16) and registered in the German Clinical Trials Register (DRKS00010499). The body donors have given their written informed consent to medical and scientific use in accordance with the regulations of the state of Baden-Wuerttemberg.
Figures





Similar articles
-
[Conventional intubation and laryngeal tube in cervical spine instability : Changes in the width of the dural sac in unfixed human body donors].Anaesthesist. 2019 Aug;68(8):509-515. doi: 10.1007/s00101-019-0625-8. Epub 2019 Jul 23. Anaesthesist. 2019. PMID: 31338524 German.
-
Avoidance versus use of neuromuscular blocking agents for improving conditions during tracheal intubation or direct laryngoscopy in adults and adolescents.Cochrane Database Syst Rev. 2017 May 17;5(5):CD009237. doi: 10.1002/14651858.CD009237.pub2. Cochrane Database Syst Rev. 2017. PMID: 28513831 Free PMC article.
-
Videolaryngoscopy versus direct laryngoscopy for adult patients requiring tracheal intubation.Cochrane Database Syst Rev. 2016 Nov 15;11(11):CD011136. doi: 10.1002/14651858.CD011136.pub2. Cochrane Database Syst Rev. 2016. Update in: Cochrane Database Syst Rev. 2022 Apr 4;4:CD011136. doi: 10.1002/14651858.CD011136.pub3. PMID: 27844477 Free PMC article. Updated.
-
Videolaryngoscopy versus direct laryngoscopy for adults undergoing tracheal intubation.Cochrane Database Syst Rev. 2022 Apr 4;4(4):CD011136. doi: 10.1002/14651858.CD011136.pub3. Cochrane Database Syst Rev. 2022. PMID: 35373840 Free PMC article.
-
Success of airway management in out-of-hospital cardiac arrest using different devices - a prospective, single-center, observational study comparing professions.Scand J Trauma Resusc Emerg Med. 2025 Jun 23;33(1):109. doi: 10.1186/s13049-025-01422-2. Scand J Trauma Resusc Emerg Med. 2025. PMID: 40551144 Free PMC article.
References
-
- Kumar, R. et al. Traumatic spinal injury: Global epidemiology and worldwide volume. World Neurosurg.113, e345–e363 (2018). - PubMed
-
- Bohlman, H. H. Acute fractures and dislocations of the cervical spine. An analysis of three hundred hospitalized patients and review of the literature. J. Bone Jt. Surg. Am.61(8), 1119–1142 (1979). - PubMed
-
- Stephan, K. et al. Spinal cord injury–incidence, prognosis, and outcome: An analysis of the TraumaRegister DGU. Spine J.15(9), 1994–2001 (2015). - PubMed
-
- Ross, S. E., O’Malley, K. F., DeLong, W. G., Born, C. T. & Schwab, C. W. Clinical predictors of unstable cervical spinal injury in multiply injured patients. Injury23(5), 317–319 (1992). - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

