Parsimonious Subphenotyping Algorithms Perform Differently in Patients With Sepsis and Hematologic Malignancy
- PMID: 40637495
- PMCID: PMC12323692
- DOI: 10.1097/CCM.0000000000006774
Parsimonious Subphenotyping Algorithms Perform Differently in Patients With Sepsis and Hematologic Malignancy
Abstract
Objectives: Latent class assignment-derived subphenotyping algorithms may identify treatment-responsive subgroups of critically ill patients with sepsis and acute respiratory distress syndrome. It is unclear if these algorithms are generalizable to patients with comorbid malignancy, a state which may perturb influential inflammatory biomarkers. This study aimed to test whether malignancy or neutropenia modified the effect of subphenotype assignment by two algorithms as applied to a prospective cohort enriched for ICU patients with active malignancy.
Design: Prospective cohort study at a single U.S. quaternary referral center.
Setting/patients: ICU patients older than 18 admitted to an ICU with a primary admission indication of sepsis.
Interventions: None.
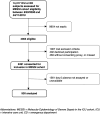
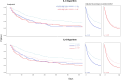
Measurements and main results: We applied two published subphenotyping algorithms utilizing either interleukin (IL)-6 or IL-8 (in addition to soluble tumor necrosis factor receptor 1 and bicarbonate) to our cohort of 930 patients with sepsis, 396 (42%) of whom had active malignancy. A greater proportion of hematologic malignancy patients were assigned the "hyperinflammatory" subphenotype by the IL-8-utilizing algorithm than the IL-6 algorithm (58% vs. 32%). Patients with leukemia and neutropenia were overrepresented among those classified as hyperinflammatory by IL-8 algorithm. We constructed Cox proportional hazards models to assess for interaction between the presence of solid malignancy, hematologic malignancy, and severe neutropenia and the subphenotype/mortality association. Hematologic malignancy uniquely appeared to attenuate the associated mortality of the IL-6-assigned hyperinflammatory subphenotype (interaction; p = 0.037), but not the IL-8-assigned hyperinflammatory subphenotype (interaction; p = 0.260), which retained an independent association with mortality in hematologic malignancy subjects (hazard ratio, 1.50; 95% CI, 1.08-2.07; p = 0.014).
Conclusions: As subphenotyping algorithms are being tested as point-of-care prognostic tools, it is important to understand their generalizability to patients with comorbid malignancy, which constitute an increasing proportion of ICU patients. The differential behavior of these algorithms in patients with hematologic malignancy suggests a need for independent derivation and validation in this specific population.
Keywords: critical illness subphenotyping; hematologic malignancy; oncologic intensive care unit; sepsis.
Copyright © 2025 The Author(s). Published by Wolters Kluwer Health, Inc. on behalf of the Society of Critical Care Medicine and Wolters Kluwer Health, Inc.
Conflict of interest statement
Drs. Ronner, Miano, Dasgupta, West, Jones, Reilly, and Meyer received support for article research from the National Institutes of Health (NIH). Dr. Ronner reports stock ownership in Verona Pharma. Dr. Giannini reports medical advising for TellHealth. Dr. Reilly’s and Meyer’s institutions received funding from the NIH. Dr. Meyer’s institution received funding from the National Heart, Lung, and Blood Institute and Quantum Leap Healthcare Collaborative; she received funding from Endpoint Health, Novartis, and AstraZeneca. The remaining authors have disclosed that they do not have any potential conflicts of interest.
Figures
References
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

