Associations between maternal visceral fat in mid-pregnancy and subsequent gestational diabetes mellitus in a Chinese population: a cohort study
- PMID: 40640737
- PMCID: PMC12243135
- DOI: 10.1186/s12884-025-07873-w
Associations between maternal visceral fat in mid-pregnancy and subsequent gestational diabetes mellitus in a Chinese population: a cohort study
Abstract
Background: Maternal obesity is an established risk factor for gestational diabetes mellitus (GDM). This study aimed to investigate the association between ultrasound-measured visceral adipose tissue and GDM risk in lean Chinese pregnant women.
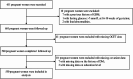
Methods: A prospective cohort study of pregnant women aged 18-45 years with a singleton pregnancy was conducted in Shenzhen Nanshan Maternity and Child Healthcare Hospital, China, between May 2022 and October 2022. Ultrasound measurements of abdominal subcutaneous (SAT) and visceral adipose tissue (VAT) depth were performed at 21-23 weeks' gestation. GDM diagnosis was performed using 75 g oral glucose tolerance test (OGTT) at 24-28 weeks' gestation. After adjustment for maternal age, parity, family history of diabetes, educational level, and pre-pregnancy body mass index (BMI), log-binomial model was used to analyze the associations of ultrasound measurements of VAT and SAT with GDM. A receiver-operating characteristic (ROC) curve analysis was conducted to assess the predictive value of VAT and SAT for new-onset GDM.
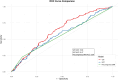
Results: Among 550 women included, 141 subjects (25.6%) developed GDM. The mean maternal age (32.9 ± 4.8 vs. 30.7 ± 4.2 year, P < 0.001) and the mean pre-pregnancy BMI (22.05 ± 2.95 vs. 20.76 ± 2.46 kg/m2, P < 0.001) were significantly higher in women who developed GDM than those who did not. Ultrasound measurements of VAT depth, but not SAT depth, were significantly associated with increased risk for GDM, impaired fasting glucose (IFG) and impaired glucose tolerance (IGT) after adjustment for potential confounders. Compared with the bottom tertile, the risk ratio (RR) and 95% confidence interval (95% CI) in the highest tertile of ultrasound measurements of VAT depth for GDM, IFG and IGT were 2.04 (1.24-3.37), 10.86 (1.37-85.80) and 2.03 (1.22-3.39), respectively. The receiver-operating characteristic (ROC) curve analysis for diagnosis of GDM showed a higher area under the curve (AUC) for VAT than SAT or pre-pregnancy BMI. In stratified analysis, the association of VAT depth with fasting glucose was more profound in women with normal weight before pregnancy than those with overweight or obesity (P - interaction = 0.009).
Conclusions: Ultrasound-measured abdominal VAT during mid-pregnancy is a potential clinical tool for improving sensitivity of early risk stratification for GDM in non-obese pregnant women.
Keywords: Chinese pregnant women; Gestational diabetes; Maternal visceral obesity; Ultrasound.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: The study protocol was reviewed and approved by the Research Ethics Board of Shenzhen Nanshan Maternity and Child Healthcare Hospital (Study code: NSFYEC-KY-2021012, Date of Approval 16 March 2021) and all participants provided written informed consent. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures


Similar articles
-
Different strategies for diagnosing gestational diabetes to improve maternal and infant health.Cochrane Database Syst Rev. 2017 Aug 23;8(8):CD007122. doi: 10.1002/14651858.CD007122.pub4. Cochrane Database Syst Rev. 2017. PMID: 28832911 Free PMC article.
-
Metformin for women who are overweight or obese during pregnancy for improving maternal and infant outcomes.Cochrane Database Syst Rev. 2018 Jul 24;7(7):CD010564. doi: 10.1002/14651858.CD010564.pub2. Cochrane Database Syst Rev. 2018. PMID: 30039871 Free PMC article.
-
Advanced maternal age, overweight and obese positively correlate to the abnormal plasma glucose among gestational diabetes mellitus women even with physical exercise > 90 min/day: a prospective cohort study in Shanghai.Sci Rep. 2025 Jul 1;15(1):21191. doi: 10.1038/s41598-025-09097-6. Sci Rep. 2025. PMID: 40594962 Free PMC article.
-
Prevalence and Risk Factors of Preeclampsia in Pregnant Women With Gestational Diabetes Mellitus.Br J Hosp Med (Lond). 2025 Jun 25;86(6):1-13. doi: 10.12968/hmed.2024.0990. Epub 2025 Jun 20. Br J Hosp Med (Lond). 2025. PMID: 40554442
-
Different intensities of glycaemic control for women with gestational diabetes mellitus.Cochrane Database Syst Rev. 2023 Oct 10;10(10):CD011624. doi: 10.1002/14651858.CD011624.pub3. Cochrane Database Syst Rev. 2023. PMID: 37815094 Free PMC article.
References
-
- Wang H, Li N, Chivese T, et al. IDF diabetes atlas: estimation of global and regional gestational diabetes mellitus prevalence for 2021 by international association of diabetes in pregnancy study group’s criteria. Diabetes Res Clin Pract. 2022;183. 10.1016/j.diabres.2021.109050. published Online First: 20211206. - PubMed
-
- Sweeting A, Hannah W, Backman H, et al. Epidemiology and management of gestational diabetes. Lancet. 2024;404(10448):175–92. 10.1016/s0140-6736(24)00825-0. published Online First: 20240620. - PubMed
MeSH terms
Supplementary concepts
Grants and funding
- JCYJ20210324140808022/Shenzhen Science and Technology Program
- JCYJ20210324140808022/Shenzhen Science and Technology Program
- JCYJ20210324140808022/Shenzhen Science and Technology Program
- JCYJ20210324140808022/Shenzhen Science and Technology Program
- JCYJ20210324140808022/Shenzhen Science and Technology Program
- JCYJ20210324140808022/Shenzhen Science and Technology Program
- No.202408/Sanming Project of Medicine in Shenzhen Nanshan
- No.202408/Sanming Project of Medicine in Shenzhen Nanshan
- No.202408/Sanming Project of Medicine in Shenzhen Nanshan
- No.202408/Sanming Project of Medicine in Shenzhen Nanshan
- No.202408/Sanming Project of Medicine in Shenzhen Nanshan
- No.202408/Sanming Project of Medicine in Shenzhen Nanshan
LinkOut - more resources
Full Text Sources
Research Materials

