Malignant Perivascular Epithelioid Cell Tumor (PEComa) of the Uterus: A Rare Type of Mesenchymal Tumors and a Management Challenge
- PMID: 40647483
- PMCID: PMC12249296
- DOI: 10.3390/cancers17132185
Malignant Perivascular Epithelioid Cell Tumor (PEComa) of the Uterus: A Rare Type of Mesenchymal Tumors and a Management Challenge
Abstract
Gynecologic perivascular epithelioid cell tumors (PEComas) are rare mesenchymal neoplasms characterized by the co-expression of melanocytic markers (HMB-45 and Melan-A) and smooth muscle markers (SMA, desmin, and caldesmon). The uterus is the most common organ affected, with approximately 110 cases reported worldwide, while occurrences in the cervix, vagina, ovary, and other gynecologic locations are exceptionally rare. These tumors typically present with nonspecific symptoms such as abnormal uterine bleeding and pelvic pain, often mimicking other uterine neoplasms. Histopathologically, PEComas exhibit epithelioid and spindle cell morphology with variable nuclear atypia, mitotic activity, and characteristic immunohistochemical profiles. Although most PEComas behave benignly, a subset demonstrates malignant potential, associated with larger tumor sizes, an increased mitotic index, necrosis, and vascular invasion; however, standardized diagnostic criteria remain scarce. Molecular alterations frequently involve the mTOR signaling pathway through tuberous sclerosis complex (TSC) 1 and TSC2 gene mutations, offering potential targets for therapy. Surgical resection with clear margins remains the cornerstone of treatment. For advanced or metastatic cases, mTOR inhibitors have shown promising efficacy, whereas the role of radiotherapy remains uncertain. This review aims to synthesize current knowledge regarding the epidemiology, clinical presentation, histologic features, malignant potential, and treatment of uterine PEComas, emphasizing the importance of accurate histopathological classification and molecular profiling to guide individualized therapeutic strategies.
Keywords: PEComa; mTOR; mesenchymal neoplasms; perivascular epithelioid cell neoplasm; tuberous sclerosis complex.
Conflict of interest statement
Ainhoa Madariaga declares to have received honoraria from AbbVie, AZ, Eisai, GSK, MSD, Pharma&, and PharmaMar. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
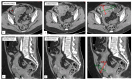
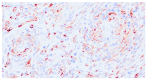
Figures

Similar articles
-
PEComa-its clinical features, histopathology, and current therapy.Jpn J Clin Oncol. 2025 Jul 6;55(7):691-698. doi: 10.1093/jjco/hyaf056. Jpn J Clin Oncol. 2025. PMID: 40336169 Review.
-
PEComa with metastatic pulmonary embolism upon presentation: A case report.Radiol Case Rep. 2025 Jun 24;20(9):4561-4566. doi: 10.1016/j.radcr.2025.06.009. eCollection 2025 Sep. Radiol Case Rep. 2025. PMID: 40641843 Free PMC article.
-
A systematic review: perivascular epithelioid cell tumor of gastrointestinal tract.Medicine (Baltimore). 2016 Jul;95(28):e3890. doi: 10.1097/MD.0000000000003890. Medicine (Baltimore). 2016. PMID: 27428182 Free PMC article.
-
Primary pancreatic perivascular epithelioid cell tumor (PEComa): A surgical enigma. A systematic review of the literature.Pancreatology. 2018 Apr;18(3):238-245. doi: 10.1016/j.pan.2018.02.007. Epub 2018 Feb 19. Pancreatology. 2018. PMID: 29478828
-
Gynecologic perivascular epithelioid cell tumors (PEComas): a review of recent evidence.Arch Gynecol Obstet. 2024 Jun;309(6):2381-2386. doi: 10.1007/s00404-024-07510-5. Epub 2024 Apr 25. Arch Gynecol Obstet. 2024. PMID: 38664269 Free PMC article.
References
-
- Schoolmeester J.K., Howitt B.E., Hirsch M.S., Dal Cin P., Quade B.J., Nucci M.R. Perivascular epithelioid cell neoplasm [PEComa] of the gynecologic tract: Clinicopathologic and immunohistochemical characterization of 16 cases. Am. J. Surg. Pathol. 2014;38:176–188. doi: 10.1097/PAS.0000000000000133. - DOI - PubMed
-
- Musella A., De Felice F., Kyriacou A.K., Barletta F., Di Matteo F.M., Marchetti C., Izzo L., Monti M., Benedetti Panici P., Redler A., et al. Perivascular epithelioid cell neoplasm [PEComa] of the uterus: A systematic review. Int. J. Surg. 2015;19:1–5. doi: 10.1016/j.ijsu.2015.05.002. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

