Systemic Inflammation and Metabolic Changes After Cardiac Surgery and Postoperative Delirium Risk
- PMID: 40648974
- PMCID: PMC12251062
- DOI: 10.3390/jcm14134600
Systemic Inflammation and Metabolic Changes After Cardiac Surgery and Postoperative Delirium Risk
Abstract
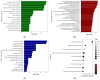
Introduction: Postoperative delirium (POD) remains a major complication in geriatric surgical care, with poorly understood molecular mechanisms. Emerging evidence links cardiac surgery to elevated markers of neurologic injury, even in cognitively intact individuals. While neuroinflammation is the prevailing model, a more detailed characterization of the systemic inflammatory and metabolic response to surgery may offer deeper insights into POD pathogenesis. Methods: We used the 7K SomaLogic proteomic platform to analyze preoperative and postoperative day-one serum samples from 78 patients undergoing cardiac surgery with cardiopulmonary bypass. We compared proteomic profiles within individuals (pre- vs. post-surgery) and between those who developed POD and those who did not. Functional analyses were performed to identify relevant biological pathways. A composite metabo-inflammatory score (MIF) was derived to quantify systemic derangement. We modeled the association between POD and age, sex, baseline cognition, and MIF score. Results: Cardiac surgery with CPB was associated with marked inflammatory responses across all subjects, including increased IL-6, CRP, and serum amyloid A. Compared to controls, POD cases showed greater metabo-inflammatory shifts from baseline (average logFC = 2.56, p < 0.001). Lower baseline cognitive scores (OR = 0.74, p = 0.019) and higher MIF scores (OR = 1.03, p = 0.013) were independently associated with increased POD risk. Conclusions: Cardiac surgery with CPB elicits a significant metabo-inflammatory response in all patients. However, those who develop POD exhibit disproportionately greater dysregulation.
Keywords: cardiac surgery; inflammation; metabolism; postoperative delirium; proteomics.
Conflict of interest statement
O.A. holds patents on anesthetic state monitoring and is a scientific consultant with equity in Reversal Therapeutics. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
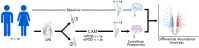

Similar articles
-
Intravenous versus inhalational maintenance of anaesthesia for postoperative cognitive outcomes in elderly people undergoing non-cardiac surgery.Cochrane Database Syst Rev. 2018 Aug 21;8(8):CD012317. doi: 10.1002/14651858.CD012317.pub2. Cochrane Database Syst Rev. 2018. PMID: 30129968 Free PMC article.
-
Remimazolam-Based Anesthesia and Systemic Inflammatory Biomarkers in Relation to Postoperative Delirium in Elderly Patients: A Retrospective Cohort Study.Medicina (Kaunas). 2025 May 30;61(6):1023. doi: 10.3390/medicina61061023. Medicina (Kaunas). 2025. PMID: 40572710 Free PMC article.
-
Intra- and early postoperative predictors of delirium risk in cardiac surgery: results from the prospective observational FINDERI study.Int J Surg. 2025 Apr 1;111(4):2872-2885. doi: 10.1097/JS9.0000000000002265. Int J Surg. 2025. PMID: 39903520 Free PMC article.
-
HMG CoA reductase inhibitors (statins) for preventing acute kidney injury after surgical procedures requiring cardiac bypass.Cochrane Database Syst Rev. 2015 Mar 11;2015(3):CD010480. doi: 10.1002/14651858.CD010480.pub2. Cochrane Database Syst Rev. 2015. PMID: 25758322 Free PMC article.
-
Red cell transfusion management for patients undergoing cardiac surgery for congenital heart disease.Cochrane Database Syst Rev. 2014 Feb 7;2014(2):CD009752. doi: 10.1002/14651858.CD009752.pub2. Cochrane Database Syst Rev. 2014. Update in: Cochrane Database Syst Rev. 2025 Mar 19;3:CD009752. doi: 10.1002/14651858.CD009752.pub3. PMID: 24510598 Free PMC article. Updated.
References
-
- Schubert M., Schürch R., Boettger S., Garcia Nuñez D., Schwarz U., Bettex D., Jenewein J., Bogdanovic J., Staehli M.L., Spirig R. A hospital-wide evaluation of delirium prevalence and outcomes in acute care patients-a cohort study. BMC Health Serv. Res. 2018;18:550. doi: 10.1186/s12913-018-3345-x. - DOI - PMC - PubMed
-
- Li H.-C., Yeh T.Y.-C., Wei Y.-C., Ku S.-C., Xu Y.-J., Chen C.C.-H., Inouye S., Boehm L.M. Association of Incident Delirium With Short-term Mortality in Adults With Critical Illness Receiving Mechanical Ventilation. JAMA Netw. Open. 2022;5:e2235339. doi: 10.1001/jamanetworkopen.2022.35339. - DOI - PMC - PubMed
-
- Wildes T.S., Mickle A.M., Abdallah A.B., Maybrier H.R., Oberhaus J., Budelier T.P., Kronzer A., McKinnon S.L., Park D., Torres B.A. Effect of electroencephalography-guided anesthetic administration on postoperative delirium among older adults undergoing major surgery: The ENGAGES randomized clinical trial. JAMA. 2019;321:473–483. doi: 10.1001/jama.2018.22005. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

