Correlation between fatigue and pulmonary involvement in the post-COVID-19 condition: a cross-sectional study 6-12 months after hospital discharge
- PMID: 40659409
- PMCID: PMC12258267
- DOI: 10.1136/bmjopen-2024-097338
Correlation between fatigue and pulmonary involvement in the post-COVID-19 condition: a cross-sectional study 6-12 months after hospital discharge
Abstract
Introduction: Post-COVID-19 conditions (PCC) may include pulmonary sequelae, fatigue and other symptoms, but its mechanisms are not fully elucidated.
Objective: This study investigated the correlation between fatigue and the presence of pulmonary abnormalities in PCC patients with respiratory involvement 6-12 months after hospitalisation.
Design: Cross-sectional study.
Setting: A tertiary hospital in Brazil.
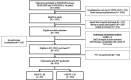
Participants: 315 patients, aged ≥18 years, were considered eligible based on SARS-CoV-2 infection confirmed by reverse transcription-PCR.
Methods: Pulmonary function tests (PFT), cardiopulmonary exercise tests (CPET), chest CT and hand grip were performed. The following scales were applied: Functional Assessment of Chronic Illness Therapy-Fatigue (FACIT-F) scale, Euroqol 5 Dimensions quality of life (EQ-5D) and Hospital Anxiety and Depression Scale (HADS). Participants were divided between the fatigue group (FACIT-F≤30) and the non-fatigue group (FACIT-F>30). For the statistical analysis, the primary outcome was the difference in the diffusing capacity of the lungs for carbon monoxide (DLCO) between groups. Considered secondary outcomes were differences in PFT, CPET, chest CT, hand grip, EQ-5D and HADS.
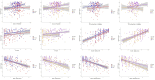
Results: The fatigue group had 81 patients (25.7%) against 234 (74.3%). PFT and CPET showed no significant difference in DLCO and oxygen consumption peak values between groups. The fatigue group had a lower workload (mean 55.3±21.3 watts vs 66.5±23.2 watts, p=0.003), higher breathing reserve (median 41.9% (33.8-52.5) vs 37.7% (28.9-47.1), p=0.028) and lower prevalence of ground glass opacity (60.8% vs 77.7%, p=0.003) and reticulation (36.7% vs 54.9%, p=0.005) in chest CT. The fatigue group had higher anxiety (57% vs 24%, p<0.001), depression (50.6% vs 13.6%, p<0.001), lower health-related quality of life (median 50 (32-63) vs 80 (61.3-88.3), p<0.001) and lower hand grip strength (median 15.8 (6-21) kgf vs 21 (12.1-30) kgf, p<0.001).
Conclusion: Fatigue in patients with PCC 6-12 months after hospitalisation is relatively common and had weak correlation with pulmonary disorders. Our results suggested fatigue could be strongly related with peripheral disorders such as reduced musculoskeletal strength or psychosocial limitations.
Keywords: COVID-19; Fatigue; Medicine; Post-Acute COVID-19 Syndrome.
© Author(s) (or their employer(s)) 2025. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ Group.
Conflict of interest statement
Competing interests: None declared.
Figures
References
-
- World Health Organization COVID-19 weekly epidemiological update. 2024;Available from https://covid19.who.int Available.
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
