High tidal volume mechanical ventilation exacerbates pulmonary injury via upregulation of PAI-1 expression in rats
- PMID: 40660401
- PMCID: PMC12261637
- DOI: 10.1186/s41065-025-00446-z
High tidal volume mechanical ventilation exacerbates pulmonary injury via upregulation of PAI-1 expression in rats
Abstract
Objective: This study aimed to investigate the impact of different mechanical ventilation strategies on pulmonary plasminogen activator inhibitor-1 (PAI-1) expression in a rat model.
Methods: Seventy-two specific pathogen-free (SPF) adult male Sprague-Dawley (SD) rats were randomly assigned to four groups (n = 18): Group C (spontaneous breathing), group S (low tidal volume, VT = 6 mL/kg), group R (regular tidal volume, VT = 10 mL/kg), and group L (high tidal volume, VT = 40 mL/kg). Each group was further divided into three subgroups based on mechanical ventilation duration (2, 4, or 6 h). Following tracheotomy intubation, group C maintained spontaneous breathing, while the other groups underwent mechanical ventilation with a small animal ventilator. Lung wet-to-dry weight ratios, cell apoptosis rate, and lung injury score were recorded. PAI-1 and IL-8 levels were measured in bronchoalveolar lavage fluid (BALF), and PAI-1 mRNA expression in lung tissue was analyzed using real-time polymerase chain reaction (PCR).
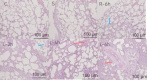
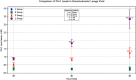
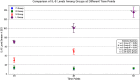
Results: Progressive lung tissue injury was observed in Group L with increasing ventilation durations, accompanied by significant increases in PAI-1, IL-8, and PAI-1 mRNA expression, compared to group C (P < 0.05). No significant differences were identified between Group S and group C, while group R exhibited mild lung injury and minimal increases in PAI-1 expression, observed only after 6 h of ventilation. In group L, PAI-1, IL-8, and PAI-1 mRNA expression increased significantly with extended ventilation durations (P < 0.05).
Conclusion: Mechanical ventilation strategies utilizing high tidal volumes were associated with substantial increases in PAI-1 expression in rat lung tissue and BALF, with these effects exacerbated by prolonged ventilation durations. These findings suggest that high tidal volume ventilation strategies may contribute to pulmonary injury by upregulating PAI-1 expression.
Keywords: Bronchoalveolar lavage fluid; High tidal volume; Mechanical ventilation; PAI-1; Rats.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: All experiments were evaluated and approved by the Ethics Committee of Shanxi Provincial People’s Hospital (2024.863). Principles of Laboratory Animal Care’ (NIH Publication Vol 25, No. 28 revised 1996; http://grants.nih.gov/grants/guide/notice-files/not96-208 . html) were followed, as well as specific national laws (e.g. the current version of the German Law on the Protection of Animals) where applicable. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures
Similar articles
-
Intraoperative use of low volume ventilation to decrease postoperative mortality, mechanical ventilation, lengths of stay and lung injury in adults without acute lung injury.Cochrane Database Syst Rev. 2018 Jul 9;7(7):CD011151. doi: 10.1002/14651858.CD011151.pub3. Cochrane Database Syst Rev. 2018. PMID: 29985541 Free PMC article.
-
Ventilation with lower tidal volumes versus traditional tidal volumes in adults for acute lung injury and acute respiratory distress syndrome.Cochrane Database Syst Rev. 2003;(3):CD003844. doi: 10.1002/14651858.CD003844. Cochrane Database Syst Rev. 2003. Update in: Cochrane Database Syst Rev. 2004;(2):CD003844. doi: 10.1002/14651858.CD003844.pub2. PMID: 12917991 Updated.
-
Hemodynamic Effects of Altering Tidal Volume During Positive Pressure Ventilation in the Fontan Circulation: A Randomized Crossover Trial.Paediatr Anaesth. 2025 Aug;35(8):607-618. doi: 10.1111/pan.15096. Epub 2025 Mar 19. Paediatr Anaesth. 2025. PMID: 40105302 Clinical Trial.
-
Ventilator Management(Archived).2023 Mar 27. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2023 Mar 27. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 28846232 Free Books & Documents.
-
Ventilation with lower tidal volumes versus traditional tidal volumes in adults for acute lung injury and acute respiratory distress syndrome.Cochrane Database Syst Rev. 2004;(2):CD003844. doi: 10.1002/14651858.CD003844.pub2. Cochrane Database Syst Rev. 2004. Update in: Cochrane Database Syst Rev. 2007 Jul 18;(3):CD003844. doi: 10.1002/14651858.CD003844.pub3. PMID: 15106222 Updated.
References
-
- AK AK, Anjum F, Ventilator-Induced Lung Injury (VILI). 2023 Apr 27. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan–. PMID: 33085391. - PubMed
-
- Monjezi M, Jamaati H, Noorbakhsh F. Attenuation of ventilator-induced lung injury through suppressing the pro-inflammatory signaling pathways: A review on preclinical studies. Mol Immunol. 2021;135:127–36. 10.1016/j.molimm.2021.04.007. Epub 2021 Apr 22. PMID: 33895577. - PubMed
-
- Silva PL, Ball L, Rocco PRM, Pelosi P. Physiological and pathophysiological consequences of mechanical ventilation. Semin Respir Crit Care Med. 2022;43(3):321–34. 10.1055/s-0042-1744447. Epub 2022 Apr 19. PMID: 35439832. - PubMed
-
- Kuchnicka K, Maciejewski D. Ventilator-associated lung injury [J]. Anaesthesiol Intensive Ther. 2013;45(3):164–70. - PubMed
-
- Li M, Song J, Tang X, Bi J, Li Y, Chen C, Feng N, Song Y, Wang L. Critical roles of PAI-1 in lipopolysaccharide-induced acute lung injury. Adv Med Sci. 2024;69(1):90–102. Epub 2024 Feb 21. PMID: 38387409. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Miscellaneous

