Concurrent Treatment of Posttraumatic Stress Disorder and Alcohol Use Disorder in Women: A Randomized Clinical Trial
- PMID: 40663349
- PMCID: PMC12371515
- DOI: 10.1001/jamanetworkopen.2025.21087
Concurrent Treatment of Posttraumatic Stress Disorder and Alcohol Use Disorder in Women: A Randomized Clinical Trial
Erratum in
-
Error in the Visual Abstract.JAMA Netw Open. 2025 Aug 1;8(8):e2532737. doi: 10.1001/jamanetworkopen.2025.32737. JAMA Netw Open. 2025. PMID: 40839272 Free PMC article. No abstract available.
Abstract
Importance: Trauma-focused treatments are effective for posttraumatic stress disorder (PTSD) but are rarely offered to patients with comorbid substance use disorder. Research suggests gender-based differences in prevalence and treatment needs for these patients, but treatment trials have mainly included men.
Objective: To evaluate whether integrated trauma-focused psychological treatment (ie, integrated treatment) leads to greater reduction in PTSD symptom severity and weekly alcohol use than usual treatment (ie, relapse prevention) for alcohol use disorder (AUD) in women.
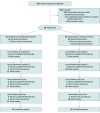
Design, setting, and participants: This randomized clinical trial was conducted at 3 outpatient addiction services in Sweden. Data were collected from 2016 to 2021, and participants were followed up for 9 months after treatment initiation. Data were analyzed from October 2024 to April 2025. Participants were women older than 18 years with current PTSD and moderate-to-severe AUD diagnoses meeting Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) criteria. Participants were randomly assigned to either the integrated treatment or relapse prevention arm. Intention-to-treat analyses were carried out using linear mixed models.
Interventions: Twelve sessions, typically weekly, of integrated treatment (ie, Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure [COPE]) or relapse prevention were delivered by trained and experienced staff (including registered nurses, licensed psychologists, and social workers).
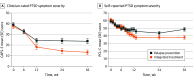
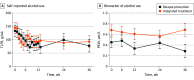
Main outcomes and measures: Prespecified co-primary outcomes were PTSD symptom severity (assessed by blinded raters using Clinician-Administered PTSD Scale for DSM-5 [CAPS-5]) and weekly alcohol use (self-assessed using Timeline Followback) from baseline to the 9-month follow-up. Secondary outcomes included self-reported PTSD symptom severity, clinician-rated PTSD remission, and an objective biomarker of alcohol use (phosphatidylethanol level).
Results: Ninety women (mean [SD] age, 44.7 [12.5] years) were included and randomly assigned to integrated treatment (n = 45) or relapse prevention (n = 45). In both arms, PTSD symptom severity decreased from baseline to 9-month follow-up (mean CAPS-5 score for integrated treatment: 37.40 [95% CI, 33.84-40.96] to 13.18 [95% CI, 8.95-17.41]; relapse prevention: 39.09 [95% CI, 35.53-42.65] to 23.68 [95% CI, 19.47-27.88]), with a significantly greater decrease in the integrated treatment arm than the relapse prevention arm (treatment-by-time interaction: F4,155 = 3.0; P = .02). Self-reported alcohol use decreased significantly over time (F14,581 = 3.0; P < .001) in both arms (integrated treatment: 144.41 [95% CI, 104.66-184.15] g/week to 92.65 [95% CI, 48.81-136.48] g/week; relapse prevention: 133.45 [95% CI, 93.71-173.19] g/week to 77.80 [95% CI, 31.65-123.95] g/week), but there was no detectable difference between treatments.
Conclusions and relevance: In this trial of integrated treatment vs relapse prevention, integrated treatment led to a greater reduction in PTSD symptom severity and no detectable difference in alcohol use decrease compared with relapse prevention. These results support that integrated treatment can safely and effectively treat PTSD in women with AUD and ongoing alcohol use.
Trial registration: ISRCTN.org Identifier: ISRCTN61391164.
Conflict of interest statement
Figures
References
-
- Kessler RC. Posttraumatic stress disorder: the burden to the individual and to society. J Clin Psychiatry. 2000;61(suppl 5):4-12. - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

