Genetically proxied risk and protective factors for pancreatic cancer: a systematic review and meta-analysis of Mendelian randomization studies
- PMID: 40672103
- PMCID: PMC12261061
- DOI: 10.21037/jgo-2025-305
Genetically proxied risk and protective factors for pancreatic cancer: a systematic review and meta-analysis of Mendelian randomization studies
Abstract
Background: Despite extensive observational evidence implicating lifestyle habits, metabolic factors, hormone levels, predisposing genetic conditions, medications, and other exposures, causal inference regarding pancreatic ductal adenocarcinoma (PDAC) risk factors remain contentious due to residual confounding. This Mendelian randomization (MR) meta-analysis was employed to address unresolved etiological controversies and systematically investigate causal relationships between these modifiable factors and clinical outcomes.
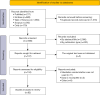
Methods: We conducted a systematic assessment and meta-analysis focusing on studies that employed MR methods to assess the correlation between impact factors and PDAC. We searched five databases, including PubMed, Embase, Web of Science, Scopus, and Ovid, and ultimately included 82 studies, with 292 independent findings. A meta-analysis was performed on 56 of these influencing factors.
Results: Our study found that several factors may be risk factors for PDAC, including body mass index (BMI) [odds ratio (OR): 1.23, 95% confidence interval (CI): 1.10-1.36], gut microbiota (OR: 1.25, 95% CI: 1.05-1.49), diabetes mellitus (OR: 1.07, 95% CI: 1.02-1.13), body size (OR: 1.72, 95% CI: 1.48-2.00), fasting insulin (OR: 2.23, 95% CI: 1.61-3.09), hip circumference (OR: 1.34, 95% CI: 1.11-1.61) and inflammatory bowel disease (IBD) (OR: 1.18, 95% CI: 1.04-1.34). Conversely, potential protective factors against PDAC included lycopene intake (OR: 0.87, 95% CI: 0.77-0.99) and cathepsin E levels (OR: 0.96, 95% CI: 0.94-0.99), and these factors should be further investigated.
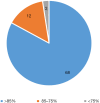
Conclusions: This meta-analysis of MR studies identified several risk and protective factors for pancreatic cancer, with most showing low heterogeneity. However, these findings represent associations, not causality. These findings may inform clinical risk assessment while awaiting further validation. The study highlights the need for continued research focusing on diverse populations, mechanistic studies, longitudinal investigations, and translational work to advance understanding and develop effective strategies for pancreatic cancer prevention and treatment.
Keywords: Mendelian randomization (MR); Pancreatic neoplasms; meta-analysis; risk factors; systematic review.
Copyright © 2025 AME Publishing Company. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jgo.amegroups.com/article/view/10.21037/jgo-2025-305/coif). S.G.K. is the PI of investigator-initiated studies from Mauna Kea Technologies, Paris, France, and TaeWoong Medical, USA, and serves as a consultant for Boston Scientific. The other authors have no conflicts of interest to declare.
Figures


Similar articles
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2017 Dec 22;12(12):CD011535. doi: 10.1002/14651858.CD011535.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2020 Jan 9;1:CD011535. doi: 10.1002/14651858.CD011535.pub3. PMID: 29271481 Free PMC article. Updated.
-
Inflammatory cytokines mediate the gut microbiota-EGPA subtype link: a Mendelian randomization study.Clin Rheumatol. 2025 Jul;44(7):3061-3071. doi: 10.1007/s10067-025-07526-5. Epub 2025 Jun 12. Clin Rheumatol. 2025. PMID: 40500572
-
Regional cerebral blood flow single photon emission computed tomography for detection of Frontotemporal dementia in people with suspected dementia.Cochrane Database Syst Rev. 2015 Jun 23;2015(6):CD010896. doi: 10.1002/14651858.CD010896.pub2. Cochrane Database Syst Rev. 2015. PMID: 26102272 Free PMC article.
-
Selenium for preventing cancer.Cochrane Database Syst Rev. 2018 Jan 29;1(1):CD005195. doi: 10.1002/14651858.CD005195.pub4. Cochrane Database Syst Rev. 2018. PMID: 29376219 Free PMC article.
References
LinkOut - more resources
Full Text Sources
