TyG-BMI as a predictor of ischemic stroke over 10 years in middle-aged and older adults: findings from the China cardiometabolic disease and cancer cohort (4C) study
- PMID: 40672456
- PMCID: PMC12263381
- DOI: 10.3389/fneur.2025.1609853
TyG-BMI as a predictor of ischemic stroke over 10 years in middle-aged and older adults: findings from the China cardiometabolic disease and cancer cohort (4C) study
Abstract
Background: Ischemic stroke (IS) is a leading cause of death and disability, imposing a significant economic burden globally. Research has demonstrated that insulin resistance (IR) plays a key role in the development of atherosclerosis, platelet dysfunction, and a hypercoagulable state, all of which contribute to the pathogenesis and progression of IS. The triglyceride-glucose (TyG) index serves as a practical tool for assessing insulin sensitivity, with previous studies exploring its correlation with IS. However, the relationship between the novel TyG-body mass index (TyG-BMI), which combines TyG with body mass index (BMI) as a measure of general obesity, and IS remains unclear. Therefore, this study employs a prospective design to assess the predictive value of TyG-BMI for the 10-year risk of IS in individuals without intervention.
Methods: The study population was derived from the China Cardiometabolic Disease and Cancer Cohort (4C) Study, predominantly comprising participants from Luzhou City, Sichuan Province, and primarily targeting individuals aged 40 and above. Comprehensive data collection was conducted using both questionnaires and specialized medical equipment, covering physical measurements, blood pressure, and relevant biochemical markers. Participants with a history of stroke were excluded from the study. Based on the initial data, participants were divided into four groups according to the TyG-BMI quartiles. Spearman correlation analysis was used to examine the relationship between TyG-BMI and clinical and laboratory parameters. The Log-rank test was applied to analyze differences in the cumulative incidence of IS among the four groups. The Cox proportional hazards model was used to analyze the relationship between TyG-BMI and the 10-year incidence of new IS. Additionally, the ROC curve was employed to assess the predictive value of TyG-BMI for the 10-year incidence of new IS in the middle-aged and elderly population.
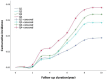
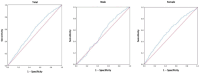
Results: This study included 9,406 participants, consisting of 3,139 males (33.4%) and 6,267 females (66.6%). During the non-interventional follow-up period of 10 years, 483 deaths were recorded, resulting in a mortality rate of 5.1%. In addition, 527 new cases of IS were reported, yielding an incidence rate of 5.6%. The Log-rank test revealed a significant increase in the cumulative incidence of IS across increasing TyG-BMI quartiles (p < 0.01). Furthermore, Cox regression analysis identified a significant correlation between TyG-BMI levels, as a risk factor, and the occurrence of IS. After adjusting for other risk factors, the risk of developing new IS in the Q2 group was 1.449 times that of the Q1 group (p = 0.012), while the risk in the Q3 group was 1.438 times that of the Q1 group (p = 0.014), and the risk in the Q4 group was 1.434 times that of the Q1 group (p = 0.020). ROC curve analysis showed that, in the overall study population, TyG-BMI demonstrated a predictive value for new IS over 10 years (AUC = 0.566, 95% CI = 0.542-0.590, p < 0.001), with a cutoff value of 204.1307, sensitivity of 64.3%, and specificity of 47.8%. In male participants, TyG-BMI showed a predictive value for new IS over 10 years (AUC = 0.537, 95% CI = 0.501-0.574, p = 0.067), with a cutoff value of 195.1996, sensitivity of 73.8%, and specificity of 37.0%. In female participants, TyG-BMI demonstrated a predictive value for new IS over 10 years (AUC = 0.583, 95% CI = 0.551-0.615, p < 0.001), with a cutoff value of 204.295, sensitivity of 65.8%, and specificity of 48.7%.
Conclusion: This study revealed a significant association between TyG-BMI and the 10-year incidence of new-onset IS among middle-aged and elderly individuals, indicating that TyG-BMI may serve as a valuable predictive marker for assessing IS risk in this population.
Keywords: TyG-BMI; body mass index; insulin resistance; ischemic stroke; triglyceride-glucose index.
Copyright © 2025 Miao, Wang, He, Yan and Wan.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Association between insulin resistance indices and outcomes in patients with heart failure with preserved ejection fraction.Cardiovasc Diabetol. 2025 Jan 22;24(1):32. doi: 10.1186/s12933-025-02595-x. Cardiovasc Diabetol. 2025. PMID: 39844150 Free PMC article.
-
[Association between obesity and the risk of microvascular complications in Yinzhou District, Ningbo adults with type 2 diabetes mellitus].Wei Sheng Yan Jiu. 2025 Jul;54(4):608-620. doi: 10.19813/j.cnki.weishengyanjiu.2025.04.012. Wei Sheng Yan Jiu. 2025. PMID: 40695761 Chinese.
-
Associations of the Neutrophil-to-Lymphocyte Ratio(NLR), Triglyceride-Glucose Index (TyG), and TyG-derived indices with vitality decline in older adults in China: a study within the Integrated Care for Older People (ICOPE) framework.Lipids Health Dis. 2025 Jul 30;24(1):256. doi: 10.1186/s12944-025-02671-x. Lipids Health Dis. 2025. PMID: 40739643 Free PMC article.
-
Effects of a gluten-reduced or gluten-free diet for the primary prevention of cardiovascular disease.Cochrane Database Syst Rev. 2022 Feb 24;2(2):CD013556. doi: 10.1002/14651858.CD013556.pub2. Cochrane Database Syst Rev. 2022. PMID: 35199850 Free PMC article.
-
Signs and symptoms to determine if a patient presenting in primary care or hospital outpatient settings has COVID-19.Cochrane Database Syst Rev. 2022 May 20;5(5):CD013665. doi: 10.1002/14651858.CD013665.pub3. Cochrane Database Syst Rev. 2022. PMID: 35593186 Free PMC article.
Cited by
-
The triglyceride-glucose index: updating evidence from clinical settings to molecular mechanisms in ageing-related cerebrovascular diseases.Cardiovasc Diabetol. 2025 Aug 26;24(1):350. doi: 10.1186/s12933-025-02914-2. Cardiovasc Diabetol. 2025. PMID: 40859224 Free PMC article. Review.
References
LinkOut - more resources
Full Text Sources