Development and validation of a histological calculator for anastomotic margins to predict anastomotic failure among rectal cancer patients treated with neoadjuvant chemoradiotherapy
- PMID: 40676556
- PMCID: PMC12273347
- DOI: 10.1186/s12885-025-14522-0
Development and validation of a histological calculator for anastomotic margins to predict anastomotic failure among rectal cancer patients treated with neoadjuvant chemoradiotherapy
Abstract
Purpose: To identify histological features of anastomotic margins and develop a prediction model for anastomotic failure (AF) in rectal cancer (RC) patients with neoadjuvant chemoradiotherapy (nCRT).
Methods: A total of 350 pairs anastomotic "doughnuts" from RC with nCRT were randomly divided into the primary and validation cohorts at a ratio of 7:3. The histological features were identified and constructed using LASSO (Least absolute shrinkage and selection operator) regression to develop the radiation-induced colorectal injury (RCI) score. An AF prediction mode based on the RCI score was built and evaluated using the area under the receiver operating characteristic curve (AUC), decision curve analysis (DCA), and the DeLong test.
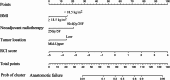
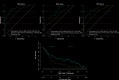
Results: The primary cohort consisted of 245 patients, among whom AF occurred in 26.9% of cases, while the validation cohort comprised 105 patients, with an AF rate of 24.8%. The RCI score of anastomotic margins showed a significant correlation with AF (odds ratio: 2.963; 95% confidence interval [CI]: 2.298-3.822; P < 0.001). Multivariable analysis identified body mass index (BMI) < 18.5, tumor location, long-course radiotherapy, and the RCI score as independent predictors for AF. The nomogram based on the RCI score exhibited good discrimination in both the primary cohort (AUC: 0.886; 95% CI: 0.840-0.931), with a sensitivity of 86.36% (95% CI, 75.7-93.6%) and specificity of 76.54% (95% CI, 69.6-82.5%). Calibration curves revealed satisfactory agreement between the predicted and the observed probabilities.
Conclusions: The comprehensive nomogram incorporating the RCI score could assist physicians in predicting AF and formulating personalized treatment strategies for RC patients with neoadjuvant radiotherapy.
Keywords: Anastomotic failure; Nomogram; Radiation-induced colorectal injury; Radiotherapy; Rectal cancer.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study adhered to the principles of Declaration of Helsinki and received approval from the Institutional Review Board of Fujian Medical University Union Hospital has approved our research procedures (Ethics approval number: 2023KJCX014). Written informed consent was obtained from individual or guardian participants. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures


Similar articles
-
Association of Collagen Changes in Distal Anastomotic Margin and Anastomotic Stenosis after Neoadjuvant Chemoradiotherapy for Rectal Cancer.J Am Coll Surg. 2024 Oct 1;239(4):363-374. doi: 10.1097/XCS.0000000000001116. Epub 2024 Sep 16. J Am Coll Surg. 2024. PMID: 38752618
-
Comparison of Two Modern Survival Prediction Tools, SORG-MLA and METSSS, in Patients With Symptomatic Long-bone Metastases Who Underwent Local Treatment With Surgery Followed by Radiotherapy and With Radiotherapy Alone.Clin Orthop Relat Res. 2024 Dec 1;482(12):2193-2208. doi: 10.1097/CORR.0000000000003185. Epub 2024 Jul 23. Clin Orthop Relat Res. 2024. PMID: 39051924
-
[Development of a nomogram for predicting pathological complete response after neoadjuvant chemoradiotherapy in patients with locally advanced rectal cancer].Zhonghua Wei Chang Wai Ke Za Zhi. 2025 Mar 25;28(3):304-313. doi: 10.3760/cma.j.cn441530-20250106-00012. Zhonghua Wei Chang Wai Ke Za Zhi. 2025. PMID: 40123401 Chinese.
-
Response prediction for neoadjuvant treatment in locally advanced rectal cancer patients-improvement in decision-making: A systematic review.Eur J Surg Oncol. 2025 Jul;51(7):109463. doi: 10.1016/j.ejso.2024.109463. Epub 2024 Nov 15. Eur J Surg Oncol. 2025. PMID: 39562260
-
Does neoadjuvant therapy increase the incidence of anastomotic leakage after anterior resection for mid and low rectal cancer? A systematic review and meta-analysis.Colorectal Dis. 2017 Jan;19(1):16-26. doi: 10.1111/codi.13424. Colorectal Dis. 2017. PMID: 27321374
References
-
- Li J, Hu YT, Liu CC, Wang LH, Ju HX, Huang XF, Chi P, Du JL, Wang JP, Xiao Y, et al. Primary surgery followed by selective chemoradiotherapy versus preoperative chemoradiotherapy followed by surgery for locally advanced rectal cancer: a randomized clinical trial. Int J Radiat Oncol Biol Phys. 2024. 10.1016/j.ijrobp.2023.12.027. - PubMed
-
- Leung E, Gladwish AP, Davidson M, Taggar A, Velker V, Barnes E, Mendez L, Donovan E, Gien LT, Covens A, et al. Quality-of-Life outcomes and toxic effects among patients with cancers of the uterus treated with stereotactic pelvic adjuvant radiation therapy: the SPARTACUS phase 1/2 nonrandomized controlled trial. JAMA Oncol. 2022;8(6):1–9. - PMC - PubMed
-
- Sun W, Dou R, Chen J, Lai S, Zhang C, Ruan L, Kang L, Deng Y, Lan P, Wang L, et al. Impact of long-course neoadjuvant radiation on postoperative low anterior resection syndrome and quality of life in rectal cancer: post hoc analysis of a randomized controlled trial. Ann Surg Oncol. 2019;26(3):746–55. - PubMed
-
- Qiu X, Dong K, Guan J, He J. Hydrogen attenuates radiation-induced intestinal damage by reducing oxidative stress and inflammatory response. Int Immunopharmacol. 2020;84:106517. - PubMed
Publication types
MeSH terms
Grants and funding
- (No: 2017Y9038, 2019Y9101, 2019Y9061, 2020Y9071, 2023Y9167)/the Joint Funds for the Innovation of Science and Technology, Fujian Province
- (No: 2017Y9038, 2019Y9101, 2019Y9061, 2020Y9071, 2023Y9167)/the Joint Funds for the Innovation of Science and Technology, Fujian Province
- (No: 2017Y9038, 2019Y9101, 2019Y9061, 2020Y9071, 2023Y9167)/the Joint Funds for the Innovation of Science and Technology, Fujian Province
- (No: 2017Y9038, 2019Y9101, 2019Y9061, 2020Y9071, 2023Y9167)/the Joint Funds for the Innovation of Science and Technology, Fujian Province
- 2019Y9077, 2023Y9218/the Joint Funds for the Innovation of Science and Technology, Fujian Province,
- 2019Y9077, 2023Y9218/the Joint Funds for the Innovation of Science and Technology, Fujian Province,
- 2019Y9077, 2023Y9218/the Joint Funds for the Innovation of Science and Technology, Fujian Province,
- No: 2020J011030, 2021J01764, 2022J01726, 2022J01753/Natural Science Foundation of Fujian Province
- No: 2020J011030, 2021J01764, 2022J01726, 2022J01753/Natural Science Foundation of Fujian Province
- No: 2020CXA025, 2020GGB022/Fujian Provincial Health Technology Project
- No: 2020CXA025, 2020GGB022/Fujian Provincial Health Technology Project
LinkOut - more resources
Full Text Sources

