The Perinatal Committee report: Review of the progress of obstetric healthcare in Japan
- PMID: 40690975
- PMCID: PMC12279424
- DOI: 10.1111/jog.16354
The Perinatal Committee report: Review of the progress of obstetric healthcare in Japan
Abstract
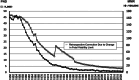
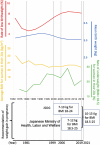
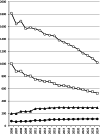
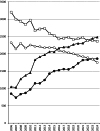
Background: Japan's maternal mortality rate and perinatal mortality rate have shown one of the world's most significant declines, positioning Japan at the global forefront of the lowest levels. The nearly logarithmic annual decline in maternal and perinatal mortality rates suggests that, in addition to advances in medicine and healthcare, various types of care for mothers and newborns have played a crucial role in this achievement.
Method: From the period of World War II to the postwar era, up to around 1980, and then every decade thereafter, the events and movements surrounding perinatal healthcare in each era were examined from the perspectives of epidemiology, medical/healthcare advancements, and institutional/policy trends.
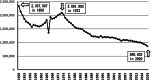
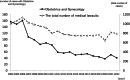
Results: The major events in each era are outlined as follows: Until around 1980: After World War II, in 1948, several laws were enacted to protect mothers and fetuses, including the Maternal and Child Health Handbook, in 1966. The number of births experienced a baby boom for about 10 years following 1945, peaking in 1973. Birthplaces shifted from home deliveries to medical facilities, with doctors becoming the primary birth attendants. Academically, the Japan Association of Obstetricians and Gynecologists (JAOG) for Maternal Protection and the Japan Society of Obstetrics and Gynecology (JSOG) were established in 1949. In the medical field, neonatal intensive care units (NICUs) were introduced and neonatal transport systems became well-established by the 1970s. In 1976, the limit of viability was revised from under 28 weeks of gestation to under 24 weeks. The late 1970s saw the fetal heart rate monitoring, the heartbeat detection using Doppler ultrasound and the ultrasound imaging techniques. 1980s: The perinatal medicine became well established, leading to hold The Japan Society of Perinatal Medicine. For fetal management, the fields of fetal diagnosis and fetal treatment entered their early stages with the widespread use of fetal heart rate monitoring and ultrasound imaging. In neonatal care, neonatal transport systems to NICU facilities were enhanced. A major breakthrough in this field was the discovery and widespread use of pulmonary surfactant. Two key concepts that emerged and advanced during this period were maternal transport systems and the Perinatal Maternal and Child Center initiative. In 1987, cases of hepatitis caused by non-heat-treated coagulation products became a major issue. As a result, informed consent affecting mothers and fetuses became a significant point of discussion. The Obstetrics and Gynecology Specialist system was introduced, along with the regular publication of Training Notes for Obstetricians and Gynecologists and Glossary of Obstetrics and Gynecology Terms. As a result of these efforts, both the perinatal mortality rate and the maternal mortality rate were reduced by approximately half over the course of 10 years. 1990s: In 1991, the limit of viability was revised to 22 weeks of gestation. In terms of maternal care, nutritional management guidelines for general pregnant women were introduced. In fetal medicine, major topics included the administration of steroids to the mother to promote fetal lung maturation, as well as direct fetal treatments such as shunt procedures and needle aspirations. In neonatal care, inhaled nitric oxide therapy and extracorporeal membrane oxygenation treatment became more widely adopted. Following the Great Hanshin-Awaji Earthquake, in 1995, led to the development of the Disaster Medical Assistance Team and the establishment of Perinatal Maternal and Child Medical Center. In 1996, the Maternal Protection Law was enacted, and the Japan Council for Quality Health Care (JCQHC) was founded to standardize medical care. Asia & Oceania Federation of Obstetrics & Gynecology Journal and Journal of Obstetrics and Gynecology Research were launched as English-language academic journals. 2000s: Japan's perinatal mortality rate became the lowest in the world, but the maternal mortality rate was still struggling. Obstetric care changed significantly after an obstetrician was arrested for causing a maternal death during a cesarean section. The JSOG and the JAOG developed practice guidelines describing standard obstetric diagnosis and treatments, and the JCQHC established the Japan Obstetric Compensation System for Cerebral Palsy. In addition, a project to report on maternal deaths by JAOG was also launched, and the combination of these measures led to form a framework of professional autonomy for obstetricians. During this period, brain hypothermic therapy for brain injury was developed. 2010s: The Great East Japan Earthquake in 2011 led to major changes in disaster medical planning. This included the introduction of training programs for disaster medical coordinators and the development of disaster-time pediatric and perinatal liaisons. To enhance medical safety, JAOG launched an incidental case reporting system in 2004. Additionally, in 2010, a maternal mortality reporting system was introduced, followed by the maternal severe complications reporting system in 2021. The Japan Council for Implementation of Maternal Emergency Life-Saving System was established, along with the Japan Association for Labor Analgesia, a collaborative council for academic societies and organizations related to painless delivery. Suicide as a significant cause of maternal death led to the establishment of the "Mother and Child Mental Forum" academic conference, which later evolved into the Mental Health Care for Mother & Child training program. In the field of prenatal testing, non-invasive prenatal testing was introduced as a clinical research initiative. From 2020 onward: The year 2020 began with the global outbreak of COVID-19. Until 2023, numerous issues arose due to repeated pandemics, including delivery methods and locations for COVID-positive pregnant women, standard precautions during labor, mother-infant separation after birth, vaccination, so on. JSOG and JAOG worked together to address these challenges. The most pressing issue in the perinatal field is the declining birth rate. Alongside an aging workforce of physicians and a shortage of successors, the decrease in new obstetric clinic openings has become a major concern. By 2024, the decrease in the number of full-time obstetricians and the overtime work limits in Medical Care Act are making it necessary to reconsider the structure of obstetric medical services. Japan's perinatal care system, which has maintained the highest global standards, now stands at a major crossroads.
Conclusion: Researchers (clinicians), academic societies, and professional organizations, centered on the mother and child, have collaborated with support from the government, making progress and building the current safe pregnancy and childbirth management system. However, significant issues remain that need urgent attention, including regulations on overtime work, securing obstetrician numbers, the rapid decline in childbirth facilities, and the functional collapse of perinatal maternal-child healthcare centers. These are critical challenges that must be addressed promptly.
Keywords: JAOG; JSOG; advance in obstetrical care; maternal mortality; perinatal mortality.
© 2025 The Author(s). Journal of Obstetrics and Gynaecology Research published by John Wiley & Sons Australia, Ltd on behalf of Japan Society of Obstetrics and Gynecology.
Conflict of interest statement
Dr. Kurasawa, Kentaro is an Editorial Board member of JOGR Journal and a co‐author of this article. To minimize bias, they were excluded from all editorial decision‐making related to the acceptance of this article for publication.
Figures







Similar articles
-
Sexual Harassment and Prevention Training.2024 Mar 29. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2024 Mar 29. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 36508513 Free Books & Documents.
-
NIH consensus development conference draft statement on vaginal birth after cesarean: new insights.NIH Consens State Sci Statements. 2010 Mar 10;27(3):1-42. NIH Consens State Sci Statements. 2010. PMID: 20228855
-
The Black Book of Psychotropic Dosing and Monitoring.Psychopharmacol Bull. 2024 Jul 8;54(3):8-59. Psychopharmacol Bull. 2024. PMID: 38993656 Free PMC article. Review.
-
Maternal and neonatal outcomes of elective induction of labor.Evid Rep Technol Assess (Full Rep). 2009 Mar;(176):1-257. Evid Rep Technol Assess (Full Rep). 2009. PMID: 19408970 Free PMC article.
-
Intermittent auscultation (IA) of fetal heart rate in labour for fetal well-being.Cochrane Database Syst Rev. 2017 Feb 13;2(2):CD008680. doi: 10.1002/14651858.CD008680.pub2. Cochrane Database Syst Rev. 2017. PMID: 28191626 Free PMC article.
References
-
- Ministry of Health, Labour and Welfare . Vital statistics (as of June 30, 2025). https://www.mhlw.go.jp/toukei/saikin/hw/jinkou/kakutei23/index.html 2023.
-
- Japan Society of Obstetrics and Gynecology . 50‐Year history of the Japan Society of Obstetrics and Gynecology. Tokyo: Shindan to Chiryo Sha; 1998.
-
- Japan Society of Perinatal and Neonatal Medicine . 50th Anniversary commemorative book of the Japan Society of Perinatal and Neonatal Medicine. Tokyo: Medical View Co., Ltd; 2014.
-
- Kogure K. Historical changes in the treatment of childbirth in the medical insurance system. 5th study group on support measures for pregnant and postpartum women (as of June 30, 2025). https://www.mhlw.go.jp/content/12401000/001330856.pdf 2024.
-
- Japan WHO Association . Maternal and child health handbook (as of June 30, 2025). https://japan-who.or.jp/about-us/maternal-and-child-health-handbook/ 2025.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials

