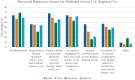
Regional trends in perceptions of American Shoulder and Elbow Surgeons towards barriers to access for patients with Medicaid: limited perioperative service access, low patient engagement, and decreased reimbursement are regionally consistent obstacles
- PMID: 40697303
- PMCID: PMC12277712
- DOI: 10.1016/j.xrrt.2025.03.007
Regional trends in perceptions of American Shoulder and Elbow Surgeons towards barriers to access for patients with Medicaid: limited perioperative service access, low patient engagement, and decreased reimbursement are regionally consistent obstacles
Abstract
Background: Medicaid is a means-tested health insurance program for low-income adults (∼30%), children (∼40%), individuals with disabilities (15%) and some elderly patients that are dual Medicare and Medicaid eligible (15%). It is jointly funded by the federal and state governments but administered by individual states. Allowing states to oversee the administration of Medicaid has led to regional variability in eligibility criteria, types of services covered, and reimbursement. The purpose of this study was to evaluate current perceptions of shoulder and elbow surgeons surrounding practice patterns and barriers to access for patients whose primary insurance type is Medicaid, and to determine if there are notable regional variations in these opinions.
Methods: This was a national, observational study that surveyed the American Shoulder and Elbow Surgeons (ASES) society membership. This 15-question survey assessed surgeon demographics, practice types, reimbursement models, as well as rates and trends of their access to patients with government-assisted insurance. Regional trends in perceived barriers to access for patients with Medicaid were specifically compared in this study.
Results: A total of 257 (18.5% response rate) ASES members completed the survey. The mean year in practice for respondents was 14. The most represented region was the South (35%), followed by the Midwest (24%) and the West (20%) and Northeast (20%). Our results showed that across all regions the top three perceived barriers to access for patients with Medicaid, in varying order, remained consistent - reimbursement, low patient engagement in their care, and the patient's ability to access perioperative services. The most significant regional difference in perceived barriers to Medicaid access was due to implant reimbursement at surgeons' primary surgical facilities. In the South, nearly half (46%) of respondents viewed this as a barrier, whereas only 16% in the Northeast did.
Conclusion: Among members of the ASES, the primary perceived barriers to access for patients with Medicaid remained consistent across geographic region and included reimbursement, low patient engagement in their care, and patient's ability to access perioperative services. The greatest regional disparity in perceived barriers to access for Medicaid was between the South and the Northeast in regard to implant reimbursement at surgeons' primary surgical facility. This was perceived as a barrier to access in 30% more of the Southern respondents compared to respondents from the Northeast. Further investigation into regional differences in Medicaid administration would be valuable to assess how these variances affect patient access to subspecialized shoulder and elbow care.
Keywords: Barriers to care; Insurance; Medicaid; Medical reimbursement; Physician perceptions; Regional medicaid variations.
© 2025 The Author(s).
Figures
References
-
- Alexander D., Schnell M. The impacts of physician payments on patient access, use, and health. Am Econ J Appl Econ. 2024;16:142–147. doi: 10.1257/app.20210227. - DOI
LinkOut - more resources
Full Text Sources