A Premature Infant With Renal Tubular Dysgenesis Who Survived 61 Days With Anuria
- PMID: 40709124
- PMCID: PMC12289354
- DOI: 10.7759/cureus.86687
A Premature Infant With Renal Tubular Dysgenesis Who Survived 61 Days With Anuria
Abstract
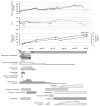
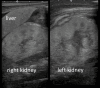
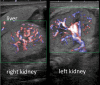
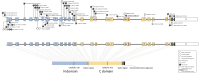
Autosomal recessive renal tubular dysgenesis (AR-RTD) is a rare and typically lethal disorder of the renin-angiotensin system (RAS), caused by mutations in genes such as angiotensinogen (AGT), renin (REN), angiotensin-converting enzyme (ACE), and angiotensin II receptor type 1 (AGTR1). It is characterized by severe hypotension, anuria, and features of Potter sequence, usually resulting in fetal or neonatal death. Although more than 15 surviving cases have been reported, survival has generally been associated with non-truncating mutations. We report the case of a premature male infant born at 34 weeks' gestation with clinical features of AR-RTD and confirmed homozygosity for a novel truncating ACE variant (c.2691delC, p.Phe898SerfsTer14). The pregnancy was complicated by oligohydramnios and fetal growth restriction, and the infant showed no urinary output throughout his life. Despite a poor prognosis, he survived for 61 days with intensive multidisciplinary support but without renal replacement therapy. Initial management included mechanical ventilation, nitric oxide, vasopressin for refractory hypotension, and strict restriction of fluid and electrolyte intake. Lactulose was administered enterally from day 32 of life to mitigate uremic symptoms, potentially aiding in the excretion of nitrogenous waste via the immature intestinal mucosa. The patient ultimately succumbed to renal failure on day 61 of life. Genetic testing confirmed the diagnosis, but parental testing was not performed. A literature review identified 61 genetically confirmed ACE-related AR-RTD cases, with an overall survival rate of 24.6%. Survival was significantly lower among patients with biallelic truncating mutations (8.6%) compared to those with at least one non-truncating allele. While truncating mutations were generally associated with poorer outcomes, exceptions existed, and variant location within the gene did not consistently predict prognosis. Interestingly, more reported mutations clustered on the 3' end, although disease severity tended to be higher with 5' variants. This case is notable as the longest known survival of a patient with confirmed AR-RTD and complete anuria, without renal replacement. The relatively prolonged survival may be attributed to the early initiation of supportive therapy immediately after birth, even before genetic confirmation. Importantly, the time gained allowed for meaningful genetic counseling and family bonding. This report underscores that survival beyond the neonatal period may be possible in AR-RTD cases with truncating ACE variants when early diagnosis and multidisciplinary management are initiated. It highlights the importance of prompt clinical suspicion and supportive care in maximizing life expectancy and enabling family-centered care, even in cases expected to have a dismal prognosis.
Keywords: angiotensin-converting enzyme; anuria; autosomal recessive renal tubular dysgenesis; renal tubular dysgenesis; renin-angiotensin system.
Copyright © 2025, Hayata et al.
Conflict of interest statement
Human subjects: Informed consent for treatment and open access publication was obtained or waived by all participants in this study. Ethics Committee of the Institutional Review Board of Institute of Science Tokyo (Tokyo Medical and Dental University) issued approval G2000-103. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures
Similar articles
-
The Black Book of Psychotropic Dosing and Monitoring.Psychopharmacol Bull. 2024 Jul 8;54(3):8-59. Psychopharmacol Bull. 2024. PMID: 38993656 Free PMC article. Review.
-
Citrullinemia Type I.2004 Jul 7 [updated 2022 Aug 18]. In: Adam MP, Feldman J, Mirzaa GM, Pagon RA, Wallace SE, Amemiya A, editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993–2025. 2004 Jul 7 [updated 2022 Aug 18]. In: Adam MP, Feldman J, Mirzaa GM, Pagon RA, Wallace SE, Amemiya A, editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993–2025. PMID: 20301631 Free Books & Documents. Review.
-
Intravenous magnesium sulphate and sotalol for prevention of atrial fibrillation after coronary artery bypass surgery: a systematic review and economic evaluation.Health Technol Assess. 2008 Jun;12(28):iii-iv, ix-95. doi: 10.3310/hta12280. Health Technol Assess. 2008. PMID: 18547499
-
Maternal and neonatal outcomes of elective induction of labor.Evid Rep Technol Assess (Full Rep). 2009 Mar;(176):1-257. Evid Rep Technol Assess (Full Rep). 2009. PMID: 19408970 Free PMC article.
-
Management of urinary stones by experts in stone disease (ESD 2025).Arch Ital Urol Androl. 2025 Jun 30;97(2):14085. doi: 10.4081/aiua.2025.14085. Epub 2025 Jun 30. Arch Ital Urol Androl. 2025. PMID: 40583613 Review.
References
-
- Spectrum of mutations in the renin-angiotensin system genes in autosomal recessive renal tubular dysgenesis. Gribouval O, Morinière V, Pawtowski A, et al. Hum Mutat. 2012;33:316–326. - PubMed
-
- Renal tubular dysgenesis. Gubler MC. Pediatr Nephrol. 2014;29:51–59. - PubMed
-
- Management of a preterm infant with renal tubular dysgenesis: a case report and review of the literature. Kondoh T, Kawai Y, Matsumoto Y, et al. Tohoku J Exp Med. 2020;252:9–14. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
