Lung Function Changes and Connective Tissue Growth Factor Expression in Idiopathic Pulmonary Fibrosis, Other Progressive Fibrosing Interstitial Lung Diseases, and Post-COVID Fibrosis
- PMID: 40717875
- PMCID: PMC12289458
- DOI: 10.7759/cureus.88645
Lung Function Changes and Connective Tissue Growth Factor Expression in Idiopathic Pulmonary Fibrosis, Other Progressive Fibrosing Interstitial Lung Diseases, and Post-COVID Fibrosis
Abstract
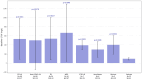
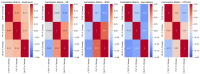
Background The clinical course of patients with idiopathic pulmonary fibrosis (IPF) and other progressive interstitial lung diseases (F-ILDs) varies from mild to severe worsening, which makes the development of new diagnostic and prognostic methods even more urgent. A number of studies have shown that plasma connective tissue growth factor (CTGF) is elevated during IPF, and that the levels of this substance are correlated with the changes in forced vital capacity (FVC). The aim of our study was to investigate CTGF levels in patients with F-ILDs group, including its subgroups IPF and other F-ILDs, as well as post-COVID-19 cases, and to assess their association with lung function changes over a 12-month period. Methods A prospective cohort study was conducted with patients observed over 30 months. The involvement period was 18 months, followed by a 12-month observation period. A total of 86 subjects were enrolled in the study. FVC (measured by spirometry), diffusing lung capacity for carbon monoxide (DLCO), and CTGF levels in blood serum (measured by enzyme-linked immunosorbent assay (ELISA)) were assessed at the beginning and end of the study. Results Regression analysis of the correlations between mean serum CTGF levels, FVC, and DLCO changes in the F-ILDs group demonstrated a significant negative correlation between the changes in mean serum CTGF levels, FVC, and DLCO. Similarly, in the IPF, idiopathic nonspecific interstitial pneumonia (iNSIP) and chronic sarcoidosis (IV stage) subgroups, there was a significant negative correlation between changes in mean serum CTGF levels, FVC, and DLCO. However, in the post-COVID-19 group, regression analysis did not reveal any correlations between changes in mean serum CTGF concentrations, FVC, and DLCO. Conclusion Our data suggest a correlation between decreased pulmonary function and increased CTGF levels in patients with IPF and other PPF conditions. Therefore, CTGF emerges as a potential surrogate marker for fibrosis progression in these patients. In contrast, post-COVID-19 fibrosis appears to be a non-progressive fibrotic disease; however, further monitoring is necessary.
Keywords: connective tissue growth factor (ctgf); diffuse lung capacity for carbon monoxide (dlco); forced vital capacity (fvc); idiopathic pulmonary fibrosis (ipf); interstitial lung diseases (ilds); post-covid-19; progressive fibrosing interstitial lung diseases (f-ilds); progressive pulmonary fibrosis.
Copyright © 2025, Sherozia et al.
Conflict of interest statement
Human subjects: Informed consent for treatment and open access publication was obtained or waived by all participants in this study. The Center for Diabetes, Endocrine and Cardio-Pulmonary Diseases Diacor's independent ethics committee issued approval LEC_INITIAL_APPROVAL_PHDF-21-5568. Animal subjects: All authors have confirmed that this study did not involve animal subjects or tissue. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: This study was funded by the Shota Rustaveli National Science Foundation of Georgia. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures
Similar articles
-
Cyclophosphamide for connective tissue disease-associated interstitial lung disease.Cochrane Database Syst Rev. 2018 Jan 3;1(1):CD010908. doi: 10.1002/14651858.CD010908.pub2. Cochrane Database Syst Rev. 2018. PMID: 29297205 Free PMC article.
-
Jinbei oral liquid for idiopathic pulmonary fibrosis: a randomized placebo-controlled trial.Sci Rep. 2025 Jan 23;15(1):3007. doi: 10.1038/s41598-025-87474-x. Sci Rep. 2025. PMID: 39849152 Free PMC article. Clinical Trial.
-
Lung function trajectories in patients with idiopathic pulmonary fibrosis.Respir Res. 2023 Aug 24;24(1):209. doi: 10.1186/s12931-023-02503-5. Respir Res. 2023. PMID: 37612608 Free PMC article.
-
Exploring the role of serum adiponectin and its holigomerization in fibrotic interstitial lung diseases: results from a cross-sectional study.BMC Pulm Med. 2025 May 26;25(1):263. doi: 10.1186/s12890-025-03706-w. BMC Pulm Med. 2025. PMID: 40420027 Free PMC article.
-
Intravenous antibiotics for pulmonary exacerbations in people with cystic fibrosis.Cochrane Database Syst Rev. 2025 Jan 20;1(1):CD009730. doi: 10.1002/14651858.CD009730.pub3. Cochrane Database Syst Rev. 2025. PMID: 39831540
References
-
- Diagnosis of idiopathic pulmonary fibrosis. An Official ATS/ERS/JRS/ALAT Clinical Practice Guideline. Raghu G, Remy-Jardin M, Myers JL, et al. Am J Respir Crit Care Med. 2018;198:0–68. - PubMed
-
- Progressive fibrosing interstitial lung diseases: current practice in diagnosis and management. Wijsenbeek M, Kreuter M, Olson A, et al. Curr Med Res Opin. 2019;35:2015–2024. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
