Impact of eliciting treatment priorities on analgesic prescribing in older patients with high levels of polypharmacy
- PMID: 40720208
- PMCID: PMC12302712
- DOI: 10.1093/fampra/cmaf056
Impact of eliciting treatment priorities on analgesic prescribing in older patients with high levels of polypharmacy
Abstract
Background: Multimorbidity guidelines recommend tailoring care to patients' priorities. The Supporting Prescribing in Multimorbidity in Primary Care (SPPiRE) trial focused on optimizing medicines use in older adults with significant polypharmacy and tailoring prescribing and deprescribing to individual priorities. This study aimed to compare self-reported and general practitioner (GP)-recorded patient priorities and examine the impact of prioritizing pain on analgesic prescribing.
Methods: This secondary cohort analysis of the SPPIRE trial and process evaluation assessed baseline participant-identified priorities and intervention group GP-recorded priorities during medication reviews with agreement assessed using Cohen's kappa. Analgesic prescribing patterns and daily morphine milligram equivalents changes during the study period were summarized. The impact of pain (self-reported, GP-recorded, and severe or extreme pain on the baseline EQ5D) on opioid intensification was analysed using multi-level models accounting for GP practice clustering and intervention effects.
Results: A total of 403 patients (mean age 76.5 years) were included; 178 (44.2%) reported pain as a priority at baseline. Agreement between self-reported and GP-recorded pain was poor (kappa 0.118, P = 0.05). Most analgesic prescriptions decreased during the study, except for potent opioids, which increased in both trial arms. All three pain variables were associated with increased odds of opioid intensification at follow-up.
Conclusion: In this older population of patients with significant polypharmacy, identifying pain as a priority was associated with an increased likelihood of opioid intensification, despite guidelines advising against their use for chronic pain. This study highlights the challenges faced by GPs treating pain in older adults with multimorbidity.
Plain language summary
Guidelines for managing patients with multiple health conditions recommend focusing on what matters most to patients. The Supporting Prescribing in Multimorbidity in Primary Care (SPPiRE) trial aimed to improve medication use in older adults prescribed ≥ 15 medicines by aligning prescribing decisions with individual patient priorities. This study analysed data from the SPPiRE trial to assess how often patients and general practitioners (GPs) agreed on treatment priorities and how prioritizing pain affected painkiller prescribing. This study included data on 403 older adults (average age 76.5 years), 178 of whom self-reported pain as a priority for treatment when returning postal questionnaires at the start of study. Overall, agreement between patients and GPs on treatment priorities was poor. When assessing changes in painkiller prescribing in all patients (those who had a medication review and those who did not) prescriptions for most painkillers reduced during the study period, but prescriptions for stronger opioids increased. When GPs recorded pain as a treatment priority during the medication review, patients were 2.73 times more likely to have their opioid prescribing intensified compared to patients whose pain was not recorded as a priority in their medication review. This is despite clinical practice guidelines advising not to use opioids to treat chronic pain.
© The Author(s) 2025. Published by Oxford University Press.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures

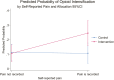
References
-
- Polypharmacy Guidance. SIGN Guidelines. Scottish Intercollegiate Guidelines Network, 2015.
-
- National Guideline Centre (UK). Multimorbidity: assessment, prioritisation and management of care for people with commonly occurring multimorbidity. London: NICE, 2016. - PubMed
-
- Boyd C, Smith CD, Masoudi FA, et al. Decision making for older adults with multiple chronic conditions: executive summary for the American Geriatrics Society guiding principles on the care of older adults with multimorbidity. J Am Geriatr Soc 2019;67:665–73. https://doi.org/ 10.1111/jgs.15809 - DOI - PubMed
-
- McCarthy C, Clyne B, Corrigan D, et al. Supporting prescribing in older people with multimorbidity and significant polypharmacy in primary care (SPPiRE): a cluster randomised controlled trial protocol and pilot. Implementation Sci 2017;12:99. https://doi.org/ 10.1186/s13012-017-0629-1 - DOI - PMC - PubMed
-
- Kyne K, McCarthy C, Kiely B, et al. ; SPPiRE Study team. Study protocol for a process evaluation of a cluster randomised controlled trial to reduce potentially inappropriate prescribing and polypharmacy in patients with multimorbidity in Irish primary care (SPPiRE). HRB Open Res 2019;2:20. https://doi.org/ 10.12688/hrbopenres.12920.2 - DOI - PMC - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

