Clinical, laboratory, radiological features, and outcome of acute fat embolism syndrome in sickle cell disease
- PMID: 40721454
- PMCID: PMC12304287
- DOI: 10.1038/s41598-025-11983-y
Clinical, laboratory, radiological features, and outcome of acute fat embolism syndrome in sickle cell disease
Erratum in
-
Correction: Clinical, laboratory, radiological features, and outcome of acute fat embolism syndrome in sickle cell disease.Sci Rep. 2025 Nov 26;15(1):42104. doi: 10.1038/s41598-025-24320-0. Sci Rep. 2025. PMID: 41298534 Free PMC article. No abstract available.
Abstract
Non-traumatic fat embolism syndrome (FES) affecting brain, lung and hematopoietic system is a rare, but a serious complication of sickle cell disease (SCD), resulting from bone marrow necrosis. SCD-related FES is rare, with the spectrum of clinical, laboratory, radiological manifestations and patient outcome is not fully understood. After medical research & ethics committee approval, retrospectively, SCD-FES patients at our centre, were reviewed between January 2006 to December 2023. 27 patients (17 males, 10 females) with a median age of 24 years and length of hospital stay of 24 (16-38) days were enrolled. They had fever, chest/back pain, cough and crepitation in 100%, 96%, 56% and 100% respectively, with neurological manifestations in 96%. Abnormal chest X-rays and CT scans were observed in 96%, and 100% respectively. Patients had significant anemia, reticulocytopenia, and thrombocytopenia, with raised WBC (p < 0.05). There was a significant rise in LDH, ALP, Ferritin and C-reactive protein levels. All patients received antibiotics, and exchange transfusions, whereas 24%, 76% required non-invasive ventilation (NIV) and mechanical ventilation respectively, with 18.5% mortality. FES is a rapidly progressive respiratory and neurological syndrome, characterized by hypoxia, and cytopenia, with raised inflammatory markers, raised LDH and ALP, with distinctive multiple cerebral microbleeds.
Keywords: Bone marrow necrosis; Exchange transfusion; Fat embolism syndrome; Parvovirus B19; Sickle cell disease.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Competing interests: The authors declare no competing interests.
Figures

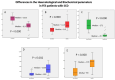
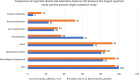
References
-
- Mellor, A. & Soni, N. Fat embolism. Anaesthesia56, 145–154 (2001). - PubMed
-
- Ataga, K. I. & Orringer, E. P. Bone marrow necrosis in sickle cell disease: A description of three cases and a review of the literature. Am. J. Med. Sci.320, 342–347 (2000). - PubMed
-
- Paydas, S. et al. Bone marrow necrosis: Clinicopathologic analysis of 20 cases and review of the literature. Am. J. Hematol.70, 300–305 (2002). - PubMed
-
- Adamski, J. et al. Multiorgan failure and bone marrow necrosis in three adults with sickle cell-β+-thalassemia. Am. J. Hematol.87, 621–624 (2012). - PubMed
-
- Tsitsikas, D. A. et al. Bone marrow necrosis and fat embolism syndrome in sickle cell disease: increased susceptibility of patients with non-SS genotypes and a possible association with human parvovirus B19 infection. Blood Rev.28, 23–30 (2014). - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

