Biomolecular Predictors of Recurrence Patterns and Survival in IDH-Wild-Type Glioblastoma: A Retrospective Analysis of Patients Treated with Radiotherapy and Temozolomide
- PMID: 40722305
- PMCID: PMC12293595
- DOI: 10.3390/brainsci15070713
Biomolecular Predictors of Recurrence Patterns and Survival in IDH-Wild-Type Glioblastoma: A Retrospective Analysis of Patients Treated with Radiotherapy and Temozolomide
Abstract
Background and aim: Glioblastoma (GBM) is the most aggressive primary brain tumor in adults, with poor prognosis despite maximal surgical resection, radiotherapy (RT), and temozolomide (TMZ) per the Stupp protocol. IDH-wild-type GBM, the predominant molecular subtype, frequently harbors EGFR amplification and is resistant to therapy, while MGMT promoter methylation predicts improved TMZ response. This study aimed to assess the prognostic impact of EGFR and MGMT status on survival and recurrence patterns in IDH-wild-type GBM.
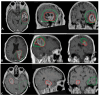
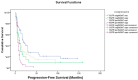
Materials and methods: We retrospectively analyzed 218 patients with IDH-wild-type GBM treated at the Azienda Ospedaliero-Universitaria Senese (2016-2024). All patients underwent maximal safe surgical resection whenever feasible. The cohort includes patients who received gross total resection (GTR), subtotal resection (STR), or biopsy only, depending on tumor location and clinical condition, followed by intensity-modulated RT (59.4-60 Gy) with concurrent and adjuvant TMZ. EGFR amplification was assessed via FISH/NGS and immunohistochemistry; MGMT promoter methylation was determined using methylation-specific PCR. Progression-free survival (PFS), overall survival (OS), and recurrence patterns (in-field, marginal, out-field) were evaluated using Kaplan-Meier, Cox regression, and logistic regression analyses.
Results: Among patients (64.7% male; mean age 61.8), 58.7% had EGFR amplification and 49.1% showed MGMT methylation. Median OS and PFS were 14 and 8 months, respectively. EGFR non-amplified/MGMT methylated tumors had the best outcomes (OS: 22.0 months, PFS: 10.5 months), while EGFR-amplified/MGMT unmethylated tumors fared worst (OS: 10.0 months, PFS: 5.0 months; p < 0.001). MGMT methylation was an independent positive prognostic factor (HR: 0.48, p < 0.001), while EGFR amplification predicted worse survival (HR: 1.57, p = 0.02) and higher marginal recurrence (OR: 2.42, p = 0.01).
Conclusions: EGFR amplification and MGMT methylation significantly influence survival and recurrence dynamics in IDH-wild-type GBM. Incorporating these biomarkers into treatment planning may enable tailored therapeutic strategies, potentially improving outcomes in this challenging disease. Prospective studies are needed to validate biomolecularly guided management approaches.
Keywords: EGFR; MGMT; glioblastoma; pattern of recurrence; radiotherapy.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

References
-
- Ostrom Q.T., Price M., Neff C., Cioffi G., Waite K.A., Kruchko C., Barnholtz-Sloan J.S. CBTRUS Statistical Report: Primary Brain and Other Central Nervous System Tumors Diagnosed in the United States in 2015–2019. Neuro-Oncology. 2022;24((Suppl. 5)):v1–v95. doi: 10.1093/neuonc/noac202. - DOI - PMC - PubMed
-
- Louis D.N., Perry A., Wesseling P., Brat D.J., Cree I.A., Figarella-Branger D., Hawkins C., Ng H.K., Pfister S.M., Reifenberger G., et al. The 2021 WHO Classification of Tumors of the Central Nervous System: A summary. Neuro-Oncology. 2021;23:1231–1251. doi: 10.1093/neuonc/noab106. - DOI - PMC - PubMed
-
- Stupp R., Hegi M.E., Mason W.P., van den Bent M.J., Taphoorn M.J., Janzer R.C., Ludwin S.K., Allgeier A., Fisher B., Belanger K., et al. Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet Oncol. 2009;10:459–466. doi: 10.1016/S1470-2045(09)70025-7. - DOI - PubMed
-
- Hegi M.E., Liu L., Herman J.G., Stupp R., Wick W., Weller M., Mehta M.P., Gilbert M.R. Correlation of O6-methylguanine methyltransferase (MGMT) promoter methylation with clinical outcomes in glioblastoma and clinical strategies to modulate MGMT activity. J. Clin. Oncol. 2008;26:4189–4199. doi: 10.1200/JCO.2007.11.5964. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

