The impact of intermittent fasting on body composition and cardiometabolic outcomes in overweight and obese adults: a systematic review and meta-analysis of randomized controlled trials
- PMID: 40731344
- PMCID: PMC12309044
- DOI: 10.1186/s12937-025-01178-6
The impact of intermittent fasting on body composition and cardiometabolic outcomes in overweight and obese adults: a systematic review and meta-analysis of randomized controlled trials
Abstract
Background: Obesity is a global health crisis, projected to affect over 1.53 billion adults by 2035. Intermittent fasting (IF) has emerged as a potential alternative to continuous energy restriction (CER) for weight management and metabolic improvement. However, previous meta-analyses have reported inconsistent results. These knowledge gaps hinder the clinical translation of IF, and a rigorous synthesis of randomized controlled trials (RCTs) is necessary to clarify their effects on body composition and cardiometabolic health in overweight and obese populations.
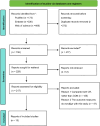
Methods: This PRISMA-guided systematic review and meta-analysis searched PubMed, Embase, and Web of Science up to March 2025. We included 15 randomized controlled trials (n = 758) comparing IF diets with control diets in overweight/obese adults. Primary outcome indicators included total cholesterol (TC), triglycerides (TG), low-density lipoprotein (LDL), high-density lipoprotein (HDL), fasting plasma glucose (FPG), hemoglobin A1C (HbA1c), systolic blood pressure (SBP), diastolic blood pressure (DBP), body weight (BW), body mass index (BMI), waist circumference (WC), and waist-to-hip ratio (WHR). Data were pooled using a random-effects model and analyzed in subgroups by intervention duration and IF form.
Results: IF significantly reduced BW (MD: -3.73 kg, 95% CI: -5.29, -2.17) and BMI (MD: -1.04 kg/m², 95% CI: -1.39, -0.70) in overweight/obese adults, while effectively improving lipid profiles, including TC (MD: -6.31 mg/dl, 95% CI: -12.36, -0.26) and LDL (MD: -5.44 mg/dl, 95% CI: -12.36, -0.26). However, short-term IF (≤ 12 weeks) may have resulted in a temporary elevation of TG (MD: 13.22 mg/dl, 95% CI: 3.39, 23.05), whereas long-term intervention (> 12 weeks) optimized lipid metabolism benefits. In addition, IF significantly reduced DBP (MD: -3.30 mmHg, 95% CI: -5.47, -1.13) but had no significant effect on SBP, FPG and HbA1c. Subgroup analyses showed that alternate day fasting (ADF) was superior to time-restricted eating (TRE) in terms of weight loss and improvement in LDL. The findings suggest that the metabolic effects of IF are time-dependent, and that its clinical use needs to be combined with individualized regimens and long-term adherence strategies. Limitations include the short intervention period (≤ 12 weeks) and high heterogeneity of most studies, and standardized long-term trials are needed to validate the sustained benefits and safety.
Conclusions: As a non-pharmacological intervention, IF demonstrates significant value for weight management and metabolic improvement. Its advantages in adherence and metabolic regulation position it as a promising therapeutic approach. However, its long-term efficacy and safety warrant further validation through additional high-quality clinical studies. Future efforts should focus on developing precise, sustainable, and personalized IF protocols within a personalized medicine framework to achieve comprehensive cardiometabolic health optimization.
Registration: PROSPERO CRD420251036588.
Keywords: Body composition; Intermittent fasting; Lipid profiles; Obesity; Overweight.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Human Ethics and Consent to Participate: Not applicable. Consent for publication: All authors approved the final version of the manuscript, and agreed for all aspects of the work to be published. Competing interests: The authors declare no competing interests. Clinical trial number: Not applicable.
Figures
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous