Wernicke's Encephalopathy Beyond Alcoholism: A Radio-Clinical Case Series From a Tertiary Care Center in South India
- PMID: 40734843
- PMCID: PMC12306145
- DOI: 10.7759/cureus.86954
Wernicke's Encephalopathy Beyond Alcoholism: A Radio-Clinical Case Series From a Tertiary Care Center in South India
Abstract
Introduction Wernicke's encephalopathy (WE) is a serious yet potentially reversible neurological condition resulting from thiamine (vitamin B1) deficiency. Although traditionally linked to chronic alcohol consumption, an increasing number of cases are now being recognized in nonalcoholic individuals, where atypical clinical presentations often lead to diagnostic challenges and delays in treatment. This case series highlights a spectrum of WE cases with varied underlying etiologies, along with their clinical manifestations and characteristic neuroimaging findings. By emphasizing the importance of early recognition and imaging, this study aims to increase clinical awareness and promote timely, appropriate management, thereby reducing morbidity and improving outcomes. Materials and methods This retrospective case series analyzed 14 patients diagnosed with WE between January 2020 and January 2025 at a tertiary care center in South India. The inclusion criteria were clinical suspicion of WE, with supportive MRI findings showing bilateral symmetrical T2/FLAIR hyperintensities in typical regions (thalami, mammillary bodies, and periaqueductal gray). Patients with alternative diagnoses were excluded. Clinical details, comorbidities, etiological factors, imaging findings, treatment response, and outcomes were reviewed. All patients received thiamine therapy. Descriptive statistics were used to summarize the data. Results Among the 14 patients, four were chronic alcoholics, while 10 had nonalcoholic causes such as hyperemesis gravidarum (3), nutritional deficiency (4), parenteral nutrition (2), and CKD on dialysis (1). Most patients presented with altered sensorium and incomplete classical triad symptoms. MRI consistently showed typical WE findings, with additional atypical sites in some nonalcoholic cases. Twelve patients improved with thiamine supplementation, while two were lost to follow-up. All pregnant patients had favorable obstetric outcomes. Conclusions WE is often underdiagnosed, especially in nonalcoholic patients, due to atypical presentations. Clinicians and radiologists should maintain a high index of suspicion for WE in patients with risk factors beyond alcohol use. Early diagnosis and treatment are critical to prevent irreversible neurological damage.
Keywords: chronic alcoholism; hyperemesis gravidarum; mri; nonalcoholic we; periaqueductal grey matter; thiamine deficiency; wernicke’s encephalopathy.
Copyright © 2025, B Chittaragi et al.
Conflict of interest statement
Human subjects: Informed consent for treatment and open access publication was obtained or waived by all participants in this study. Institutional Ethics Committee of JSS Medical College issued approval JSSMC/IEC/160525/45 NCT/2024-25. Animal subjects: All authors have confirmed that this study did not involve animal subjects or tissue. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures


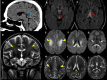

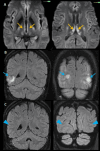


References
-
- Wernicke's encephalopathy revisited. Translation of the case history section of the original manuscript by Carl Wernicke 'Lehrbuch der Gehirnkrankheiten fur Aerzte and Studirende' (1881) with a commentary. Thomson AD, Cook CC, Guerrini I, Sheedy D, Harper C, Marshall EJ. Alcohol Alcohol. 2008;43:174–179. - PubMed
-
- Hyperemesis-gravidarum-induced Wernicke's encephalopathy: serial clinical, electrophysiological and MR imaging observations. Netravathi M, Sinha S, Taly AB, Bindu PS, Bharath RD. J Neurol Sci. 2009;284:214–216. - PubMed
-
- Comprehensive review of Wernicke encephalopathy: pathophysiology, clinical symptoms and imaging findings. Ota Y, Capizzano AA, Moritani T, Naganawa S, Kurokawa R, Srinivasan A. Jpn J Radiol. 2020;38:809–820. - PubMed
LinkOut - more resources
Full Text Sources
