Transgender-Affirming Hormone Therapies, QT Prolongation, and Cardiac Repolarization
- PMID: 40736733
- PMCID: PMC12311718
- DOI: 10.1001/jamanetworkopen.2025.24124
Transgender-Affirming Hormone Therapies, QT Prolongation, and Cardiac Repolarization
Abstract
Importance: Transgender women (assigned male at birth) usually take antiandrogens associated with estrogens (or are castrated) to induce feminization, whereas transgender men (assigned female at birth) take testosterone to induce masculinization. However, the cardiovascular outcomes of these gender-affirming hormone therapies (GAHTs) remain poorly studied.
Objective: To examine the association between GAHT intake and cardiac repolarization alterations on electrocardiography in transgender individuals.
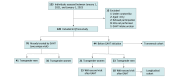
Design, setting, and participants: In this cohort study, data from a prospective cohort of adult transgender individuals from a single center in France were collected from January 1, 2021, to January 1, 2023. GAHT consisted of injectable testosterone in transgender men and transdermal estradiol with mostly oral cyproterone acetate as antiandrogens in transgender women.
Main outcomes and measures: Electrocardiographic features, including QTc, T-wave maximal amplitude (TAmp), and QT peak (QTp; distance between Q onset and T peak), were studied. Circulating sex hormones, including total testosterone, estradiol, progesterone, and gonadotrophins, were assessed concomitantly to electrocardiographic intake.
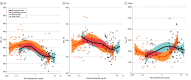
Results: In the overall cohort of 120 transgender individuals (mean [SD] age, 29.7 [11.9] years; 64 transgender men and 56 transgender women), mean (SD) QTc was similar between 35 transgender women receiving GAHT (406 [20] milliseconds) and 23 transgender men before GAHT (400 [16] milliseconds) but prolonged vs 41 transgender men receiving GAHT (378 [19] milliseconds) (P < .001) or 21 transgender women before receiving GAHT (384 [21] milliseconds) (P < .001). The start of GAHT in 15 transgender women was associated with increased QTc (mean [SD], 20 [12] milliseconds vs before receiving GAHT; P < .001) and decreased QTc in 18 transgender men (mean [SD], -17 [16] milliseconds vs before receiving GAHT; P < .001). No participant had a QTc greater than 480 milliseconds or QTc change greater than 60 milliseconds after the start of GAHT in this study. Nonlinear mixed models (eg, integrating age, calcemia, relevant circulating hormones levels, and torsadogenic drug intake) showed that QTc was associated with total testosterone in transgender men (mean [SD] estimate, -1.6 [0.6] ms/ng/mL; P = .007) and prolactin (mean [SD], 0.4 [0.1] ms/ng/mL; P < .001). In transgender women, QTc was associated with total testosterone (mean [SD] estimate, -3.5 [0.8] ms/ng/mL; P < .001). Variation of QTp and TAmp observed after the start of GAHT and associated hormonal alteration were globally associated with those observed with QTc, although in opposite directions for transgender women and transgender men.
Conclusions and relevance: In this cohort study, testosterone use in transgender men was associated with QTc and QTp shortening and increased TAmp. Androgen deprivation in transgender women was associated with opposite observations. The magnitude of QTc sexual dimorphism seen in cisgender adults was also observed in the transgender population. This work highlights that potential GAHT effects on cardiac repolarization warrant attention in the exponentially increasing transgender population, which is often exposed to coprescribed drugs prolonging QTc and at risk of TdP.
Conflict of interest statement
Figures

Comment in
References
-
- Streed CG Jr, Beach LB, Caceres BA, et al. ; American Heart Association Council on Peripheral Vascular Disease; Council on Arteriosclerosis, Thrombosis and Vascular Biology; Council on Cardiovascular and Stroke Nursing; Council on Cardiovascular Radiology and Intervention; Council on Hypertension; and Stroke Council . Assessing and addressing cardiovascular health in people who are transgender and gender diverse: a scientific statement from the American Heart Association. Circulation. 2021;144(6):e136-e148. doi: 10.1161/CIR.0000000000001003 - DOI - PMC - PubMed
-
- Caceres BA, Streed CG Jr, Corliss HL, et al. ; American Heart Association Council on Cardiovascular and Stroke Nursing; Council on Hypertension; Council on Lifestyle and Cardiometabolic Health; Council on Peripheral Vascular Disease; and Stroke Council . Assessing and addressing cardiovascular health in LGBTQ adults: a scientific statement from the American Heart Association. Circulation. 2020;142(19):e321-e332. doi: 10.1161/CIR.0000000000000914 - DOI - PMC - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

